Primary hyperparathyroidism-induced brown tumour of the third metacarpal
The clinical history in this case was not particularly helpful in making the diagnosis and, indeed, the plain-film appearances of expansion and osteopenia would be in keeping with a number of lesions. A swelling in the neck may have suggested hyperparathyroidism, but biochemical results were essential for making the diagnosis. A brown tumour of primary hyperparathyroidism was confirmed pathologically after bone biopsy and parathyroidectomy.
Primary hyperparathyroidism is due to an intrinsic abnormality of the parathyroid glands. The cause is a parathyroid adenoma in 85% of cases, parathyroid hyperplasia and parathyroid carcinoma being the other causes. Typically, serum parathyroid hormone, calcium and alkaline phosphatase levels are elevated, with the serum phosphate level being decreased. Primary hyperparathyroidism is typically a disease of middle age. Women are affected three times more often than men.1 The incidence of primary hyperparathyroidism has increased recently, but clinically evident bone disease is less common than previously reported.2 Most patients are asymptomatic at the time of diagnosis. 1 Up to 10% of cases of primary hyperparathyroidism are hereditary, usually associated with multiple endocrine neoplasia type 1 and type 2 syndromes.1
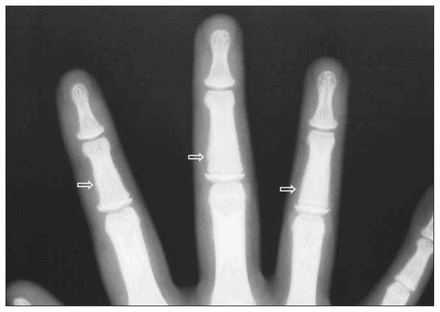
Radiologically, hyperparathyroidism commonly appears as nonspecific osteopenia, less commonly with pathognomonic subperiosteal bone resorption of the digits (Fig. 5), skull and long bones and uncommonly as a destructive brown tumour, as in this case.3 Other bone changes include bone softening, osteosclerosis and an erosive arthropathy. The deleterious effects are on cortical rather than on cancellous bone. These effects are characterized by increased bone turnover,1,2,4 which can cause diffuse uptake on isotope bone scanning, giving the appearance of a “superscan” (Fig. 6). The incidence of bone lesions in primary hyperparathyroidism is 25%–40%, with 20% of these being visible on radiographs. Brown tumours are commoner in primary (3%) than in secondary (2%) disease, but the prevalence of secondary disease means that brown tumours are more commonly found in association with it. Brown tumours are well defined, often expansile, solitary or multifocal lytic lesions,3 provoking little reactive bone formation. They may be diaphyseal, metaphyseal or rarely epiphyseal.3 They are benign slow-growing lesions, representing a reparative cellular process rather than a neoplastic process and typically undergo no further growth after removal of the parathyroid glands.5 Healing may lead to sclerotic foci or complete resolution. 3 In a minority of cases, if the cellular elements undergo necrosis, a bone cyst results that may persist.3
Plain radiograph of the fingers demonstrates extensive subperiosteal bone resorption of the phalanges (arrows).
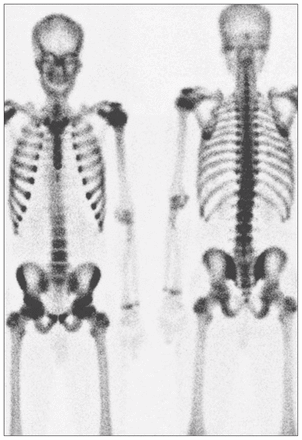
Isotope bone scan demonstraties the “superscan” appearance of primary hyperparathyroidism.
On computed tomography, attenuation of these lesions is in the range of blood, and fibrous tissue and fluid–fluid levels can be seen on magnetic resonance imaging.6 Brown tumours show increased uptake on isotope bone scanning and are most commonly found in the jaw, femur, pelvis and ribs.3
Histologically, these lesions are characterized by the presence of hemosiderin pigment deposits and osteoclastic giant cells arranged in groups and separated by richly vascularized fibrous tissue. Zones of recent and old hemorrhage are frequent, and surrounding bone shows increased osteoclastic resorption. It is the accumulation of hemosiderin that gives these lesions their characteristic colour and name. Differential diagnosis includes giant cell reparative granuloma, true giant cell tumour, aneurysmal bone cyst and cherubism, and on gross and histologic examination these entities can easily be confused.5,6 Multiple brown tumours may be mistaken for metastases, myeloma or histiocytosis.6 Hence, if the presenting complaint is that of a “bone tumour” and image interpretation fails to identify hyperparathyroidism, pathologic findings may be inconclusive, and the diagnosis may be overlooked.6 Treatment of these lesions requires surgical removal of the parathyroid glands. Preoperative localization tests include computed tomography, ultrasonography, magnetic resonance imaging and technetium-99m sestamibi scanning.1
When an expansile lytic bone lesion is encountered, clinical and biochemical parameters are important in differentiating brown tumours from other benign and malignant bone lesions. The presence of an abnormal plasma calcium level suggests an abnormal parathyroid hormone level, and further investigation is warranted; however, the absence of an elevated calcium level does not rule out hyperparathyroidism. In our case, a wide differential was initially suggested on the basis of the plain film findings. It was not until further examination revealed a neck mass that the diagnosis of a brown tumour was suggested. We conclude that biochemical and pathological correlations are required to diagnose this bone lesion and that any benign lesion rich in giant cells requires the exclusion of hyperparathyroidism.