Abstract
Background: High-level payment data provided by Doctors of BC showed a 19.7% pay disparity in annual payments between female and male general surgeons in fiscal year 2019/20, and this was previously as high as 30% in 2012/13. This study aimed to examine the impact of targeted fee increases on pay disparity by sex over time.
Methods: The top 35 fees billed by female general surgeons, representing 76.3% of total payments, were retrospectively analyzed. The pay disparity by sex was calculated for each individual fee from 2000/01 to 2019/20.
Results: There were notable billing differences between female and male general surgeons. Female surgeons billed breast oncology procedures, malignancy consultations and visits, and peritoneal malignancy surgical procedures in greater proportions than did their male counterparts. Male surgeons billed hemorrhoid banding and rigid proctosigmoidoscopy in greater proportions than their female counterparts. With targeted fee increases, pay disparity by sex worsened for 17 of the top 35 fees but improved for the other 18 from 2010/11 to 2019/20, to varying degrees, resulting in an overall reduction in pay disparity by sex from 23% to 15%. If across-the-board fee increases had been implemented instead of targeted fee increases, the disparity in 2019/20 would have been 19% instead of 15%.
Conclusion: Targeted fee increases reduced pay disparity between male and female general surgeons compared with theoretical across-the-board fee increases in British Columbia from 2010/11 to 2019/20, but not uniformly; some fee increases resulted in increased disparity. Other physician groups should conduct a similar analysis and allocate future fee changes with the aim of improving rather than worsening disparity.
In 2021, Doctors of BC (DoBC), the medical association for all physicians in British Columbia, provided the economics committee of each specialty section with Medical Services Plan payment data from fiscal year 2019/20 by physician sex. This revealed a 19.7% disparity between female and male general surgeons billing more than $150 000 per year, excluding those above the 90th percentile. Historical data showed a disparity as high as 30% in 2012/13. This is in keeping with other studies that show female surgeons earn 24% less per hour than male surgeons.1 This prompted us to conduct a deeper analysis of current billing patterns, historical trends over 20 years and the effect of target fee increases over the past 10 years.
Pay disparity between female and male surgeons is a complex issue with many contributing factors.1–5 We were not able to find any other studies looking at individual fee codes and the impact of fee allocations on disparity by sex with respect to payment.
We hypothesized that fee allocation decisions made in the past 10 years have unintentionally helped to mitigate the pay disparity by sex; several new fees had been introduced, such as a higher consultation fee for malignancy that may have disproportionately benefited female surgeons, but to our knowledge the impact has not yet been analyzed or quantified. In this study, we sought to examine the impact of fee increases such as this using data with more granular detail than the data provided by DoBC, which were based on gross payments and not individual fees.
Methods
We obtained aggregate, anonymized raw data from DoBC, including payments by individual fee codes to members of General Surgeons of BC for fiscal years 2000/01, 2005/06, 2010/11, 2015/16 and 2019/20 to conduct our own analysis. Data were available only by surgeon sex, not self-identified gender.
We selected the top 35 fees (out of more than 600) billed by female general surgeons by payment in 2019/20 for analysis, representing 76.3% of total payments to female general surgeons. The same 35 fees represented 72.0% of total payments to male general surgeons. Initially, we intended to analyze the top 20 fees, but this comprised only 60% of total payments; therefore, more fees were added to increase this percentage. We did not have the resources to analyze all of the more than 600 fees billed by general surgeons in BC.
We calculated the annual payment to the average female or male general surgeon for each individual fee. First, we calculated the proportion of total payments to all female and male general surgeons for each fee in a given fiscal year. Then we multiplied this percentage by the average annual payments to female and male general surgeons as reported by DoBC for the same year (billing more than $150 000 and excluding those above the 90th percentile). We could calculate the pay disparity by sex for each fee code by subtracting the payments to male general surgeons from the payments to female general surgeons. We chose this methodology as we had aggregate data only, not individual billing data per surgeon.
We chose to use the average annual payment data supplied by DoBC that excluded those who billed less than $150 000 per year and those above the 90th percentile to better reflect the typical practice of a general surgeon in BC. These are standard cut-offs that are reported annually by the Medical Services Plan in BC and thus readily available, reflecting a short tail on the low end with semi-retired and part-time surgeons earning less than $150 000 and a long tail with a small number of outliers on the high end of the payment curve.
We performed the same calculation by fee code on historical data from 2010/11 to 2019/20 to analyze for trends. We also analyzed fee values over time.
Finally, we performed a simulation to calculate what the current payments for the top 35 fees would have been if across-the-board fee increases had been implemented rather than targeted fee increases from 2010/11 to 2019/20.
Results
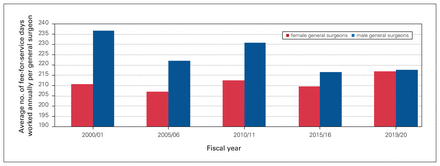
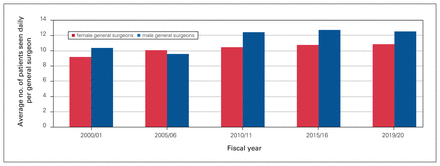
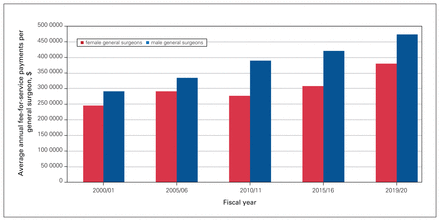
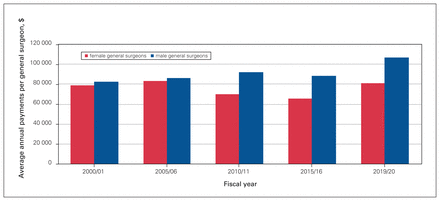
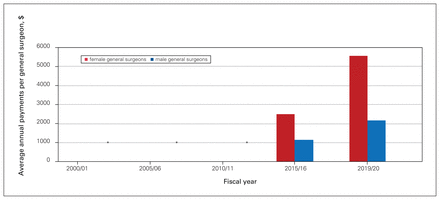
Figure 1, Figure 2, Figure 3 and Figure 4 present aggregate data provided by DoBC. These are data for the province of BC as a whole and do not provide detail in terms of academic versus rural practice or geographic location. Figure 1 shows that the number of female general surgeons in BC billing more than $150 000 annually increased more than 7-fold, whereas the number of male surgeons stabilized and then remained unchanged over the study period. Figure 2 shows that the number of days worked per year equalized over the study period between male and female general surgeons. Figure 3 shows that there was a persistent difference in the number of patients seen per day by male and female general surgeons. Figure 4 shows that the average fee-for-service payments increased 55% for female general surgeons and 62% for male general surgeons from 2000 to 2019.
Number of general surgeons in British Columbia billing more than $150 000 annually (excluding those above the 90th percentile).
Average number of fee-for-service days worked per year by general surgeons in British Columbia billing more than $150 000 per year (excluding those above the 90th percentile).
Average number of patients seen per day by general surgeons in British Columbia billing more than $150 000 per year (excluding those above the 90th percentile).
Average annual fee-for-service payments to general surgeons in British Columbia billing more than $150 000 per year (excluding those above the 90th percentile).
Table 1 shows the top 35 fees billed by female general surgeons in 2019/20, $19 639 154 out of a total of $25 752 808 that year (76.3%). Table 2 shows the top 35 fees billed by male general surgeons in the same year. Total payments to male general surgeons were $85 020 363.
Top 35 fees billed in 2019/20 by total payments to female surgeons
Top 35 fees billed in 2019/20 by total payments to male surgeons
Overall, there is good correlation between the 2 lists with a few notable exceptions. The breast oncology fees (sentinel node biopsy, partial mastectomy, skin-sparing mastectomy, total mastectomy, fine-wire breast biopsy and axillary dissection) occupy the fifth, 10th, 13th, 20th, 28th and 29th positions, respectively, for female general surgeons. Among male general surgeons, only sentinel node biopsy makes the top 35; it is in the 24th position, 19 positions lower than among female general surgeons. The other breast fees appear much further down for male general surgeons, with skin-sparing mastectomy in the 121st position.
The consultation and office visit fees for malignancy appear in the 8th and 12th positions, respectively, for female general surgeons and in the 13th and 30th, respectively, for male general surgeons. Peritonectomy is 34th for female general surgeons but in the 189th position for male general surgeons.
The reverse situation is seen for hemorrhoid banding, located in the ninth position for male general surgeons and the 27th position for female general surgeons. Rigid proctosigmoidoscopy is 23rd for male general surgeons, along with the associated major tray fee in 20th position. These are in 90th and 70th positions, respectively, for female general surgeons.
Table 3 summarizes the calculated disparity in payments per surgeon for the top 35 fees billed by female general surgeons, comparing 2010/11 to 2019/20. In 2010, female general surgeons received $63 849 less in payments for these fees than male general surgeons, a 23% difference. In 2019/20, this amount decreased to $50 972, a 15% difference. The disparity worsened for 17 fees but improved for the other 18 fees to varying degrees. Colonoscopy and polypectomy had the largest increase in disparity by $10 093, but this was offset by lessening disparities in the other 2 colonoscopy fees. The consultation fee also showed an increase in disparity by $3064. The fees with the greatest improvement or reversal of gender pay disparity were the malignancy consult and visit fees, laparoscopic cholecystectomy, skin-sparing mastectomy and inguinal hernia repair.
Disparity in payments for the top 35 fees to the average female general surgeon relative to the average male general surgeon in 2010/11 and 2019/20, and the disparity if across-the-board fee increases for the top 35 fees had been implemented in 2019/20
The fourth column in Table 3 shows the disparity that would have resulted if fees had been increased by 2% across the board rather than in a targeted fashion, as shown in Table 4. Instead of a difference of $50 972, the pay disparity between male and female general surgeons would have been $59 166 or 19%. For a handful of fees, the disparity would have been lessened with across-the-board increases, most notably the consultation fee and the fee for hemorrhoid banding. However, for most fees, the disparity would have been worse with across-the-board increases. The data show that fee increases predominantly in the malignancy consultation and visit fees, the breast oncology fees and the peritonectomy fee contributed to reducing payment disparity between female and male general surgeons. Increases for fees for other office visits, certified assistant fees, fees for laparoscopic appendectomy and some other fees also made modest contributions to reducing disparity.
Changes in the payments for the top 35 fees billed by female general surgeons over the study period
In 2018, the decision was made to reduce the colonoscopy with polypectomy fee by 17.8% and the funds were used to increase the consultation fee. In BC, there are separate fees for colonoscopy with and without polypectomy. This reduction in the colonoscopy with polypectomy fee had an interesting effect on pay disparity between male and female general surgeons, decreasing it by almost $6000 per surgeon compared with the amount if this had not been done. This is illustrated in Figure 5.
Average annual payments per surgeon for colonoscopy with polypectomy (calculated from raw data). All general surgeons were included in the analysis in this figure.
Increases to the consultation fee, however, increased disparity by about $3500 per surgeon, as illustrated in Figure 6. This could be explained by the difference in the number of patients seen per day (Figure 3), resulting in a disparity in payment because of the compounding of this difference over a whole year. In BC, the consultation fee is the same whether it is billed during business hours or after hours. Consults seen after hours are supplemented by a call-back or continuing care surcharge and after-hours surgeries are supplemented by an after-hours surgical surcharge. A special consultation fee for malignancy was created in 2012. Figure 7 shows that this was billed disproportionately by female general surgeons and its creation was a key factor in reducing pay disparity between male and female general surgeons. Figure 8 shows that the office visit for malignancy fee had an even greater impact.
Average annual payments per surgeon for consultation (calculated from raw data). All general surgeons were included in the analysis in this figure.
Average annual payments per surgeon for consultation for malignancy (calculated from raw data). All general surgeons were included in the analysis in this figure. *There are no data for these years because this fee was created in 2012.
Average annual payments per surgeon for office visit for malignancy (calculated from raw data). All general surgeons were included in the analysis in this figure. *There are no data for these years because this fee was created in 2012.
Discussion
The top 35 fees, representing more than three-quarters of total payments, showed improvements in the pay disparity between female and male general surgeons from 2010 to 2019, from 23% to 15%. Although this is better than the 24% disparity previously described in Ontario2 and the 39% disparity among some surgeons in the United States,3 we still have work to do to address and eliminate disparity. The 19.7% disparity reported by the DoBC in 2019/20 is more than the 15% that we have calculated, probably because of methodologic differences. The reason for the discrepancy is not clear; it may be because we analyzed only the top 35 fees and not all of the more than 600 fees in the general surgery fee schedule. We acknowledge this limitation; however, our findings do agree with those of DoBC in that the disparity has been decreasing rather than increasing since 2010. We have shown that this was a serendipitous result of targeted fee increases.
In 2011, General Surgeons of BC approved a motion at their annual general meeting to allocate new funds to fees that had the greatest difference in value compared with the neighbouring province of Alberta, which was accepted as a gold standard because Alberta’s fees were the highest in the country at the time. Fees at parity with or higher than the corresponding fees in Alberta were not allocated new money. Before this motion, fee increases were largely allocated by across-the-board percentage increases to all fees. This new approach largely explains the differences in fee increases from 2010/11 to 2019/20 seen in Table 4, ranging from 0% to 173% increases. Several new fees were also created during this time period, including fees for consultations for malignancy, office visits for malignancy, surcharges for patients with body mass index greater than 35, preoperative assessments and peritonectomy. Fee increases could not be calculated when there was no preexisting comparator.
Why there was a disparity in colonoscopy and other endoscopy fees is unclear. Other studies have reported that male surgeons are preferentially referred patients who require more remunerative procedures.1 It is also possible that female surgeons are not allocated a proportional amount of resources for endoscopy, but investigating this possibility was beyond the scope of this study.
Pay disparity by sex is multifactorial. First, as we have demonstrated, there are substantial practice differences between female and male general surgeons, illustrated by fees for breast oncology and hemorrhoid banding. The reasons for these differences are complex, involving training motivations and influences from medical school through residency and fellowship and biases in recruitment and hiring.4 Practice and lifestyle decisions are also a factor, but we did not address this in our study. Second, there are changes in practice over time. For example, the volume of breast biopsies and total mastectomies has decreased over time, the volume of partial mastectomies has increased, the volume of open appendectomies and colon resections has decreased and the volume of laparoscopic procedures has increased. Third, there are structural or systemic factors; these include equitable allocation of resources such as operating room or endoscopy time as well as referral bias.
Referral bias has been reported to be a cause of pay disparity by sex because of more nonoperative referrals being sent to female surgeons.2 Previous studies have shown that female physicians spend 10% more time than male physicians in medical visits.5 Moreover, oncology consultations, predominantly for breast cancer, take longer than consultations for other conditions. This contributes to female surgeons seeing fewer patients per day, even though they work the same number of days per year as their male colleagues. This structural or systemic bias is more difficult to correct with fee increases alone and requires other interventions such as proportional resource allocation,6 centralized referral models,7 shared care protocols and education of referring physicians.
Residency education may also help reduce pay disparity by sex. For example, opportunities could be offered to enable male residents to develop skills and interest in breast surgery and female residents to develop skills and interest in endoscopy and hemorrhoid banding. This requires further study.
Limitations
We acknowledge that this study is limited in that we had access only to aggregate and raw billing data and were not able to identify or analyze subgroups, including subspecialties. Practices may also differ by geographic location and practice type. For example, an academic breast oncology practice in Vancouver that does not offer endoscopy would be very different from a community general surgery practice in Powell River, BC. We did not have access to a breakdown of the reasons for consultations, which would have helped to illuminate operative versus nonoperative referrals. In addition, it is unlikely that 60 female surgeons are each performing 2 peritonectomies a year; it is more likely that 3 female surgeons are performing 40 a year (and the rest are not performing any). As a result, our conclusions are limited to the “average” female or male surgeon.
Conclusion
We have shown in this study that choices in fee allocation have a significant impact on pay disparity between female and male general surgeons. Moreover, across-the-board increases across a set of fees exacerbate existing disparities. As a result of this study, General Surgeons of BC allocated retroactive fee increases from April 2021 after first calculating their impact on pay disparity by sex and made adjustments that, overall, reduced disparity. A specific example is an increase to several breast surgery fees. We plan to perform similar analyses for all future fee increases. We have also endeavoured to achieve sex balance on the economics committee of General Surgeons of BC that oversees these decisions. We encourage other physician groups in BC and across Canada to undertake a similar analysis of their fee schedules and make fee allocation decisions that do not worsen pay disparity by sex.
Footnotes
Competing interests: None declared.
Contributors: H. Hwang, A. Barton, D. Jenkin designed the study. T. Scott analyzed the data. H. Hwang and D. Jenkin wrote the article, which H. Hwang, A. Barton and T. Scott critically revised. All authors gave final approval of the version to be published.
- Accepted July 11, 2023.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/