Abstract
Background: Immigrants and refugees face unique challenges navigating the health care system to manage severe arthritis, because of unfamiliarity, lack of awareness of surgical options, or access. The purpose of this study was to assess total knee arthroplasty (TKA) uptake, surgical outcomes, and hospital utilization among immigrants and refugees compared with Canadian-born patients.
Methods: We included all adults undergoing primary TKA from January 2011 to December 2020 in Ontario. Cohorts were defined as Canadian-born or immigrants and refugees. We assessed change in yearly TKA utilization for trend. We compared differences in 1-year revision, infection rates, 30-day venous thromboembolism (VTE), presentation to emergency department, and hospital readmission between matched Canadian-born and immigrant and refugee groups.
Results: We included 158 031 TKA procedures. A total of 11 973 (7.6%) patients were in the immigrant and refugee group, and 146 058 (92.4%) patients were in the Canadian-born group. The proportion of TKAs in Ontario performed among immigrants and refugees nearly doubled over the 10-year study period (p < 0.001). After matching, immigrants were at relatively lower risk of 1-year revision (0.9% v. 1.6%, p < 0.001), infection (p < 0.001), death (p = 0.004), and surgical complications (p < 0.001). No differences were observed in rates of 30-day VTE or length of hospital stay. Immigrants were more likely to be discharged to rehabilitation (p < 0.001) and less likely to present to the emergency department (p < 0.001) than Canadian-born patients.
Conclusion: Compared with Canadian-born patients, immigrants and refugees have favourable surgical outcomes and similar rates of resource utilization after TKA. We observed an underutilization of these procedures in Ontario relative to their proportion of the population. This may reflect differences in perceptions of chronic pain or barriers accessing arthroplasty.
Total knee arthroplasty (TKA) is a successful procedure performed more than 75 000 times a year in Canada.1 Whereas the outcomes of this procedure are well documented, there has been limited evaluation of outcomes among immigrants and refugees.2 The population of Canada comprises approximately 23% immigrants, and the proportion of immigrants reaches nearly 30% in the province of Ontario.3 These proportions are among the highest of any country in the world.4 While this diversity is one of Canada’s strengths, it can present challenges for these patients and their health care providers.
The top countries of birth among immigrants to Ontario include India, China, and the Philippines.3 Immigrants from these countries may be more likely to have torsional deformities of the lower extremity, increased tibial bowing, and varus flexion contractures of the knee, which make TKA challenging and increase the risks for complications after surgery.5–9 Although new immigrants are typically healthier than their Canadian-born counterparts, this health advantage tends to decline as their years in Canada increase and they are vulnerable to chronic conditions such as osteoarthritis.10,11 Immigrants are also more likely to face challenges navigating the health care system secondary to barriers related to differences in language and health literacy.12–14 They may also differ in their beliefs about arthritis and the role of surgical treatment to alleviate pain and improve function.13,15 As such, despite a high prevalence of severe arthritis, immigrants may be more vulnerable to delayed presentation and reduced uptake of TKA, and may have a higher risk for complications or unsatisfactory outcomes after surgery.
It is important that the relation between immigration status and outcomes of total joint arthroplasty are evaluated in this growing and particularly vulnerable population. We hypothesized that immigrants may have worse outcomes owing to differences in baseline health status, social supports, and utilization of health care resources. The aims of this study were to assess surgical and resource utilization outcomes of a matched cohort of immigrants and refugees compared with Canadian-born patients after TKA and to identify the change, if any, in the proportion of TKAs performed on immigrants annually.
Methods
Study population
Our study cohort included adult patients (age ≥ 18 yr) who underwent a primary elective TKA over a 10-year period between Jan. 1, 2011, and Dec. 31, 2020. Patients with a residential postal code outside the province of Ontario at the time of surgery were excluded. Recipients of TKA were identified using a combination of surgeon billing claim fee codes for TKA and corresponding procedure codes on hospital discharge records. Patients were classified as either immigrant/refugee or Canadian-born/long-standing resident based on their status in the Immigration, Refugees and Citizenship Canada (IRCC) Permanent Resident Database. Those classified as immigrants and refugees included those who obtained permanent residency between Jan. 1, 1985, and May 31, 2017, (based on the most recent IRCC data available at the time of study) and second-generation immigrant children younger than 19 years who were born in Ontario to mothers who gained permanent residence in Ontario since 1985. We classified individuals born or living in Ontario who are not in the IRCC database as Canadian-born and long-term residents, although this would include immigrants and refugees who arrived in Ontario before 1985 or after May 2017, and those who initially immigrated to other Canadian provinces or territories and later moved to Ontario. The IRCC Permanent Resident Database captures approximately 90% of immigrants planning to settle in Ontario, with lowest rates of linkage among economic immigrants, those from eastern Asia, and immigrants older than 85 years.16,17
Data sources
The study cohort was identified from data housed at ICES, an independent, nonprofit research institute funded by the Ontario Ministry of Health (www.ices.on.ca). Administrative health care and demographic data were securely linked and analyzed at the individual level using unique encoded identifiers. We used physician service claims paid by the Ontario Health Insurance Plan (OHIP) and Canadian Institute for Health Information (CIHI) Discharge Abstract Database (DAD) to identify all patients who underwent TKA, as well as diagnostic information, including preoperative comorbidities and postoperative complications. The OHIP Registered Persons Database was used to obtain patient demographic information. We used the Postal Code Conversion File and Canadian census data to determine patients’ rurality index, Ontario Marginalization Index, and neighbourhood income quintile. The CIHI National Ambulatory Care Reporting System (NACRS) was used to identify patients who presented to an emergency department. Finally, we identified immigrants and refugees using the IRCC Permanent Resident Database, as described above.
Covariate and outcome definitions
We recorded patient demographic characteristics, including age, sex, and socioeconomic status, to compare characteristics between groups at baseline. We used the Ontario Marginalization Index, an adaptation of the Canadian Marginalization Index, to characterize patients’ socioeconomic status.18 This index comprises 4 dimensions: dependency (proportion of seniors, children, and unemployed), deprivation (fewer resources), ethnic diversity (proportion of immigrants or ethnic minorities), and residential instability (living alone, recently moved, average number of people per dwelling). Each dimension is categorized into 5 quintiles, arranged from least (first quintile) to most (fifth quintile) marginalized. This index has been evaluated and validated to be stable across time and geographic areas within Ontario.19 We used the Rurality Index of Ontario score to define whether a patient lives in a rural residence based on their primary address.20 The teaching status of the hospital in which the arthroplasty was performed was also analyzed.
The Deyo–Charlson Comorbidity Index for each patient was calculated using the comorbidities listed on hospital discharge abstracts in the 3 years preceding the index TKA.21,22 Patients were also defined as frail based on coding from the Adjusted Clinical Groups (ACGs) (Johns Hopkins ACG System Version 10.0) in the 2 years before surgery.23
We identified medical and surgical outcomes using physician billing codes and International Classification of Diseases, 10th Revision diagnosis codes on hospital discharge records. Number of venous thromboembolism (VTE) events, stratified into categories of deep vein thrombosis (DVT) and pulmonary embolism (PE), were recorded up to 30 days postoperatively. Surgical outcomes such as revision rate, infection rate, and death were recorded up to 1 year. Presentation to any emergency department within Ontario, as captured in the NACRS database, was limited to a period of 30 days from the time of TKA. Readmission to hospital, also within 30 days, was captured in the CIHI DAD. Length of hospital stay (LOS) in days was recorded as date of admission to discharge date, with same-day discharge counted as an LOS of 0 days.
Statistical analysis
Comparisons between baseline characteristics of groups were made using standardized differences, as this test is independent of sample size and we had large and unbalanced cohort sizes.24 Standardized differences greater than 0.10 are generally considered a meaningful difference between groups.25
Immigrant and refugee, and Canadian-born TKA recipients were matched 1:1 on age, sex, Deyo–Charlson Comorbidity Index score, and year of surgery. Univariate comparisons were made between patient groups, immigrant or Canadian-born, using the McNemar test to determine differences in outcome events. We analyzed the change in the proportion of TKAs that were performed among immigrants over the 10-year data period using the Cochran–Armitage test for trend. The type I error probability was set to 0.05 for all analyses.
Ethics approval
Use of data for this project was authorized under section 45 of Ontario’s Personal Health Information Protection Act and does not require review by a research ethics board.
Results
Over the study period, 158 031 TKA procedures occurred, 11 973 (7.6%) among patients in the immigrant and refugee group and 146 058 (92.4%) among patients in the Canadian-born group (Appendix 1, Figure S1, available at www.canjsurg.ca/lookup/doi/10.1503/cjs.013723/tab-related-content). A significantly greater proportion of patients in the immigrant group who underwent TKA were female (70.7% v. 60.6%). There were no significant differences in the presence of preoperative comorbidities between groups. There were differences between groups in all dimensions of the Ontario Marginalization Index; immigrant patients were more likely to be from areas with lower rates of dependency, higher rates of deprivation, higher rates of diversity, and lower rates of household instability. Overall, immigrant and refugee patients who underwent TKA were from neighbourhoods with lower income quintiles and were less likely to live in rural areas than Canadian-born patients. Immigrant and refugee patients were less likely to have their TKA performed at a teaching hospital (Table 1).
Baseline differences in demographic characteristics, comorbidity, and socioeconomic status between Canadian-born and immigrant patients undergoing total knee arthroplasty
Proportion of TKAs performed among immigrants and refugees
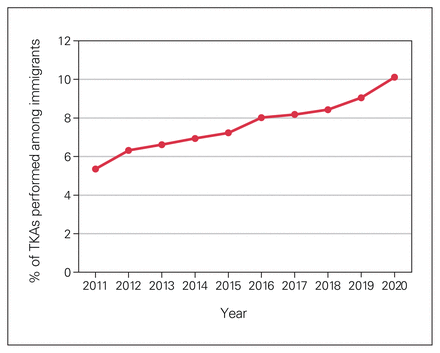
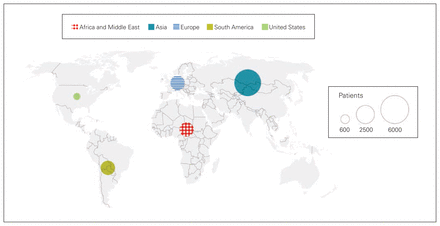
Over the 10-year study period, the percentage of TKAs performed among immigrants and refugees increased from 5.4% to 10.1% (p < 0.001) (Figure 1). Most of the patients who immigrated to Ontario and underwent TKA arrived from the continent of Asia (n = 6476, 54.2%). This was followed by South America and the Caribbean (n = 1752, 14.7%), Europe (n = 1724, 14.4%), and then Africa and the Middle East (n = 1657, 13.9%) (Figure 2). Most immigrants undergoing TKA had been in Ontario for more than 10 years (80.7%), with very few receiving a TKA during their first 5 years in Ontario (0.8%).
Percentage of total knee arthroplasty (TKA) procedures performed among immigrants in Ontario, by year.
Continent of birth for immigrants who underwent primary total knee arthroplasty in Ontario.
Patient outcomes
The final matched cohort included 11 948 patients in each study group, with 99.8% of the immigrant and refugee group retained. After matching, there were no significant differences between the immigrant and refugee group and the comparator group in terms of age, sex, comorbidities, or year of surgery (standardized differences were all < 0.1) (Appendix 1, Table S1). Immigrants and refugees had a lower revision rate (p < 0.001), infection rate (p < 0.001), and mortality rate (p = 0.004) at 1 year than patients born in Canada. The incidence of intraoperative complications was also lower among immigrants and refugees (p < 0.001). There were no significant differences in 30-day VTE rates between groups (Table 2).
Surgical and medical outcomes after primary total knee arthroplasty, by group
There was no significant difference in postoperative hospital LOS between groups (p = 0.07). Immigrants and refugees had lower rates of 30-day presentation to the emergency department after TKA (p < 0.001); however, there was no difference in rates of hospital readmission between groups (p = 0.2). For those in both groups who did present to the emergency department or were readmitted, there was no difference in the average time to these events. Immigrants and refugees were more likely to be discharged to a rehabilitation facility after TKA than matched nonimmigrants (p < 0.001) (Table 3).
Hospital resource utilization following primary total knee arthroplasty by group
Discussion
We found that immigrants and refugees who underwent TKA in Ontario had better surgical outcomes, in terms of lower complication rates, than matched Canadian-born or long-term residents. This included lower rates of revision, infection, and death at 1 year. Moreover, immigrants were less likely to present to the emergency department in the 30 days after their TKA procedure. This may have been partially owing to the greater proportion of immigrant patients discharged to a rehabilitation facility after their TKA, increasing the supports received postoperatively.
Studies evaluating outcomes of immigrants after total hip and knee arthroplasty from Sweden and the United States have not identified differences in revision rates with their native population.2,26 However, the immigrant populations and health care systems in those countries differ significantly from those in Canada, which may explain the differences seen in this study.27,28 Moreover, the previous study evaluating TKA outcomes identified patients primarily by the proportion of immigrants in their neighbourhood rather than at a patient level.26 By grouping patients and evaluating postsurgical outcomes at the population level rather than at an individual level, the effect can be significantly masked or confounded.
We identified that immigrants accounted for about 10% of TKA procedures performed in Ontario in 2020. This percentage nearly doubled over the 10-year study period. Although a cause for this increase cannot be determined, it may be due to an increase in the proportion of immigrants in the population over this time, as most immigrants had their TKA after being in Canada for longer than 10 years. This increase may also have been due to increased hospital funding in regions with higher immigrant populations.29 Although a direct analysis of TKA utilization is not possible as baseline rates of end-stage knee arthritis in each group are unknown, it is known that 30% of the population of Ontario are immigrants, a 3-times larger proportion of the population than their TKA utilization rate. However, this population is younger than the Canadian-born population, making direct calculation of surgery utilization impossible at the population level with available data.
Other countries have shown that immigrants may experience barriers to accessing timely arthroplasty care compared with long-term residents.13,30 This may be due to differences in patient preferences or attitudes toward surgery, surgeon’s perceptions of surgical risk, socioeconomic or language differences, or lack of health literacy.31–33 A review performed by Park and colleagues identified language proficiency and education level as the most significant factors determining an individual immigrant’s health literacy level.31 Despite these barriers, which may have caused immigrants to present later, at a more advanced stage of osteoarthritic disease, our study showed that their postoperative outcomes are equivalent or superior to those of matched Canadian-born patients. However, lower levels of health literacy among immigrants could also contribute to superior surgical outcomes and lower 30-day rates of emergency department presentation after TKA if patients are less likely to seek care for postoperative pain or complications. Other possible explanations include differences in patient selection or unmeasured patient characteristics, such as body mass index or severity of arthritis. However, the exact cause is difficult to elucidate given the observational nature of the study.
Limitations
In our study, we evaluated the effect of immigration status on outcomes after TKA at an individual level using linked health administrative and Canadian databases. Our study evaluated only immigrants landing in Ontario. However, Ontario’s immigrant population is large and diverse, including approximately 50% of immigrants to Canada, which is likely to improve the generalizability of our findings. A main limitation of this study is that we were able to identify only TKA recipients and not patients experiencing knee osteoarthritis. This limited the analysis for access to arthroplasty care to comparing the rate of TKA in immigrants to the provincial average, which may not accurately represent the need for TKA. Information regarding patient body mass index and arthritis severity was not available; however, we found no significant difference in patient age, sex, or comorbidities. Additionally, with administrative data there is a potential to underestimate the incidence of complications, as the diagnostic codes used may be poorly sensitive. However, this is more likely to be an issue for complications requiring outpatient management. Finally, the follow-up for surgical outcomes of these patients was limited to 1 year postoperatively. While this was consistent among all included patients, longer-term revision rates in this cohort are unknown.
Conclusion
Despite having low utilization rates of TKA, immigrants and refugees to Ontario, Canada, have lower rates of surgical complications, revision, and infection at 1 year than patients born in Canada. Immigrants and refugees were also less likely to present to the emergency department or be readmitted to hospital than their Canadian-born counterparts. Despite immigrants representing potentially more challenging surgical cases, our findings suggest that TKA in this patient population is relatively safe. Further research is needed to better understand the perceptions and obstacles immigrants experience regarding arthroplasty surgery.
Acknowledgements
The authors thank IQVIA Solutions Canada for use of its Drug Information File. They also thank the Toronto Community Health Profiles Partnership for providing access to the Ontario Marginalization Index.
Footnotes
Competing interests: J. Michael Paterson reports research funding from Arthritis Society Canada and the Canadian Institutes of Health Research. No other competing interests were declared.
Contributors: Bheeshma Ravi contributed to the conception and design of the study and acquisition of data, and all authors contributed to the analysis and interpretation of data. Johnathan Lex drafted the manuscript, which all authors revised. All authors gave final approval of the version to be published and agreed to be accountable for all aspects of the work.
Funding: This study was supported by grant funding from the Arthritis Society. Jessica Widdifield is supported by the Holland Chair in Musculoskeletal Clinical Research.
Disclaimer: This study was supported by ICES, which is funded by an annual grant from the Ontario Ministry of Health and the Ministry of Long-Term Care. This study also received a strategic operating grant from the Arthritis Society. Parts of this material are based on data and information compiled and provided by the Canadian Institute for Health Information, the Ontario Ministry of Health, and Immigration, Refugees and Citizenship Canada current to May 2017. The study also used data adapted from the Statistics Canada Postal CodeOM Conversion File, which is based on data licensed from Canada Post Corporation, and/or data adapted from the Ontario Ministry of Health Postal Code Conversion File, which contains data copied under licence from Canada Post Corporation and Statistics Canada. The analyses, conclusions, opinions, and statements expressed herein are solely those of the authors and do not reflect those of the funding or data sources; no endorsement is intended or should be inferred.
- Accepted March 25, 2024.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/