Abstract
Background: The use of intraoperative diuretics, such as furosemide or mannitol, during kidney transplantation has been suggested to reduce the rate of delayed graft function (DGF). The evidence base for this is sparse, however, and there is substantial variation in practice. We sought to evaluate whether the use of intraoperative diuretics during kidney transplantation translated into a reduction in DGF.
Methods: We conducted a cohort study evaluating the use of furosemide or mannitol given intraoperatively before kidney reperfusion compared with control (no diuretic). Adult patients receiving a kidney transplant for end-stage renal disease were allocated to receive furosemide, mannitol, or no diuretic. The primary outcome was DGF; secondary outcomes were graft function at 30 days and perioperative changes in potassium levels. Descriptive and comparative statistics were used where appropriate.
Results: A total of 162 patients who received a kidney transplant from a deceased donor (either donation after neurologic determination of death or donation after circulatory death) were included over a 2-year period, with no significant between-group differences. There was no significant difference in DGF rates between the furosemide, mannitol, and control groups. When the furosemide and mannitol groups were pooled (any diuretic use) and compared with the control group, however, there was a significant improvement in the odds that patients would be free of DGF (odds ratio 2.10, 95% confidence interval 1.06–4.16, 26% v. 44%, p = 0.03). There were no significant differences noted in any secondary outcomes.
Conclusion: This study suggests the use of an intraoperative diuretic (furosemide or mannitol) may result in a reduction in DGF in patients undergoing kidney transplantation. Further study in the form of a randomized controlled trial is warranted.
Kidney transplantation has provided decades of successful treatment for end-stage renal disease. Delayed graft function (DGF) is a condition defined in the modern era as a requirement for dialysis within the first week of receiving a kidney transplant and is largely attributed to ischemia–reperfusion injury (IRI).1 Ischemia–reperfusion injury stems from subcellular injury via generation of free radicals leading to acute tubular necrosis, cell swelling, reduced glomerular filtration, and potentially premature renal graft failure.1 Delayed graft function is associated with a longer stay in hospital and rejection; intervention to attenuate this process may reduce the costs of transplantation and improve patient outcomes.1
Efforts to avoid DGF have been approached through several forms of intervention. Moderate hydration protocols, pulsatile machine perfusion, minimization of warm and cold ischemia time, antibody-based induction immunosuppression, and use of intraoperative diuretics have all been incorporated into renal transplantation protocols to minimize the risk of DGF.1–4
The literature does not provide clear guidance as to whether or not intraoperative diuretics should be used. The rationale for the use of intraoperative diuretics stems from early animal studies that suggested these agents could minimize the deleterious effects of IRI.5,6 However, clinical studies to support the efficacy of diuretics in renal transplant are limited. In fact, there are some data to suggest that intraoperative diuretics may cause harm to patients by altering the vascular expansion and function of the kidney.7 In parallel, a recent trial of intraoperative diuretics in patients undergoing partial nephrectomy demonstrated no clear benefit for the use of mannitol in preserving renal function.8 Despite the lack of clear evidence for or against the use of intraoperative diuretics, a recent survey of Canadian transplant surgeons showed substantial variation in their use at the time of kidney transplantation.9 The lack of robust clinical evidence to inform the use of intraoperative diuretics justifies formal study of this issue.10,11
We sought to further examine the role these agents may play in kidney transplant outcomes with a focus on perioperative graft function. We hypothesized that the rates of DGF would not differ when either mannitol, furosemide, or no diuretic was given intraoperatively.
Methods
We conducted a cohort study of kidney transplant recipients at a single institution between March 2018 and August 2020 in which we examined all recipients of a single-kidney transplant from a deceased donor (neurologic determination of death [NDD] and donation after circulatory death [DCD]). We excluded patients who received transplants from living donors, those who received simultaneous liver and kidney transplants, and those younger than 18 years.
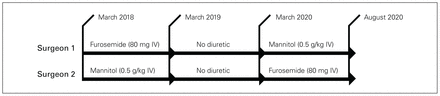
There were 3 phases of enrolment in the study. From March 2018 to March 2019, 2 surgeons altered their intraoperative practice to include the exclusive administration of either mannitol or furosemide. One surgeon was assigned to the mannitol arm (0.5g/kg of mannitol intravenously [IV]) and the other to the furosemide arm (80 mg of furosemide IV). Diuretic was given within 30 minutes before vascular unclamping. The 2 surgeons performed the transplant operation in a similar fashion over time, with no other changes to intraoperative protocols. From March 2019 to March 2020, both surgeons omitted intraoperative diuretic usage in patients (the control group). To account for the interaction between surgeon and diuretic in the initial phase, from March 2020 to August 2020, the 2 surgeons reinitiated diuretic use but crossed over in their assigned diuretic (Figure 1).
Schematic of study crossover design by surgeon and diuretic type. IV = intravenous.
All patients followed our institutional kidney transplant care pathway. The induction agent, either basiliximab or anti-thymocyte globulin in conjunction with methylprednisolone, was determined by the attending nephrologist on the basis of immunologic risk. Postoperative imunosuppressive therapy consisted of oral tacrolimus (once daily dosing), mycophenolic acid, and prednisone. Intraoperatively, systolic blood pressure was maintained at 110 mm Hg or greater before unclamping of the anastomosis using crystalloid solution or vasopressors. Postoperative fluid was administered per protocol using crystalloid solution titrated to central venous pressure during the first 24 hours with concomitant replacement of urine output during the first 48 hours. Fluid administration after 48 hours was adjusted on the basis of clinical assessment of volume status, oral intake, and urine output by the nephrology team, who did not have any prior knowledge of the intraoperative diuretic used. Routine postoperative Doppler ultrasonography was conducted on day 1 to document baseline allograft perfusion and resistive indices, with subsequent ultrasonography done for cause. Foley catheters were left in place for 4–5 days after surgery.
Ethics approval was obtained from the Western University and Lawson Health Research Institute Research Ethics Board (no. 112876). Recipient and relevant donor demographic and intraoperative data were collected. The primary outcome was the incidence of DGF, defined as requiring dialysis within 7 days of transplantation. Secondary outcomes included renal function at day 30 and change in potassium levels from the time of the immediate preoperative bloodwork to the immediate postoperative period. Subgroup analysis stratified by type of deceased donor (NDD or DCD) was also performed, and a sensitivity analysis was performed in which we pooled data for patients in whom any diuretic was used and compared them with data for patients in whom no diuretic was used.
Statistical analysis
A sample size calculation was performed using G*Power version 3.1.9.3. After setting the power at 90% and an α of 0.05, assuming a moderate effect size of 0.30 for a χ2 analysis with 2 degrees of freedom, we determined the minimum sample size to be 141. Data analysis was performed using SPSS version 26.0. Demographic data were compared between the 3 groups (control, furosemide, mannitol). Assumptions of normal distribution of continuous variables were tested with Kolmogorov–Smirnov testing and when appropriate, analysis of variance with Bonferroni post hoc testing was used for assessing differences in baseline data between groups; Kruskal–Wallis testing was used to compare groups when homogeneity of variance was rejected. Analysis of covariance was utilized to assess for differences in potassium levels postoperatively with the preoperative potassium level as the covariate of interest. The primary outcome of the study was rates of DGF and was assessed by χ2 analysis comparing the proportion in each group experiencing DGF. We also used χ2 testing for comparisons of categorical demographic data. Subsequently, we analyzed adjusted standardized residuals to distinguish differences between the individual groups. In our sensitivity analysis of pooling of any diuretic, unpaired t tests and Mann–Whitney U tests were used when appropriate to compare the 2 groups. Risk of DGF was assessed with a logistic regression model considering diuretic choice while controlling for donor type (NDD or DCD) and expanded criteria donor status. Restricting to these 3 factors allowed for increased stability of estimates given our sample size. The α was set at 0.05, and all analyses were 2-tailed.
Results
A total of 162 patients were enrolled, with 57 in the control group, 48 in the furosemide group, and 57 in the mannitol group. All enrolled patients were included in the analysis. In the control group, 1 patient died within 7 days of transplantation with a graft in situ (but with DGF). One patient required allograft nephrectomy on postoperative day 1 for arterial thrombosis and plaque rupture, and another patient required allograft nephrectomy on postoperative day 2 for arterial thrombosis related to a previously documented hypercoagulable state: these were deemed primary nonfunction but not counted as DGF. Table 1 summarizes the characteristics of our recipient population. In terms of the continuous variables outlined, the 3 groups were well balanced with respect to patient demographic factors. Recipient age, body mass index, anastomosis time, and preoperative potassium levels satisfied assumptions of normality, while cold ischemic time (CIT), calculated panel reactive antibody (cPRA%), and Class I and Class II PRA did not. Warm ischemic time (WIT) for kidneys from DCD donors was longer in the mannitol group (51 min compared with 33 min and 30 min in the furosemide and control groups, respectively). Our institution defines WIT in a DCD donor as the time from withdrawal of life support to organ flush. The frequency of DCD kidneys among the groups was not significantly different.
Baseline patient characteristics
The rate of DGF in the entire cohort was 31%, with a 58% rate of DGF in the recipients of DCD grafts and 17% in recipients of NDD grafts. In our analysis of the primary outcome, we found that the difference in the rates of DGF among the 3 groups approached statistical significance (Table 2). The Cramér V for estimation of effect size on the difference in DGF rate was 0.19. We performed a sensitivity analysis comparing DGF rates when any diuretic was used versus none. Any diuretic use was associated with an odds ratio [OR] of 2.10 (95% confidence interval [CI] 1.06–4.16, 26% v. 44%, p = 0.03) where the OR refers to freedom from DGF. However, when donor type was unpooled, there was no significant difference in DGF between patients who received diuretics and those who did not for either NDD grafts (23% v. 14%, respectively) or DCD grafts (68% v. 50%, respectively).
Renal functional parameters stratified by diuretic use
The results for secondary outcomes are shown in Table 2. None of these measures significantly varied among the 3 groups. Specifically, the rates of rejection as an underlying cause of DGF were not different, and the indications for dialysis in the first week after transplant were similar.
Table 3 summarizes the rate of DGF further stratified by donor type and shows that although patients with DCD kidney transplants experienced higher rates of DGF, the use of diuretics did not lead to significant differences in DGF rates. Table 4 summarizes the outcome data when restratified by any diuretic (furosemide or mannitol) compared with no diuretic. Delayed graft function was significantly less frequent when any diuretic was administered than when none was administered.
Delayed graft function stratified by donor type and diuretic usage
Comparison of renal functional parameters for patients who received any diuretic and those who received none (control)
Discussion
Intraoperative diuretic use in renal transplantation is a legacy practice based on limited data from an earlier era.1,5,10,12 The impact of intraoperative diuretics, most commonly mannitol and furosemide, on renal function preservation after kidney transplantation has been poorly characterized in the literature.1,5,10,12 In this study, we sought to determine whether intraoperative diuretics had any effect on DGF following transplant. The rate of DGF in our population was 31% overall, but it varied markedly by donor type, with a 58% rate of DGF in patients who received DCD kidneys, while those who received NDD kidneys had a 17% rate of DGF. These rates are in keeping with other published results.2,11,13
This study demonstrates that the rate of DGF is lower when an intraoperative diuretic (furosemide or mannitol) is used than when no diuretic is used. This was a clinically significant finding with an OR for freedom from DGF of 2.10 (26% v. 44%, diuretic v. control, p = 0.03). Interestingly, use of neither mannitol nor furosemide alone was associated with a significant reduction in DGF. Similarly, the reduction in DGF with diuretic usage was not significant when we analyzed the NDD and DCD subgroups individually. We have no clear explanation for these findings. It is possible this represents an issue with sample size, as a statistically significant difference was detected only when data from patients who received diuretic were pooled, thereby increasing the power of this sensitivity analysis. A similar finding arose when we analyzed specific donor types (NDD v. DCD) in that the pooled cohort demonstrated a significant difference but the smaller subgroups did not. There was a higher number of DCD donors in the control group. Although this difference did not reach statistical significance, the higher number of DCD donors may have influenced the rate of DGF when we compared the pooled diuretic groups. Alternatively, the lack of significant difference in DGF observed among the 3 groups may be a consequence of the nature of data collection in a prospective observational study rather than a randomized controlled trial. Interestingly, WIT was statistically longer for DCD donors in the mannitol group than in the control or furosemide group, but there was still a trend toward lower DGF rates with diuretics overall. Warm ischemic time during the DCD withdrawal process creates added periods of ischemia thought to predispose DCD kidneys to a greater severity of IRI and higher rates of DGF after transplant. Regardless, the reduction in DGF with any diuretic administration is an interesting finding that warrants further study.
There is a biologic basis for the beneficial effects of both furosemide and mannitol. Mannitol, a metabolically inert sugar alcohol, remains largely in the extracellular space and is excreted unchanged into the urine.14 Mannitol is purported to have several effects in the kidney, including diuresis, decreased renal vascular resistance, and changes in cortical and medullary blood flow with increased global renal flow.12,15,16 Mannitol is also thought to scavenge free radicals. These physiologic mechanisms have been demonstrated in animal studies.17 Bipat and colleagues demonstrated in a rabbit model of hypoxic kidneys that mannitol preserved diuresis and creatinine clearance with attenuation of the increased tubular pressure that was seen in hypoxic kidneys in which mannitol was not administered.6
Clinical studies examining mannitol in kidney transplant have previously supported its role in avoiding DGF. Van Valenberg and colleagues described the intraoperative use of mannitol as “indispensable.”13 In their randomized controlled trial of kidney transplant recipients, patients were randomly assigned to receive 250 mL of 20% mannitol or 250 mL of 5% dextrose solution. Immunosuppressive therapy comprised either azathioprine or cyclosporine and prednisone with no antibody-based induction. The authors found that rates of acute renal failure after transplantation, defined as less than 400 mL of graft-derived urine output in 24 h, or the necessity of dialysis during the postoperative course, or both, were lower in the mannitol groups (18% v. 44% and 19% v. 53% for azathioprine and cyclosporine, respectively).13 With outcomes directly tied to urine output criteria, the administration of a diuretic unsurprisingly led to improved metrics of early renal function. Although this study protocol reflects outdated immunosuppressive therapy and an alternative cut-off for what may be termed DGF in modern contexts, the findings have historically lent support to the use of mannitol for the prevention of DGF.
Koning and colleagues reported a prospective multi-institutional study of kidney transplants from deceased donors.3 Recipient variables were analyzed to identify factors that predicted DGF. The authors concluded that intraoperative mannitol was associated with a lower rate of DGF (21% for mannitol v. 30% for none) on χ2 analysis but was not significantly protective against DGF on logistic regression. Mannitol or furosemide was recommended as part of the research protocol, yet 49% of recipients did not receive either agent, and 30% specifically did not receive mannitol.3 This deviation from study protocol suggests uncertainty around intraoperative diuretics even 20 years ago.
Furosemide, a loop diuretic that has been used as an alternative intraoperative diuretic, inhibits the Na-K-2Cl channels of the thick ascending limb of the loop of Henle, inducing a natriuresis and an increase in urine flow.3 Purported benefits of furosemide relate to improving fluid balance and reducing the energy consumption of tubule cells by inhibition of ion channels.14 There is basic science evidence for using furosemide. Heyman and colleagues interrogated the impact of loop diuretics on proximal tubule damage during hypoxia in a rat model.7 In their study, rats with isolated renal perfusion were exposed to an acellular perfusate over 90 min with or without loop diuretic. Urine output was higher with furosemide than in the control group, as was fractional excretion of potassium and sodium.7 Loop diuretics attenuated medullary thick ascending limb and proximal tubular damage at all levels of the tubules, with fragmentation rates of 9.8% in the control group versus 1.4% in the furosemide group. Glucose reabsorption, a marker of active transport in the tubules, was maintained at higher levels in kidneys exposed to loop diuretics, suggesting greater oxygen availability to tubule cells.
In a retrospective review of a single institution’s outcomes, Bhandari and colleagues compared the outcomes of NDD renal transplants in patients given furosemide versus no diuretic.18 The rate of DGF was 17/57 (30%) in the furosemide group and 13/42 (31%) in the control group.18 No antibody-based induction was described, and immunosuppressive therapy consisted of prednisone; cyclosporine; and 1 of azathioprine, mycophenolate, or rapamycin. These results suggest that furosemide does not reduce rates of DGF in deceased donor transplants. The lack of DCD grafts, the use of historic immunosuppressive protocols, and the retrospective nature of the report limit the generalizability of these data, but these results question the utility of loop diuretics.
Limitations
This study has several substantial limitations to consider when interpreting the results. The assignment of patients to diuretic groups was based on the surgeon performing the transplant, rather than being true random assignment. To account for the possible effect the surgeon may have had on outcomes, this study included a crossover period in which each surgeon utilized the other diuretic or no diuretics. The decision to accept a given organ offer was based on consensus between the on-call nephrologist, surgeon, and tissue typing laboratory representative. Thus, although a given surgeon may influence the rate of acceptance of certain donor subtypes, this risk is considered minimal given the multisource input for organ acceptance. Furthermore, no changes were made to any of the standard operating practices regarding perioperative and postoperative recipient management during the study period. Another limitation relates to the lack of data on urine output as well as intraoperative hemodynamics that prevent evaluation of transient hypotension in the postreperfusion time period.
Conclusion
This study demonstrated a lower rate of DGF in patients receiving an intraoperative diuretic (mannitol or furosemide) than in those who did not. There was no difference between the individual diuretic groups and controls, however. These data suggest that diuretics may have a beneficial effect on DGF in patients undergoing kidney transplantation, but larger sample sizes and higher quality data are required to definitively answer this question. A large, multicentre randomized controlled trial is warranted.
Footnotes
Competing interests: None declared.
Contributors: A. Sener conceived the study. D. Lee and C. Rim acquired the data, which M. Levine, A. Rasmussen, K. Farokhi, and P. Luke analyzed. M. Levine, A. Rasmussen, and K. Farokhi wrote the article, which D. Lee, C. Rim, P. Luke, and A. Sener critically revised. All authors agreed to be accountable for all aspects of the work.
- Accepted November 9, 2023.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/