Abstract
Background: Current national guidelines on caring for hip fractures recommend early mobilization. However, this recommendation does not account for time spent immobilized waiting for surgery. We sought to determine timing of mobilization following hip fracture, beginning at hospital admission, and evaluate its association with medical complications and length of hospital stay (LOS).
Methods: We performed a retrospective review of prospectively collected data for 470 consecutive patients who underwent surgery for a hip fracture between September 2019 and August 2020 at an academic, tertiary-referral hospital. Outcomes of interest included time from hospital admission to mobilization, complication rate and LOS. We used a binary regression analysis to determine the effect of different surgical and patient factors on the risk of a postoperative medical complication.
Results: The mean time from admission to mobilization was 2.8 ± 2.3 days (range 3 h–14 d). There were 125 (26.6%) patients who experienced at least 1 complication. The odds of developing a complication began to increase steadily once a patient waited more than 3 days from admission to mobilization (odds ratio 2.15, 95% confidence interval 1.42–3.25). Multivariate regression analysis showed that prefracture frailty (β = 0.276, p = 0.05), and timing from hospital admission to mobilization (β = 0.156, p < 0.001) and from surgery to mobilization (β = 1.195, p < 0.001) were associated with complications. The mean LOS was 12.2 ± 10.7 days (range 1–90 d). Prolonged wait to mobilization was associated with longer LOS (p = 0.01).
Conclusion: Comprehensive guidelines on timing of mobilization following hip fracture should account for cumulative time spent immobilized.
Hip fracture is a leading cause of disability and morbidity worldwide.1–4 It is estimated that the annual global number of hip fractures will increase from 1.26 million in 1990 to 4.5 million by 2050.5 Hip fractures represent a substantial public health issue owing to increasing individual, societal and health care costs.6 For these reasons, optimizing hip fracture care pathways has become a topic of great importance.
The timing of mobilization following a hip fracture is a key performance indicator for hip fracture care pathways as this affects postoperative recovery, facilitates rehabilitation and ultimately decreases complications and improves outcomes.7,8 The quality standards developed by the National Institute for Health and Care Excellence (NICE), whose guidelines are based on the most up-to-date available scientific evidence, recommend that patients be mobilized on “the day of or day after surgery at latest.”7
While several studies have reported on the association between the timing of mobilization and outcomes following a hip fracture, these studies have focused only on the timing of mobilization following surgery.7–12 However, for many of these patients who have reduced physiological reserve and are in a catabolic state following injury,13–15 the timing of mobilization should be interpreted taking into account the cumulative time spent immobilized.
We sought to determine the timing of mobilization of patients following a hip fracture (measured from the time of hospital admission), and to evaluate if the timing from admission to mobilization was associated with medical complications and length of hospital stay (LOS), thereby allowing us to define a relevant time frame for which patients with a hip fracture should be mobilized following injury.
Methods
Study design
The Ottawa Health Science Network Research Ethics Board reviewed and approved this study. We conducted a retrospective review of prospectively collected data on a consecutive cohort of patients who underwent surgery for a hip fracture at an academic, tertiary referral centre between September 2019 to August 2020. Patients were excluded if they sustained a periprosthetic or pathologic hip fracture. Patients were under the care of 26 surgeons. Surgeries were performed in accordance with each surgeon’s preferred surgical technique and approach. Similarly, the decision on type of anesthetic and use of peripheral blocks in our study reflects the judgment and practice of the anesthesiologists rather than predetermined guidelines.
All data were collected from the Operatively Repaired Fractures Database (ORFD). The ORFD is an institutional review board-approved institutional database that prospectively collects patient-level data extracted from electronic medical records, operating room information systems and discharge summaries. Data entry into the ORFD is controlled by the institutional research team. Data are reported in accordance with Strengthening the Reporting of Observational studies in Epidemiology (STROBE) guidelines.
We collected data on age, sex, prefracture frailty score (severely/terminally frail, vulnerable/mildly frail, managing well, very fit/well),16 prefracture morbidity, prefracture mobility (no functional mobility, some functional mobility, mobile with an aid, freely mobile, assessed using the Parker Mobility Scale and grouped into the above 4 categories as recommended per the National Hip Fracture Database mobility guidelines),7,18 fracture type (intertrochanteric, subtrochanteric, femoral neck fracture), type of surgery (fixation or arthroplasty procedure), perioperative complications and LOS. Prefracture morbidity status was assessed using the Charlson Comorbidity Index.17
Outcomes of interest
We reviewed patients’ electronic medical records (EMRs) to collect time of hospital admission, time of surgery and timing of mobilization. The time at which the patient was assessed in the emergency department of the presenting hospital, by the emergency department triage nurse, served as the time of admission (Tadmit). Thirteen (2.8%) patients suffered a hip fracture while as an inpatient, and therefore, documented time of the orthopedic consultation serves as time of admission for these patients. Time at which the patient arrived to the operating room served as time of surgery (Tsurg). Based on the recommended guidelines suggesting that patients be brought into surgery no later than 48 hours after admission and be mobilized “the day of or day after surgery at latest,”7 timing from admission to surgery (Tadmit→surg) and timing from surgery to mobilization (Tsurg→mob) were grouped into 24-hour periods for analysis. Combining Tadmit→surg and Tsurg→mob for each patient allowed us to determine the timing from admission to mobilization (Tadmit→mob). According to hip fracture care guidelines,7 mobilization may be defined as the capacity for a patient to sit or stand out of bed, with or without assistance.8 At our institution, information regarding mobilization is routinely charted in a patient’s EMR as per our hip fracture pathway protocol, and therefore, timing of mobilization was determined by the time stamp of the EMR entry documenting that the patient was mobilized (Tmob).
Postoperative complications and LOS were captured as part of the ORFD. Medical complications of interest included urinary tract infection (UTI), deep vein thrombosis (DVT), pulmonary embolism (PE), stroke, pneumonia and postoperative falls. We also sought to identify patient variables that may have influenced timing to mobilization.
Statistical analysis
Data were summarized using descriptive statistics, including numbers with percentages for categorical variables. Cross tabulation and analysis with χ2 and Fisher exact tests were used for categorical variables. Scale data were analyzed using 1-way analysis of variance. Any baseline patient demographics and surgery characteristics that showed significance or a trend toward significance (p < 0.2) from univariate analysis were inputted into a binary regression analysis to determine which factors were most associated with the development of postoperative complications. A p value of less than 0.05 was considered significant. All analyses were performed using IBM (IBM Corp.) SPSS software for Mac 9, version 27.
Results
Patient population
Of the 607 consecutive patients admitted for hip fracture during the study period, 128 were excluded from our analysis owing to missing information relevant to mobilization and 9 patients were excluded owing to withdrawn informed consent, leaving a final sample of 470 (77.5%) patients. The mean age of patients was 80.7 ± 13.1 years, and 64.9% were female. Seventy-six (12.5%) patients were transferred from outside institutions. With the exception of prefracture morbidity, there were no substantial differences between patient demographics or surgery characteristics in patients included and excluded from the study. Baseline patient demographics and surgery characteristics are presented in Table 1.
Baseline patient demographic and surgery characteristics
Timing of mobilization
The average Tadmit→mob was 2.8 ± 2.3 days (range 3 h–14 d). Fifty-three (11.3%) patients were mobilized within 24 hours of admission, 200 (42.5%) patients were mobilized 24–48 hours after admission and 217 (46.2%) patients were mobilized more than 48 hours after admission.
The average Tadmit→surg was 1.4 ± 1.1 days (range 1 h–5.8 d). Two hundred (42.5%) patients underwent surgery within 24 hours of admission, 179 (38.0%) patients 24–48 hours after admission and 91 (19.5%) patients more than 48 hours after admission.
The average Tsurg→mob was 1.9 days ± 2 hours (range 2 h–13 d). There were 120 (25.5%) patients mobilized within 24 hours postoperatively, 234 (49.8%) patients 24–48 postoperatively and 116 (24.7%) patients more than 48 hours postoperatively.
Complication rate and mean length of hospital stay
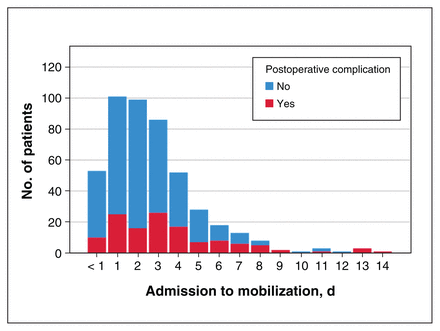
At least 1 postoperative complication occurred in 125 (26.6%) patients (146 total complications). The odds of developing a postoperative complication began to increase steadily once a patient waited more than 3 days from admission to mobilization (odds ratio [OR] 2.15, 95% confidence interval [CI] 1.42–3.25; Table 2), irrespective of when surgery took place. In addition, patients who waited more than 48 hours for surgery and more than 48 hours postoperatively to be mobilized had 6.3 (95% CI 1.4–3.6) times greater odds of developing a postoperative complication (Figure 1).
Risk of postoperative complications, by timing of admission to mobilization
Number of patients with hip fracture who experienced a postoperative complication, by timing from admission to mobilization.
Univariate analysis demonstrated a significant effect of prefracture frailty (p = 0.001), prefracture morbidity (p = 0.023), prefracture mobility (p = 0.011), Tadmit→surg (p = 0.128), Tsurg→mob (p = 0.016) and Tadmit→mob (p < 0.001). Multivariate analysis showed that prefracture frailty (β = 0.276, p = 0.050), Tadmit→mob (β = 0.156; p < 0.001) and Tsurg→mob (β = 1.195; p < 0.001) were associated with the development of a postoperative complication (Table 3).
Multivariate analysis of factors associated with the development of a postoperative complication
The mean LOS was 12.2 ± 10.7 days (range 1–90 d). Table 4 shows the association of Tsurg→mob and Tadmit→mob with LOS. Patients with the longest Tadmit→mob were those with the longest LOS (p = 0.013).
Association between the timing from surgery to mobilization and the timing from admission to mobilization and length of hospital stay
Patient factors influencing timing to mobilization
Prefracture frailty (p = 0.003), prefracture mobility (p = 0.007) and prefracture morbidity (p = 0.016) were significantly associated with the ability to mobilize patients. Patients with the poorest prefracture frailty scores experienced the greatest benefit from timely mobilization (p < 0.001). Among the 216 patients mobilized more than 72 hours after admission, the risk of developing a complication was much greater among the mildly to moderately or severely frail (69/168, 41.0%) than among those who were managing well or fit (7/48, 14.6%). The odds of delayed mobilization were significantly greater among the mildly to moderately or severely frail (168/302, 55.6%) than among those who were managing well or fit (48/168, 28.6%).
Discussion
Timely mobilization following surgery for hip fracture is standard of care as per national guidelines.7 However, current guidelines do not account for time spent immobilized from hospital admission to surgery, but rather recommend that patients be mobilized “on the day of or day after surgery.” Our findings show that the odds of developing a postoperative complication significantly increase if timing of mobilization is delayed more than 3 days from hospital admission. Patients with the longest time to mobilization (Tadmit→mob) were also those with the longest LOS.
Previous studies have shown that prolonged postoperative immobilization has been associated with worse postoperative outcomes.7–12 Goubar and colleagues8 analyzed hospital records for 126 897 patients who underwent surgery for hip fracture in England and Wales between 2014 and 2016 and found an association between early mobilization and survivorship and recovery. They concluded that early mobilization should be incorporated as a measured indicator of quality of care. In addition, previous studies have found that delayed timing from admission to surgery (beyond the recommended guidelines for surgery on the day of or day after admission) was associated with poorer patient outcomes18,19 and increased LOS.20 However, to our knowledge, no study to date has investigated the effect of timing from hospital admission to mobilization thus accounting for the total duration of time patients with a hip fracture spend immobilized following injury.
Our findings agree with current guidelines recommending early mobilization and early surgery for patients with a hip fracture. Current standard of care is to admit patients and schedule surgery on the day of or day after admission,7 and to then mobilize these patients as soon as they are medically stable, which is typically within the first 12–24 hours postoperatively. Owing to a lack of adherence to such guidelines at our centre, we found that the consequences of prolonged immobilization (Tadmit→mob) were associated with an increased risk of developing a medical complication: pneumonia, UTI, stroke, DVT, PE or having a postoperative fall. Delayed mobilization was also a determining factor in a patients’ hospital LOS. Our findings show that timing of mobilization has a significantly greater association with the likelihood of developing a complication, than does a patient’s prefracture health status.
These consequences have important ramifications on health care systems, carrying substantial financial costs and added workload for health care workers.21 It is well appreciated that postoperative mobilization of patients is time- and resource-intensive.5 Our findings show the significant need to implement, at an institutional level, more rigorous guidelines or protocols to encourage improvements in quality of care — including prompt mobilization following hip fracture surgery, especially for patients who experience a delay from admission to surgery. Similar to the conclusions by Goubar and colleagues,8 early mobilization should be used as a performance indicator for hip fracture care, with timing from admission to surgery being a key indicator of resource allocation.
Delayed time to mobilization also had a significant effect on the outcome in patients who had a higher prefracture frailty score. While patients with the highest frailty scores experienced the greatest benefit from early mobilization, they were routinely mobilized the latest. The frailty score was also found to have a significant effect on postoperative complication risk. Thus, while all patients should be mobilized within less than 48 hours, patients with a higher prefracture frailty score were mobilized later. It may be that nurses, physiotherapists and physicians are more apprehensive to mobilize these patients; however, the notion that these patients appear to benefit the most from early mobilization should be reinforced with the treatment team.22,23
The day of the week on which patients received their surgery had no effect on timing of mobilization or post-operative complication rate in our study. Our findings differ from those of previous studies that found a so-called “weekend effect,”24 whereby patients who received surgery on a weekend were mobilized later, and had higher rates of postoperative complications and higher mortality rates than patients who had their surgery on a weekday.24–26 It is likely that our findings are a result of the majority of patients on our ward being mobilized by nurses, who are present on weekends, instead of physiotherapists. Future research should test this question in a ward where the majority of mobilization is done by physiotherapists.
Limitations
This study had several limitations. As a retrospective review of prospectively collected data from a single academic centre, it is limited by all associated biases. Confounding variables (e.g., pain scores) that may have limited patients’ ability to mobilize early were not recorded. There were 137 patient records that could not be used owing to a lack of data regarding timing of mobilization. Data regarding a delay in timing of surgery as a result of direct oral anticoagulant use on admission were not obtained within ORFD. Timing of hospital admission was counted from the time at which patients first presented to the emergency department, regardless of which hospital. Thus, future research may want to investigate how a delay to surgery owing to hospital transfer affects time to surgery and subsequent postoperative outcomes. Finally, data regarding timing of postoperative complication relative to timing of postoperative mobilization were not collected. Future research may want to investigate how timing of postoperative complication affects time to mobilization.
Conclusion
We found that timing of mobilization should account for the total time spent immobilized before surgery. Timing of mobilization is a modifiable risk factor for developing a postoperative medical complication and is associated with LOS. Quality improvement efforts and increased adherence to guideline recommendations are necessary. Health care practitioners should also consider timing from admission to surgery when allocating resources to postoperative mobilization. Future studies are needed to establish the cost-effectiveness of investing into the necessary resources needed to support these endeavours. It is thus in the best interest of the patient, and perhaps the health care system, to work toward admitting patients into surgery and mobilizing patients postoperatively as soon as possible following a hip fracture.
Footnotes
This work has been presented at the 2022 American Academy of Orthopaedic Surgeons Annual Meeting, Chicago, Ill, Mar. 22–26, 2022, the Canadian Orthopaedic Association 2022 Annual Meeting, Québec, Que., June 8–11, 2022 and the 23rd European Federation of National Associations of Orthopaedics and Traumatology Annual Congress, Lisbon, Portugal, June 22–24, 2022.
Competing interests: None declared.
Contributors: C. Backman, J. Bourget-Murray, G. Grammatopoulos, I. Horton and S. Papp designed the study. O. Buth, M. Green, I. Horton and S. Papp acquired the data, which C. Backman, J. Bourget-Murray, G. Grammatopoulos, I. Horton and S. Papp analyzed. J. Bourget-Murray, G. Grammatopoulos and I. Horton wrote the article, which all authors reviewed. All authors approved the final version to be published.
- Accepted December 7, 2022.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use) and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/