Abstract
Background: Delivering trauma and surgical care to Northern Quebec presents unique challenges owing to the region’s remoteness, extreme weather and limited transport; the expansion of telehealth could help address these difficulties. We aimed to evaluate current surgical, trauma and telemedicine capacity in Nunavik, Quebec.
Methods: We used validated assessment tools, including the Personnel, Infrastructure, Procedures, Equipment and Supplies survey, the International Assessment of Capacity for Trauma index and the Maryland Health Care Commission Telemedicine Readiness tool to evaluate surgical, trauma and telemedicine capacity, respectively. We adapted these tools to the Northern Quebec context through discussions with local leadership. Data were collected in 2 regional hospitals — the Ungava Tulattavik Health Centre (UTHC) and the Inuulitsivik Health Centre (IHC) — and 12 Centres locaux de services communautaires (CLSCs; local community services centres) in 6 villages along the Hudson Bay coast and 6 villages along the Ungava Bay coast through iterative discussions with 4 chief nurses from each regional hospital and set of CLSCs; resources were confirmed through on-site evaluation by the respondents. We performed a descriptive analysis of the data.
Results: Surgical capacity was highest in the IHC (6.76) and lowest in the Ungava Bay CLSCs (5.52). Personnel (0%–0%) and procedures (13%–33%) were the least available resources. Trauma capacity was highest in the IHC (7.25) and lowest in the Hudson Bay CLSCs (5.58). Although equipment (90%–100%) and supplies (100%–100%) were readily available, personnel (0%–0%) and procedures (25%–56%) were lacking. The UTHC was most prepared for telehealth (67.80%), and the Ungava Bay CLSCs achieved a lower score (51.13%). Underdeveloped telehealth criteria included funding, administrative support, quality improvement and physical spaces (all 33%–67%).
Conclusion: Acute care capacity in Nunavik appears heterogeneous, with readily available equipment and supplies, but a lack of personnel capable of performing lifesaving procedures. To address the need for telemedicine, future initiatives should focus on improving funding, administrative support, physical spaces and quality-improvement initiatives.
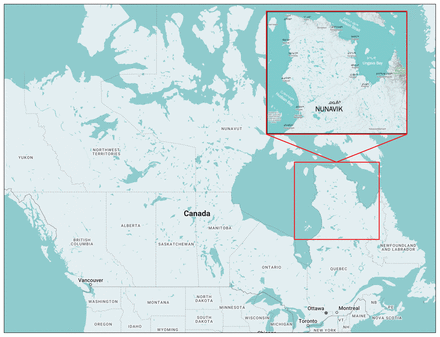
Quebec is the largest province in Canada, with a land area of 1.35 million square kilometres inhabited by the country’s second-largest population, 8.5 million residents.1,2 The Nunavik region is in Northern Quebec and occupies one-third of the province’s surface area.1 Although it represents a substantial land area, just 13 000 residents (0.15% of Quebec’s total population) inhabit the region, 90% of whom identify as Inuit and live in 14 villages located along the coasts of Ungava Bay, Hudson Bay and Hudson Strait (Figure 1 and Figure 2).1 The remoteness, lack of developed road systems, limited modes of transport, extreme weather conditions and low population density of the Nunavik region make surgical and trauma care delivery to the region very challenging.3 Furthermore, compared to the rest of Canada, Indigenous populations experience lower life expectancy owing to higher rates of trauma-related death from motor vehicle accidents, suicide and other traumatic injuries, and have poorer outcomes after operative interventions.4–6 Ongoing disparities in Indigenous health are multifactorial and stem from a colonial context of historical and intergenerational trauma, social determinants of health, and cultural, economic and political factors.
Map of Nunavik, Quebec, Canada. Source: Snazzy Maps (https://snazzymaps.com).
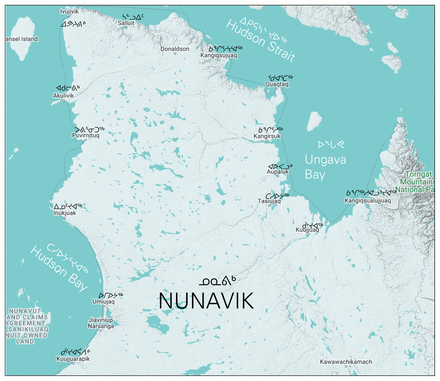
Larger-scale map of Nunavik. Source: Snazzy Maps (https://snazzymaps.com).
Improving trauma and surgical outcomes in Nunavik inevitably relies on augmenting access to care, which, in turn, relies on the availability of resources required to provide optimal care. However, to our knowledge, a systematic evaluation of the trauma and surgical resources available in the Nunavik region has not been performed. We hypothesized that an in-depth assessment would provide a detailed portrait of available resources in order to identify clear areas of deficiency to focus future capacity-building initiatives.
In addition, the use and implementation of telemedicine have significantly expanded during the COVID-19 era.7 Its use has numerous advantages in well-resourced settings, including limiting cross-infection of high-risk and chronic disease patients, increasing flexibility of staff and patients in time and space, as well as decreasing wait times; however, telemedicine is particularly advantageous in providing care and support to remote regions.7 We hypothesized that there would be deficiencies in personnel and therefore sought to assess the region’s readiness for telemedicine as a future mitigating strategy.
Thus, the main objectives of this study were to evaluate the availability of surgical and trauma resources in the Ungava Tulattavik Health Centre (UTHC), the Inuulitsivik Health Centre (IHC) and 12 Centres locaux de services communautaires (CLSCs; local community services centres) in villages along the Hudson Bay and Ungava Bay coasts; and assess the region’s readiness for the potential implementation of a telemedicine program.
Methods
Design and setting
We conducted a cross-sectional survey in 14 health care centres in Nunavik to assess the region’s surgical, trauma and telehealth capacity. There are 2 regional hospitals that provide secondary and limited tertiary care to surrounding villages: the UTHC and the IHC. The UTHC has 22 hospital beds and serves as a hub to Kuujjuaq (the largest village in the region, as well as the administrative capital) and 6 smaller villages along Ungava Bay: Kangiqsualujjuaq, Kangirsuk, Kangiqsujuaq, Quaqtaq, Aupaluk and Tasiujaq. The IHC has 26 hospital beds and provides care to Puvirnituq and 6 other villages along Hudson Bay: Salluit, Inukjuak, Kuujjuarapik, Akulivik, Ivujivik and Umiujaq. Of note, family physicians currently working in Nunavik do not have an Enhanced Surgical Skills background. The CLSCs serve as a point of service to each community, providing front-line health care and social services, physical rehabilitation and social reintegration. Villages such as Inukjuak, Salluit and Kuujjuarapik have family physicians available full-time, and other villages receive monthly visits by family physicians. Patients requiring further care are transported by prop plane to the closest regional hospital to be assessed and, if deemed necessary by the evaluating physician, are sent by fixed-wing aircraft to the Montreal General Hospital, the nearest level 1 trauma centre and the nearest hospital capable of providing emergency surgical care.
Data collection
We adapted 3 validated assessment tools — the Personnel, Infrastructure, Procedures, Equipment and Supplies (PIPES) survey,8 the International Assessment for Capacity for Trauma (INTACT) index9 and the Maryland Health Care Commission Telemedicine Readiness tool10 — to the Northern Quebec context through a literature review and discussions with local health care leadership, including the director of professional services and members of the Department of Quality, Evaluation, Organizational Performance and Ethics of the Nunavik Regional Board of Health and Social Services. Data were collected by A.K. through iterative discussions with 4 chief nurses from each regional hospital and set of CLSCs. Resources were confirmed through on-site evaluation by the respondents to ensure the validity of the results.
The PIPES survey was specifically designed to assess surgical capacity in low-resource settings and has been validated in various low- and middle-income countries including Sierra Leone and Bolivia.8,11 Higher scores have been shown to correlate with trackable and known improvements.8 The survey comprises 105 elements divided into 5 categories: personnel, infrastructure, procedures, equipment and supplies. One point is allocated for the full-time availability of each element. The personnel score is calculated by allocating 1 point for the full-time availability of general surgeons, anesthesiologists, physicians qualified to perform surgical procedures and nurse anesthetists. A final score is calculated by adding all individual scores, dividing the total score by the total number of elements (105) and multiplying the result by 10. There is no maximum score.
The INTACT index contains 40 key elements of the PIPES survey, including resuscitation, laparotomy, chest tube insertion, fracture repair and burn management capabilities, that have been validated to be more specific for trauma in 10 government hospitals in Sierra Leone.9 The applicability of this tool in resource-limited settings was further shown in India and Mongolia.12,13 The personnel score is calculated by allocating 1 point for the full-time availability of a qualified and trained surgical specialist, and 1 point for the full-time availability of an anesthesiologist, for a maximum score of 2. Scores for the remaining elements are calculated by means of the same method as for the PIPES tool. A final score is calculated on a scale of 0 to 10.
For both the PIPES survey and the INTACT index, there is no absolute scale of reference. Rather, relative scores are used for comparison between lower- and higher-resourced centres and to document improvements over time within the same centre.
To assess the region’s preparedness for a telemedicine program, we used the Maryland Health Care Commission Telemedicine Readiness tool, as it explores categories such as core readiness, operations, staff engagement and patient awareness.10 It was developed in collaboration with RTI International (Research Triangle Institute), an independent, nonprofit research institute that tackles global health challenges using scientific methods and multidisciplinary approaches in collaboration with governments, foundations, businesses and academic establishments (https://www.rti.org). The tool was created through an exhaustive literature review of more than 150 references, then field-tested with the Maryland Telehealth Alliance and Maryland Medicaid, as well as 20 small physician practices in the region. It includes a questionnaire, a scoring sheet and supporting documents that may be used as a guide to help improve individual categories that have lower scores. There are 5 key domains in the tool: core readiness, financial considerations, operations, staff engagement and patient readiness. Items are rated as not applicable/unsure (1 point), somewhat applicable (2 points) or fully applicable (3 points). The overall readiness score is a weighted average of the concept scores included within the 5 domains. The score is interpreted as follows:
≤ 50%: low level of readiness; has not considered many aspects of the questionnaire and/or is in the beginning stages of implementing a telemedicine program
> 50% to ≤ 75%: moderate level of readiness; has considered some aspects of the questionnaire, whereas others need improvement
> 75%: high level of readiness; has considered many elements of the questionnaire.
In response to iterative discussions with local health care leadership in Nunavik, we excluded questionnaire items that were deemed less pertinent or overly specific to target facilities from the original questionnaire, which made the questionnaire easier for respondents to complete.
Because this was a quality-improvement initiative, formal exemption from research ethics board approval was obtained.
Statistical analysis
We performed a descriptive analysis. We reported scores as absolute values, with means and ranges for specific categories of the assessment tools. We averaged the final PIPES survey and INTACT index scores for the 2 sets of CLSCs to enable comparisons, although we calculated individual data points to ensure a more detailed assessment of available resources.
Results
Surgical capacity as measured with the PIPES survey was highest in the IHC (6.76) and lowest in the Ungava Bay CLSCs (5.52) (Table 1). The mean score was 5.98. The available resources in the Ungava Bay CLSCs and the Hudson Bay CLSCs were identical with the exception of those in Inukjuak and Salluit, which have access to a radiography machine and therefore had higher scores than the other villages (5.62 v. 5.52). Supplies (96%–100%), equipment (86%–100%) and infrastructure (72%–85%) were the most available resources, and personnel (0%–0%) and procedures (13%–33%) were the least available.
PIPES survey scores for the 2 regional hospitals and 2 sets of CLSCs
Trauma capacity, as measured with the INTACT index, was highest in the IHC (7.25) and lowest in the Hudson Bay CLSCs (5.58) (Table 2). The mean score was 6.21. The CLSCs in Inukjuak and Salluit had a score of 5.75, and those in the other villages had a score of 5.50. Supplies (100%–100%) and equipment (90%–100%) were readily available, but personnel (0%–0%) and procedures (25%–56%) were lacking. The presence of the INTACT index elements is presented in Table 3.
INTACT index scores for the 2 regional hospitals and 2 sets of CLSCs
Scores for the INTACT index elements for the 2 regional hospitals and 2 sets of CLSCs
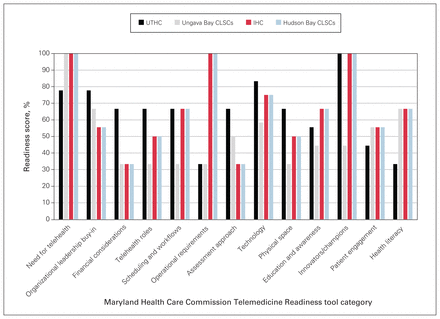
The UTHC was deemed most prepared for telehealth, with an overall weighted score of 67.80%. The Ungava Bay CLSCs achieved a lower overall weighted score, 51.13%. However, all scores fell within the moderate range of preparedness, with a mean of 62.2%. Figure 3 shows the overall scores for each category. Although the need for telehealth was deemed high (78%–100%) at all facilities, areas for improvement identified included funding (33%–67%), administrative support (33%–67%), quality improvement (33%–67%) and availability of physical spaces (33%–67%).
Telemedicine readiness scores for the 2 regional hospitals and 2 sets of CLSCs by category of the Maryland Health Care Commission Telemedicine Readiness tool. CLSC = Centre local de services communautaires (local community services centre); IHC = Inuulitsivik Health Centre; UTHC = Ungava Tulattavik Health Centre.
Discussion
We found that, although supplies, equipment and infrastructure were readily available in Nunavik, access to personnel and the skill set required to perform specialized procedures were most lacking. The need for telemedicine was deemed high at all facilities; however, preparedness was deemed moderate at best, with substantial improvement required in funding, administrative support, quality improvement and physical spaces.
Limitations in access to personnel and specialized skill sets are not limited to Northern Quebec. Fleet and colleagues14 reported that only 12% of rural emergency departments in British Columbia had access to a general surgeon on call 24 hours a day, 7 days a week; this lack was shown to be a major cause of patient transfers. Furthermore, studies from Ontario and Quebec have shown the potential benefits of continuing education and the development of professional competencies as a way to meet the challenges of a larger scope of practice in rural medicine.15,16
Tailoring trauma and surgical programs to rural settings has been shown to improve skills in acute management such as risk assessment, teamwork, efficacy and confidence.17,18 Respondents in the study by Tarighi and colleagues19 indicated difficulty accessing training programs such as the Advanced Trauma Life Support, as well as lack of awareness about newer trauma educational opportunities such as the Rural Trauma Team Development Course. Access can be facilitated through virtual delivery or the use of portable simulator machines. Martin and colleagues18 explored the use of a mobile emergency simulator that provides training opportunities for the management of critical health conditions. Their respondents were satisfied with their experience overall, as it helped develop essential critical care skills in resource-limited settings.
To further address these shortcomings, we recommend the following initiatives based on the results of our study:
Expansion of telecommunication opportunities between health care providers in rural settings and specialists from urban centres
Development of tailored educational programs for surgical and trauma care in rural settings
Elaboration of incentive programs to promote the recruitment and retention of health care workers in rural settings
Early exposure of medical students to rural medicine through emphasis on Indigenous and rural health care in medical curricula, as well as mandatory rotations in these settings; such factors have been shown to increase interest among trainees and licensed professionals to practise in these settings.19–21
The use of telemedicine may help tackle challenges in delivering high-quality surgical and trauma care in rural regions and contribute toward improving patient outcomes and system efficiency. In a rapid review of the impact of telemedicine on the diagnosis, clinical management and trauma outcomes in rural patients, Lapointe and colleagues22 observed efficient patient evaluation and diagnosis with telemedicine use, leading to shorter transfer times and reduced lengths of stay. Duchesne and colleagues23 found similar outcomes in rural Mississippi: the use of telemedicine enabled quicker identification and stratification of more severely injured patients, as well as significantly shorter patient transfers (1.7 h v. 13.0 h) and significantly decreased lengths of stay (1.5 h v. 47.0 h). Furthermore, several studies support remote teleconsultation as a way to reduce the individual, societal and economic burdens of potentially avoidable patient transfers to tertiary care centres.24–26 It has also been suggested that telemedicine use improves initial screening and management in orthopedic and neurologic emergencies, and for patients with acute burn injuries.25–27
There is limited literature exploring the use of telemedicine in Northern Canada. Seto and colleagues28 showed that, in areas such as the Yukon Territory, available programs are not used to their maximum potential. Jong and colleagues29 explained that telemedicine use can improve health care delivery in Northern Canada by providing timely and accessible care within communities, and decreasing the need for travel. Park and colleagues30 indicated 2 important benefits: improvement in clinical diagnosis of surgical emergencies and the ability of surgeons in urban centres to guide remote physicians in performing certain lifesaving procedures.
Our results indicate a marked need for but only moderate levels of preparedness for telemedicine in the facilities studied. To address this situation, we recommend the implementation of funding and quality-improvement initiatives that focus on assessing the capital costs needed to establish a telemedicine program and conducting a cost, benefit and risk analysis; establishing telehealth roles to manage administrative aspects; incorporating a longitudinal iterative assessment approach, including factors influencing success and feedback systems to promote quality of care; and establishing designated physical spaces for telemedicine consultations.
This study provides a comprehensive assessment of surgical, trauma and telemedicine capacity in Northern Quebec. It provides specific recommendations for quality-improvement and capacity-building initiatives, and should serve as a baseline for future evaluation of surgical, trauma and telemedicine capacity. We hope our findings will influence future governmental funding priorities and serve as an impetus to allocate further resources to trauma and surgical care in Nunavik, specifically in the recruitment and retention of personnel, and in the development of telemedicine capacity.
Limitations
Data points were obtained from a single respondent from each regional hospital and group of CLSCs. Every effort was made to confirm the responses through on-site evaluations to ensure the validity of results; however, it is possible that certain data points were incomplete.
Telemedicine readiness criteria included in the questionnaire may require further discussions among health care providers, administrators and quality-improvement agents to maximize the utility of this tool. However, the data collected were sufficient for a preliminary evaluation of the current need for a telemedicine program and identification of areas for improvement.
Responses to the questionnaires were often binary, taking into account only the full-time availability of resources. Access to optimal trauma and surgical care is evidently more nuanced, and future studies should examine the availability of resources in a more detailed fashion.
Finally, access to resources for trauma and surgical care is complex, and many factors may not have been captured in the questionnaires used in this study. However, these validated tools provide a framework to assess the essential resources required for basic care.
Conclusion
Our cross-sectional survey showed adequate accessibility of equipment and supplies but a lack of trained personnel capable of performing life-saving trauma and surgical procedures in Northern Quebec. We also found a major need for a telemedicine program; however, its implementation will require further improvements in funding, administrative support, quality improvement and physical spaces. These findings should guide future funding priorities and capacity-building initiatives.
Acknowledgements
The authors thank Audrey Le Gall Payne, Catherine Bédard, Sharon Collins and Marie-Claude Savard for their contributions in data collection.
Footnotes
Presented at the Trauma Association of Canada 2022 Annual Scientific Meeting & Conference, Apr. 7–8, 2022, Montréal, Que.
Competing interests: D. Deckelbaum is chair of the board of directors of DeckTherapeutics. K. Khwaja is chief medical officer of AIRMEDIC. No other competing interests were declared.
Contributors: A. Kis, T. Razek, J. Grushka, N. Boulanger, L. Watt and E. Wong designed the study. A. Kis and E. Wong acquired the data, which all authors analyzed. A. Kis and E. Wong wrote the article, which all authors reviewed. All authors approved the final version to be published.
Funding: This study was funded by a Canadian Association of General Surgeons’ Operating Grant, a Tomlinson Award from the Department of Surgery, McGill University, a McGill Global Health Scholars award to A. Kis and a McGill Global Health MDCM Student Research award to A. Kis.
- Accepted September 7, 2023.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/