Abstract
Objectives: To measure the rate of union in patients with pseudoarthosis of the scaphoid, treated with trapezoidal bone grafting as outlined by Fernandez and 1 of 3 methods of internal fixation and to compare unions versus nonunions and potential predictors of union to determine if associations exist.
Design: A retrospective radiologic study of scaphoid pseudoarthroses.
Setting: Division of Orthopedic Surgery, Ottawa Hospital, General Site, a tertiary care facility.
Patients: Thirty-four patients with nonunion of scaphoid fractures, treated between 1990 and 1997, with an average follow-up of 19.8 months.
Interventions: Trapezoidal bone grafting and internal fixation with Kirschner (K) wires, an AO cannulated screw or a Herbert screw.
Outcome measures: The time to union of scaphoid pseudoarthroses and predictors of union, including the classification, location of pseudoarthrosis, type of internal fixation and length of bone graft.
Results: The results showed a correlation between the classification and location of the fracture as determined radiologically, and the outcome. There was no correlation between the type of internal fixation used and the outcome, or between the length of the bone graft and the outcome. Twenty-three patients had radiologically demonstrated union after a mean time of 8.2 months; 16 of 24 patients achieved successful union when treated with K-wire implants, after a mean time of 7.2 months.
Conclusions: Trapezoidal bone grafting and internal fixation with K wires is a practical technique, classification and location of the fracture notwithstanding. Time to union is long, and the results may be unpredictable. Use of K wires for internal fixation presents the clinician with an alternative to fixation with either the AO cannulated screw or the Herbert screw, and has the advantages of cost, ease of insertion and accessibility. This method may therefore be the treatment of choice in developing countries. Resection of the area of pseudoarthrosis must include all fibrous tissue and sclerotic bone. The length of graft, within the parameters of this study, did not affect the outcome.
Nonunited fractures of the scaphoid have a variable healing rate after bone grafting and internal fixation. The rate of union depends on the site of the pseudoarthrosis,1,2 its classification1 and perhaps the type of internal fixation. 3 The objective of this retrospective study of patients with symptomatic pseudoarthroses of the scaphoid who were treated between 1990 and 1997, was to measure the rates of union of the scaphoid after treatment by the trapezoidal method of bone grafting.4 Our secondary objectives were to determine the association between several predictors of the rate of union: location and classification of the pseudoarthrosis, the location and dimensions of the bone graft and the type of fixation used.
In 1988, Stark and colleagues5 achieved an overall 97% union rate in 106 cases when bone grafting and Kirschner (K) wires (Zimmer Inc., Dover, Ohio) were used to treat nonunions of the waist of the scaphoid (Fig. 1). Barton,3 in 1997, observed radiographic union in 47% (15 of 32) of of nonunited scaphoid fractures after wedge grafting and implantation of K wires. Daly and associates6 reported excellent results with the use of Herbert (Zimmer Inc.) screws and grafting. Fifteen nonunited fractures of the waist were classified as D2 or D32,7,8 and in 14 (93%) of them union was successfully achieved. Herbert and Fisher7 described 71 patients with type D2 fractures who were treated with Herbert screws. Union was achieved in 42 (59%) of them. The average time to radiologic union was reported to be approximately 4 months.5,6 The time to union did increase as the classification of the pseudoarthrosis advanced from D1 through D4. Since the objective of bone grafting and internal fixation is not only to promote successful union but to prevent further degenerative changes and correct carpal collapse, the difference in times to union is not as critical as the outcome itself.
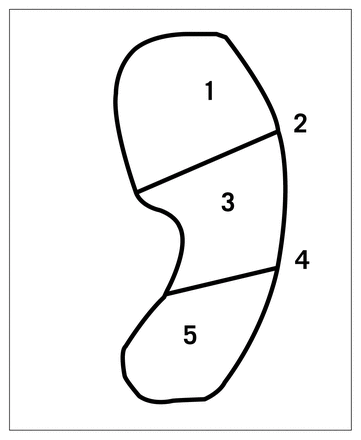
A schematic diagram of the scaphoid showing the classification of fracture sites. 1 = the distal pole, 2 = the junction between the distal pole and the waist, 3 = the waist, 4 = the junction between the waist and the proximal pole, 5 = the proximal pole.
Patients and Methods
Over the past 7 years (1989 to 1997) 44 wrists in 42 patients (39 men), were treated for nonunion of the scaphoid. The mean interval between the known causative injury and surgery was 41.1 months (range from 2 months to 17 years). The mean age at the time of surgery was 26.6 years (range from 13 to 45 years). The cause, in the majority of cases, was a fall on an outstretched hand. Seven patients had undergone previous surgical treatment; the remainder underwent conservative treatment or had no treatment at all.
Four of the 44 wrists had bone grafting only, and 6 wrists were treated through a dorsal approach. These results are not analysed in the study. The remaining 34 wrists were all managed by resection of the pseudoarthrosis, insertion of a trapezoidal, iliac crest corticocancellous graft as described by Fernandez4 and internal fixation by 1 of 3 methods. This was accomplished through a volar approach. Fixation was achieved with K wires in 24 wrists, a Herbert screw in 5 wrists and an AO cannulated screw (AO Synthes, Schweiz, Switzerland) in 5 wrists.
Radiographs were reviewed for decisive patterns of pseudoarthrosis, including cystic changes, sclerosis at the fracture site, dorsal intercalated segmented instability (DISI) with carpal collapse, and shortening of the scaphoid (Fig. 2). The presence of avascular necrosis of the proximal pole and radiocarpal osteoarthritic changes were also noted. Criteria for inclusion in the study were radiographs taken at least 3 months postoperatively and a declared final status of union or nonunion. Radiographs of the opposite wrist were not taken at the time of injury or diagnosis unless it was deemed necessary. Definitive union was considered to have occurred when bony trabeculae crossed the grafted pseudoarthrosis from the proximal to distal pole in 2 of the 4 scaphoid views.6 When there was evidence of movement of the implanted device, seen in the radiographs as a radiolucent effect, the fracture was considered nonunited. Cases of indeterminate union were declared as nonunions if no further radiographs were available for consideration. If union of the pseudoarthrosis occurred at less than 1 year, and at this time the patient’s status was considered finalized, the results were included in the study because the outcome was recognized as successful.
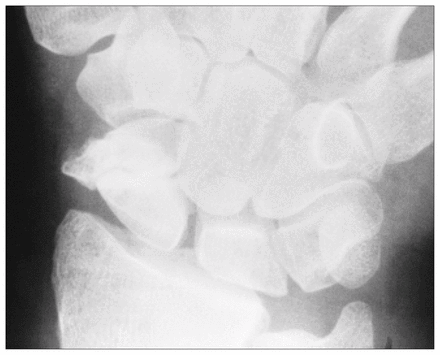
Radiograph of the wrist of a 29-year-old man with advanced pseudoarthrosis of the scaphoid (class D3). Note the loss of anatomic height of the scaphoid. Sclerosis at the margins of the fracture and evident movement at the site of the fracture are typical markers of the “false joint.”
Fracture classification, encompassing the degenerative changes characterizing pseudoarthrosis, was determined according to Herbert’s staging system,2,6–8 and the length of the graft was measured at its longest aspect. Carpal collapse is a malalignment often associated with pseudoarthrosis of the scaphoid.3,4 For the purposes of this study, preoperative radiographic analysis of the collapse of the affected hand was necessary to clarify the classification of the pseudoarthrosis. Collapse was determined postoperatively by calculating the revised carpal height ratio (RCHR) as described by Nattrass and colleagues.9
When determining the site of the fracture for the purposes of this study, we referred to other texts for a basis for classification of location (Fig. 1). The division of the scaphoid into 3 zones, namely the proximal pole, the waist and the distal pole, is standard1,7 although some studies differentiate between the distal two-thirds and the proximal pole of the scaphoid only.2
Operative Technique and Postoperative Management
The scaphoid is exposed volarly, as described by Russe.10 The hand and wrist are placed in dorsiflexion and deviated in an ulnar direction for optimal exposure of the scaphoid, and the proximal and distal fragments. A microsagittal saw is used to create 2 parallel resections on either side of the pseudoarthrosis. Fibrous tissue is curetted out, and any remaining cavity is packed with cancellous bone. Intraoperatively, the normal length of the scaphoid is judged by dorsiflexion and ulnar deviation of the carpus, bearing in mind that the distal pole of the scaphoid is attached to the scaphoidtrapezium-trapezoid joint and the proximal pole to the lunate by way of the scapholunate ligaments. The gap produced at the pseudoarthrosis after attaining this position equals the required size of the bone graft. The defect is measured, and a corresponding amount of iliac crest corticocancellous bone graft is introduced to the nonunion, as described by Fernandez4 and internally fixed. The wrist is put in a scaphoid cast for 2 weeks, then the sutures are removed and the wound is inspected. Thereafter, the wrist is immobilized until progressive healing and possible union are evident, or stable pseudoarthrosis persists. Once the cast is removed, heavy loading of the wrist is discouraged, and mobilization is recommended. In some cases physiotherapy is prescribed.
Follow-up was at 2 weeks and then monthly. Further follow-up was based on clinical and radiologic findings. Thereafter, the patient was seen only if complications arose. At every visit, radiographs were obtained. All data were compiled and analysed with use of the Statistical Package for the Social Sciences, version 6.
Results
The mean time of final radiologic follow up was 19.8 months. Twenty-three (68%) of the 34 pseudoarthroses united in a mean time of 8.2 months. The minimum time to radiographic union was 2 months, the maximum time was 26 months. Sixteen (67%) of 24 fractures, treated with K wires, achieved solid bony union in a mean time of 7.2 months. Two of 5 fractures fixed with a Herbert screw achieved solid union in a mean time of 12 months, and 4 of 5 fractures, treated with AO cannulated screws achieved solid union in a mean time of 4.4 months.
All patients underwent bone grafting by a single technique; however, since the method of internal fixation varied, comparison between the types of internal fixation was difficult due to small numbers. In our study, pseudoarthroses classified as D2 (pseudoarthrosis)2,6,8 and D3 (sclerotic pseudoarthrosis)2,6,8 and treated with K wires, achieved solid union in 8 of 10 cases. (Table I2,6,8). D2 and D3 pseudoarthroses fixed with a Herbert screw achieved a union in 2 of 3 cases and those fixed with an AO screw achieved solid union in 2 of 3 cases (Tables II and III). Nonunited fractures located in the waist of the scaphoid, regardless of classification, united in 9 of 11 cases fixed with K wires, 2 of 3 fixed with a Herbert screw and 2 of 2 fixed with an AO screw.
Union of the Scaphoid Achieved by Internal Fixation With Kirschner (K) Wires After More Than 3 Months’ Follow-up Related to Type of Fracture
Union of the Scaphoid Achieved by Internal Fixation With Herbert Screws After More Than 3 Months’ Follow-up Related to Type of Fracture
Union of the Scaphoid Achieved by Internal Fixation With AO Cannulated Screws After More Than 3 Months’ Follow-up Related to Type of Fracture
The mean graft length was 6.81 mm, ranging from 3 to 15 mm. To correct carpal collapse, some grafts were exceedingly large. For those who received grafts between 10 and 15 mm long, this represented at least one-third of the total length of the scaphoid. One patient who received a bone graft longer than 12 mm did not have a successful outcome, and 9 of 15 patients having a graft less than 6 mm long had successful union. Ten (77%) of 13 wrists with a defect 6.1 to 9.0 mm in size united and 4 of 5 wrists with a defect of 9.1 to 12.0 mm in size united. No correlation between graft dimensions and outcome was demonstrated. Due to the small number of patients involved, these results cannot be considered statistically significant. No other studies have considered the dimensions of the graft as a factor in the rate of union.
For the patients treated with K wires, a number of complications were observed radiologically: advancement into the radiocarpal joint space was seen in 1 case, an increase in avascularity of the proximal pole postoperatively was noted in another, increased resorption at the fracture site was demonstrated in 1 case and movement at the fracture site, illustrated by lucency bordering the wires, was observed in 1 case.
In 3 of the scaphoids fixed with a Herbert screw, there was evidence of screw movement, marked by lucency at the site of fracture. One of the Herbert screws became exposed, projecting into the radiocarpal joint space, another projected into the scaphotrapezial joint as a result of graft crumbling, yet there was eventually bony union (Fig. 3). One case involving an AO cannulated screw resulted in protrusion of the threads into the radiocarpal joint space and in a second case, distal advancement of the screw was noted.
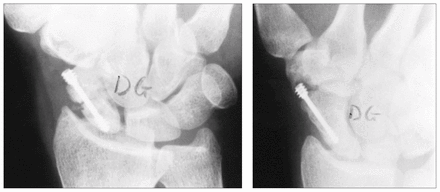
Radiographs of the wrist of a 25-year-old man illustrating placement of a Herbert screw (left) and subsequent collapse of the graft and protrusion of the screw head 2 years postoperatively (right). The pseudoarthrosis united 11 months after grafting. The Herbert screw was removed shortly after the second radiograph was obtained.
Discussion
As evidenced in earlier studies, the natural history of scaphoid fractures establishes that the rate of union depends on the location of the fracture: the more proximal the fracture, the less likely it is to unite.1,2 Initially, the usual division of the scaphoid into 3 equal zones seemed suitable. As more radiographs were examined, it became apparent that many fractures did not fall within the boundaries of the conventional divisions but crossed boundaries. For this reason, we added the junctions between the proximal pole and the waist and between the waist and the distal pole as distinct locations (Figs. 1 and 4). Ambiguity in defining location may result in an incorrect classification, thereby affecting the relationship between the rate of union and the location of the fracture. It may therefore be difficult to compare results of various studies.
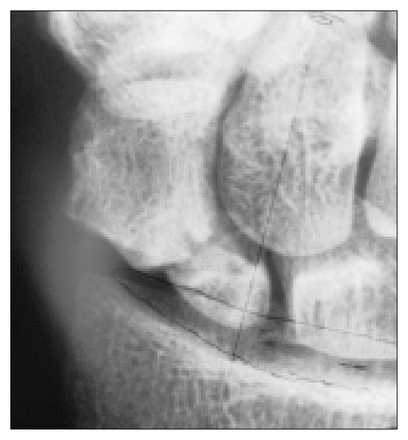
The location of this fracture illustrates the dilemma of fracture site classification. When measured, it does not lie within the boundaries of the waist or within the boundaries of the proximal pole. This nonunited fracture is classified as being on the junction separating the waist and the proximal pole.
In Filan and Herbert’s study,2 66% of D2 and 50% of D3 pseudoarthroses resulted in union after internal fixation with the Herbert screw and, given similar bone-grafting techniques, the rate of union in our study was comparable to that of our class D2 and D3 pseudoarthroses treated with K wires. The average time to radiologic union reported by Daly and associates6 and Stark and colleagues5 was approximately 4 months, and this was less than we experienced. The time to union did increase as the classification of pseudoarthroses advanced from D1 to D4. Since the objective of interpositional structural bone grafting and internal fixation is not only to promote successful union but to prevent further degenerative changes and correct for carpal collapse, the difference in times to union is not as critical as the outcome itself. Comparison between trapezoidal scaphoid bone grafting and the Russe technique may not be appropriate. Trapezoidal grafting is done when scaphoid length must be increased and a hump-back deformity corrected. The Russe technique may be used when striving to obtain union but not correct scaphoid external dimensions.
If the bone grafting technique was consistent across the studies, it follows that variable outcomes may be attributed to causes other than the technique. We found that the length of the graft did not have an effect on the outcome. However, the location of the graft and, similarly, the location of the original fracture (Table IV) both had an effect on the outcome: the more proximal the fracture, the less likely was union.
Comparison of the Rate of Union of Fractures and Location of the Fractures
The final predictor of union may be the method of internal fixation. As a result of small sample size, no evidence could be found of an association between the type of internal fixation and the time to union, or the type of internal fixation and the outcome (Table V); however, each method of internal fixation has its advantages and disadvantages.
Comparison of the Type of Internal Fixation and Location of the Fractu res
K wires provide an attractive alternative to the use of screws because they are inexpensive and they are easily accessible in developing nations. K wires have a greater ease of insertion, a shorter operative time and a minimum amount of dissection.11 Carter and associates11 documented that failure of paired parallel K wires in the mobilized scaphoid, in terms of force, rigidity and bending moments, is 3 times more likely to occur than in AO screws and Herbert screws. K wires provide relatively less compression across the fracture site than do AO cannulated screws and Herbert screws and have poor fragment purchase. K wires are subject to slippage as their strength relies on the wire–bone interface resisting the traction forces of the wires, and loose bone graft provides little support.11,12
When tested with an osteotomy model, AO cannulated screws offered greater compressive forces than Herbert screws, with no significant difference in bending moments.11 AO screws have the disadvantage of a prominent head, which can lead to damage of the cortex of the bone when compression is applied. Also, the head of the AO screw, which is relatively large compared with the scaphoid itself, remains extraosseous and intra-articular, possibly causing discomfort.13 One potential advantage of cannulated screws is their use in combination with a guide wire, increasing the accuracy of placement within the scaphoid.
Studies by Filan and Herbert2 and Daly and associates6 reported remarkable rates of union with use of the Herbert screw; however, Herbert screw fixation is the most technically demanding of the 3 conventional methods. The jig is cumbersome and extensive dissection is required, yet the screw is buried, has good compressive forces across the fracture site and is rigid.12 For these reasons, mobilization soon after surgery and soft-tissue healing are sometimes possible.
A disadvantage of both the Herbert and AO cannulated screws is the potential collapse of corticocancellous bone at the shank of the screw (Fig. 3). If collapse occurs, what was once compression now becomes a lack of compression and the well-fixed terminal aspects of the fixation keep the fragments apart. As a result, the graft is not incorporated and persistent nonunion may be observed radiologically.
Based on historic information and our own experiences with bone grafting and internal fixation, the present treatment for scaphoid fracture pseudoarthrosis does not clearly favour one type of internal fixation, and successful results for pseudoarthrosis are still unpredictable. Successful union, when it occurs, is protracted.
Herbert screws are the most expensive of the implants, costing Can$148 each. An AO cannulated screw costs approximately Can$75 (price may vary slightly depending on size) and 2 K wires may be purchased for Can$14. In many situations worldwide, particularly in developing nations, surgical instrumentation may be limited and cost may be an issue. In this case, the use of grafting and K-wire fixation represents the simplest proven technique using widely available and inexpensive instrumentation.
Conclusions
The method of trapezoidal bone grafting outlined by Fernandez is a practical technique; however, achieving union is unpredictable. If and when radiographic union does occur, the process is protracted.
The time to union depends on the classification of the fracture and the site of the fracture and graft. According to Herbert’s staging system, the more advanced the problem, in terms of DISI, shortening of the scaphoid, carpal collapse and sclerosis, the less likely will the fracture heal effectively and efficiently. Further, the more proximal the site of the pseudoarthrosis (and hence the graft), the less likely it is that a reliable union can be achieved.
In this study, the time to union was independent of the method of internal fixation used, and the outcome was independent of the dimensions of the size of the defect and corticocancellous bone graft.
- Accepted August 30, 1999.