Abstract
Background: Few studies have investigated the outcomes of surgical fracture care among socially deprived patients despite the increased incidence of fractures and the inequality of care received in this group. We evaluated whether socioeconomic deprivation affected the complications and subsequent management of marginalized/homeless patients following surgery for ankle fracture.
Methods: In this retrospective, population-based cohort study involving 202 hospitals in Ontario, Canada, we evaluated 45 444 patients who underwent open reduction and internal fixation (ORIF) for ankle fracture performed by 710 different surgeons between Jan. 1, 1994, and Dec. 31, 2011. Multivariable logistic regression models were used to assess the association between deprivation and shorter-term outcomes within 1 year (implant removal, repeat ORIF, irrigation and débridement owing to infection, and amputation). Multivariable Cox proportional hazards models were used to assess longer-term outcomes up to 20 years (ankle fusion and ankle arthroplasty).
Results: A higher level of deprivation was associated with an increased risk of irrigation and débridement (quintile 5 v. quintile 1: odds ratio [OR] 2.14, 95% confidence interval [CI] 1.25–3.67, p = 0.0054) and amputation (quintile 4 v. quintile 1: OR 3.56, 95% CI 1.01–12.4, p = 0.0466). It was more common for less deprived patients to have their hardware removed (quintile 5 v. quintile 1: OR 0.822, 95% CI 0.76–0.888, p < 0.0001). There was no correlation between marginalization and subsequent revision ORIF, ankle fusion, or ankle arthroplasty.
Conclusion: Marginalized patients are at a significantly increased risk of infection and amputation following surgical treatment of ankle fractures. However, these complications are still extremely uncommon among this group. Socioeconomic deprivation should not prohibit marginalized patients from receiving surgery for unstable ankle fractures.
Socially deprived patients face important barriers that reduce their access to care, presenting unique challenges for orthopedic surgeons.1 These patients experience unique health conditions, and disease severity is high because of factors including extreme poverty, delays in seeking care, nonadherence to therapy, mental health and substance abuse issues, and the adverse health effects of homelessness.1,2 Socially deprived patients are more likely to obtain their care in the emergency department than in an outpatient clinic.3 This is a substantial challenge for delivering efficient, cost-effective and patient-centred care.
Few studies have investigated the outcomes of surgical fracture care among socially deprived patients4–6 despite the increased incidence of fractures4 and the inequality of care received in this group. For example, Perry and colleagues7 found inequalities in the use of total hip arthroplasty for displaced intracapsular hip fractures in patients with higher levels of socioeconomic deprivation.
We studied a large population-based cohort of patients with ankle fracture to evaluate whether social deprivation affected the complications and subsequent management of marginalized or homeless patients following surgery for ankle fracture.
Methods
Data sources and setting
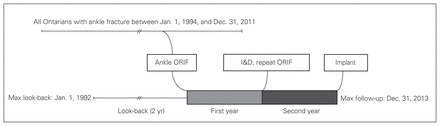
This was a population-based cohort study. Data were obtained from several health administrative databases reflecting patient encounters from 202 hospitals in Ontario, Canada. These databases are held securely in linked, encoded form, and data were analyzed at ICES. Surgeon billing codes linked to ankle fracture diagnostic codes were used to identify patients undergoing surgery for ankle fracture. The data sources and billing codes have been described in detail previously in the Appendix to a study by Pincus and colleagues.8 Our study design is depicted in Figure 1. The Research Ethics Board at Sunnybrook Health Sciences Centre approved our study protocol.
Study design. I&D = irrigation and débridement; ORIF = open reduction and internal fixation.
Cohort
The study population has been described previously.8 We chose to study ankle fractures because they are common injuries and their surgical management is typically performed in a nonelective setting. Patients older than 16 years undergoing isolated ankle open reduction and internal fixation (ORIF) in Ontario between Jan. 1, 1994, and Dec. 1, 2011, were eligible for inclusion. We excluded individuals who were not Ontario residents, were younger than 16 years, and had tibial plafond or bilateral ankle fractures. The beginning of the study period was selected to allow up to 2 years’ look-back for patient comorbidity score calculation and identification of tibial plafond fractures in the administrative databases that began data capture in 1992. Follow-up for each patient was at least 2 years and up to a maximum of 20 years (Dec. 31, 2013).
Outcomes
We considered 6 subsequent operations as indicators of surgical complications after ankle ORIF: implant removal in isolation (i.e., without repeat ORIF, irrigation and débridement, or amputation), repeat ORIF, irrigation and débridement owing to infection, lower extremity amputation within 1 year, ankle fusion and ankle arthroplasty. Surgical complications were assessed up to the end of the study period, up to maximum of 20 years.
Main exposure
Socioeconomic deprivation was measured for each patient according to their residential location by using the “deprivation” component of the Ontario Marginalization Index (ON-MARG).9 Neighbourhoods were sorted into quintiles, arranged from least (quintile 1) to most marginalized (quintile 5). Although there are limitations associated with quantifying socioeconomic deprivation based on address alone, the ON-MARG index takes into account several factors and has been shown to be associated with multiple health outcomes; previous research has found associations between the ON-MARG index and depression,10 smoking,11 alcohol consumption12 and body mass index.13
Covariates
We considered several patient, provider and surgical factors previously suggested to increase complication rates after ankle ORIF.14,15 Age and sex were analyzed as continuous and categorical variables, respectively. Comorbidities listed on hospital discharge abstracts in the 3 years before the index fixation procedure were categorized according to both the Charlson Comorbidity Index16 and Collapsed Aggregate Diagnosis Groups (CADGs).17 Previously validated algorithms identified patients with diabetes,18 hypertension19 and frailty17 at the time of their index procedure.
Index surgeon-related factors were assigned at patient entry into the cohort. These included surgeon experience (years since their Canadian orthopedic certification) and surgeon volume (the number of ankle ORIF procedures performed in the year preceding the index event). Surgeon volume was categorized by quintile. Index hospitals were categorized as either academic or nonacademic on the basis of their membership in the Council of Academic Hospitals of Ontario (www.cahohospitals.com). Surgical covariates identified using ICD-10 diagnosis codes and Ontario Health Insurance Plan (OHIP) billing codes included the presence of an open fracture, fracture–dislocation, and single-malleolar versus bi- and trimalleolar fractures. Finally, we categorized length of stay (LOS) as day surgery, 1-night stay, or > 1-night stay.
Statistical analysis
Descriptive statistics of baseline characteristics were calculated for the entire cohort and stratified by the presence of reoperation. These statstics include medians with interquartile ranges (IQRs) and proportions as appropriate. Unadjusted comparisons by deprivation status were made using Kruskal–Wallis and χ2 tests. Multivariable logistic regression models were used to assess the association between deprivation and implant removal, repeat ORIF, irrigation and débridement owing to infection, and amputation. Multivariable Cox proportional hazards (CPH) models were used to assess the association between deprivation and ankle fusion and ankle arthroplasty. Censoring for the CPH models occurred on death, emigration, loss of valid health care coverage, or the end of the follow-up period — whichever occurred first. Covariates included in each multivariable model were age, sex, comborbidity index, frailty, diabetes, LOS, surgeon experience and volume, hospital academic status, fracture–dislocation and open fracture. All analyses were performed using SAS software (version 9.3 and SAS EG 6.1, SAS Institute), and the type I error probability was set to 0.05.
Results
Baseline characteristics by deprivation
After exclusions, we identified 45 444 patients who underwent isolated ankle ORIF in Ontario during the study period (Fig. 2). Patients in the most deprived quintile had a significantly higher prevalence of diabetes and hypertension, higher CADG scores, and younger age (Table 1). Deprivation was also associated with longer hospital stays. Hospital LOS longer than 1 day occurred in 70.8% of patients in the most deprived quintile compared with 64.5% in the least deprived quintile (p < 0.001). Deprivation was not associated with sex, frailty, or a diagnosis of open fracture or ankle dislocation. Given the large sample size, the Deyo–Charlson scores, surgeon volume and experience, and hospital status reached statistical significance, but were unlikely to be clinically important factors.
Selection of patients for inclusion in the study.
Baseline characteristics by level of deprivation
Unadjusted outcomes by deprivation
The unadjusted outcomes by deprivation quintile are shown in Table 2. Deprivation was associated with an increased prevalence of irrigation and débridement for presumed infection (0.5% for quintile 5 v. 0.2% for quintile 1, p = 0.006) and amputation (0.2% for quintile 5 v. 0.1% for quintile 2, p = 0.028). Socially privileged patients were more likely to undergo hardware removal (19.6% for quintile 1 v. 17.1% for quintile 5, p < 0.001). Repeat ORIF was calculated separately for single-malleolar and bi- or trimalleolar ankle fractures. There was no correlation between marginalization and subsequent revision ORIF, ankle fusion, or ankle arthroplasty.
Outcomes by level of deprivation
Adjusted outcomes by deprivation
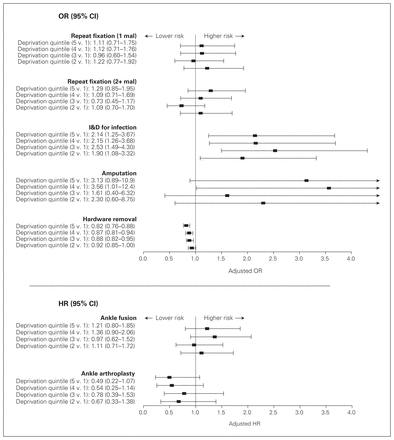
Deprivation was associated with an increased risk of requiring irrigation and débridement for infection (quintile 5 v. quintile 1: odds ratio [OR] 2.14, 95% confidence interval [CI] 1.25–3.67; Fig. 3). It was also more common for patients in quintile 4 than those in quintile 1 to require amputation (OR 3.56, 95% CI 1.01–12.4). Deprived patients were more likely to undergo a subsequent ankle fusion (hazard ratio [HR] 1.21, 95% CI 0.80–1.85) and less likely to undergo an ankle arthroplasty (HR 0.49, 95% CI 0.22–1.07) than patients in the lowest deprivation quintile, although the hazard ratios did not reach statistical significance.
Multivariable logistic regression and Cox proportional hazards models relating socioeconomic deprivation to surgical complications. Covariates included in each multivariable model were age, sex, Deyo–Charlson index, frailty, diabetes, length of stay (LOS), surgeon experience and volume, hospital academic status, fracture–dislocation, and open fracture. Adjusted odds ratios (ORs) and hazard ratios (HRs) are reported with 95% confidence intervals (CI). I&D = irrigation and débridement.
Discussion
We found a significant difference between the most and least deprived patients with regard to early repeat surgery, including irrigation and débridement for infection (p = 0.006) and amputation (p = 0.028). However, the overall risk of these complications for socially deprived patients was still low (0.5% and 0.2%, respectively). Our results suggest that while more deprived patients had a statistically significant increase in the risk of an infection, the overall ocurrance was uncommon. Therefore, the purported risk of infection or amputation should not preclude a socially deprived patient from operative management of an unstable ankle fracture. Similar to what has been reported previously in the literature on hip fractures, 7 our data also support the existence of some inequalities in provision of care for more deprived patients. More deprived patients were less likely to undergo removal of hardware; the reason is unclear, but may reflect a lack of follow-up for more deprived patients or a reluctance among surgeons to offer those patients a second surgery. We also noted trends in long-term data favouring ankle arthrodesis over ankle arthroplasty, but this finding did not reach statistical significance.
Implications
There are several practice interventions that may help improve care for marginalized patients and warrant further investigation.
Development of supportive housing/respite facilities for discharge of patients without secure housing. Most homeless patients are discharged to shelters or the street, which has a negative impact on postoperative care. Creating a secure housing facility to allow a safer environment in which to recuperate may decrease the mental and physical stresses of homeless patients.1,20
Fracture clinic screening program. A previous study found that homeless patients had more emergency department visits and fewer orthopedic clinic follow-up visits than nonhomeless patients.3 A comprehensive screening program similar to those used in elderly patients with fragility fractures21 may improve follow-up in the outpatient setting and reduce the risk of poorer clinical outcomes for marginalized patients. Screening may allow for increased use of outreach programs, connecting to social workers and community aid workers, ensuring safe discharge destinations, adhering to best practices and clinical practice guidelines, and encouraging close follow-up in the fracture clinic.22
Access to multidisciplinary clinics for follow-up of their fractures. Such clinics would give patients access to showers, foot and skin care, mental health services, substance abuse services, primary care, and adequate shoes/socks during their orthopedic assessments. The assertive community treatment model may improve care and decrease hospital admission.23,24
Prolonged period of protected immobilization and non–weight bearing. Early weight bearing on fractured limbs can contribute to nonunion and malunion. A plan for prolonged protection of weight bearing, like in patients with diabetes,25 may be beneficial for homeless patients with fractures.
Test alternative operative methods. Alternative surgical techniques include meticulous soft tissue handling, increased rigidity of fixation, use of locking plates, multiple tetracortical fibula-to-tibia screw fixation, percutaneous fixation, or primary joint fusion.25
An initial short-term recommendation is to leverage existing services in mental health, addictions management, and community agencies to create “homeless navigators.” These navigators would support community partnerships to ensure safe discharge and timely follow-up for patients with no fixed address. Additionally, in the short term, standards of care should be created for institutions who care for a high volume of homeless or marginalized individuals. The aim would be to minimize the risk of complications by standardizing care, including prolonged immobilization, more frequent wound checks, and optimizing nutritional status. Early identification of these patients will assist in adequate discharge planning and ensuring that patients receive timely follow-up.
Limitations
The population health data available through OHIP billing codes are limited in their ability to identify detailed injury and surgical predictors of reoperation. These predictors include the complexity of the initial fracture, the surgical technique used and the method of internal fixation. The details regarding postoperative management are also unavailable. However, a strength of this study is the ability of our public health care system to track patients up to 2 years postoperatively, even if they are lost to follow-up from their original surgeon, as long as they continued to be treated in Ontario and maintained their OHIP status. This is of particular relevance to tracking population-based outcomes in socioeconomically deprived patients.
It is also important to emphasize that our study focused on intermediate-term reoperation following ankle ORIF. We did not consider other adverse outcomes, such as wound complications treated nonsurgically, that may be clinically important in this population. Future work at the population level is also required to examine the outcomes of ankle fractures treated conservatively and whether surgeons avoid offering operative management to socially deprived patients. This may be best investigated using other study designs, such as qualitative studies, to assess potential surgeon bias toward socially deprived patients.
Conclusion
Marginalized patients are at increased risk of infection and amputation following surgery for ankle fractures. Socioeconomically advantaged patients are more likely to undergo removal of hardware. However, repeat irrigation and débridement and amputation were uncommon complications for both marginalized and nonmarginalized patients. Socioeconomic deprivation should not prohibit marginalized patients from receiving surgery for ankle fractures, but a high level of surveillance is required to identify and mitigate potential complications. Future prospective research should focus on the reasons for higher complication rates in marginalized patients and on the modifiable risk factors that could minimize complications.
Footnotes
Competing interests: None declared.
Contributors: J. Wolfstadt, D. Pincus and D. Wasserstein designed the study. D. Pincus and D. Wasserstein acquired and analyzed the data, which H. Kreder also analyzed. J. Wolfstadt and D. Pincus wrote the article, which all authors reviewed and approved for publication.
- Accepted November 8, 2018.