Abstract
Background: Rates of hospital readmission following surgery can serve as a marker for quality of care. The aim of this study was to establish the rates and causes of readmission and emergency department visits after vascular surgery and to understand how these patients are managed.
Methods: We conducted a prospective observational cohort study including all inpatients who underwent major vascular surgery between September 2015 and June 2016 at a tertiary vascular care centre in Toronto. Patients were followed at 30 days after discharge via telephone interview.
Results: We enrolled 133 patients (94 men [70.7%] and 39 women [29.3%] with a mean age of 65.3 years). The most common index admission diagnosis was peripheral artery disease (67 patients [50.4%]). At 30 days, 19 patients (14.8%) had been readmitted or had visited the emergency department, most commonly after lower extremity revascularization (19.4%). Ten patients were readmitted a mean of 16.8 days following discharge; surgical site infection was the most common cause for readmission (3 patients). The most common treatment was antimicrobial therapy (4 patients). The mean hospital length of stay was 14.4 days. Nine patients presented to the emergency department a mean of 10.6 days after discharge; 6 reported a wound issue, and most (6 of 9) were managed with oral antibiotic treatment.
Conclusion: Early readmission/emergency department visits after lower extremity revascularization surgery in patients with peripheral artery disease are common and are often due to surgical site infection or wound-related issues. Follow-up within 7–10 days and a specialized wound care team may help reduce the occurrence of these events.
Hospital readmission following major surgery is common and expensive and can serve as a marker for quality of care provided. In 2004, nearly 1 in 5 Medicare beneficiaries were readmitted to hospital within 30 days of discharge, costing an estimated US$17.4 billion.1 Some studies suggest that hospital readmission may be preventable, although the actual proportion of potentially preventable readmissions is unclear.2–4 Furthermore, several federal agencies, clinicians and health policy-makers recently identified the reduction of hospital readmissions as a major area of research focus.5–7
Several authors have studied the rate of readmission following major vascular surgical procedures.8–12 Such procedures are reported to yield the highest rates of hospital readmission of all surgical groups1,13 and the third-highest of any diagnosis-related group.1 However, these observations are predominantly from the United States and are derived mostly from administrative databases or registries.8,9,11,14,15 Canadian data are limited, and little prospective work has been done to assess readmission rates following major vascular surgery, particularly from large tertiary centres that receive patients from a wide geographic catchment area because of critical referrals. The aim of this study was to determine the rates of 30-day hospital readmission and emergency department visits following major vascular surgery in a Canadian context.
Methods
Setting and design
We conducted a prospective observational cohort study of consecutive patients who underwent major vascular surgery between September 2015 and June 2016 at St. Michael’s Hospital, Toronto, a tertiary health care centre with a specialized vascular surgery division. Research ethics approval was obtained from St. Michael’s Research Ethics Board. The consent requirement was waived by the board on the basis that this study pertains to a quality-improvement initiative. As such, all patients who met the eligibility criteria were automatically enrolled in the study, with the option of withdrawal. A letter was included in each eligible patient’s discharge package outlining the study and the withdrawal process. Patients also had the opportunity to drop out during the follow-up telephone call.
Participants
All consecutive patients who underwent elective or emergent major inpatient vascular surgery procedures between September 2015 and June 2016 were eligible, including those who were transferred from another institution. Procedures included lower extremity revascularization, upper extremity/neck procedures, open aortic repair, endovascular aortic repair and lower extremity amputation. Patients who had undergone same-day procedures, such as but not limited to saphenous vein stripping and creation of arteriovenous dialysis access, were not eligible. Patients in whom a same-day procedure was initially planned but who were unexpectedly admitted because of unforeseen circumstances were also excluded. A vascular surgery nurse practitioner and research study personnel reviewed the daily vascular surgery discharge census for eligibility.
Data collection
We first collected baseline data using physical patient charts and electronic medical records at the time of patient discharge. Baseline covariates included age, sex, medical comorbidities (e.g., hypertension, dyslipidemia, diabetes, peripheral artery disease), distance of patient’s residence from treating hospital, previous surgical procedure(s), admission diagnosis, length of stay, type and urgency of the procedure performed, location of incision, type of wound, patient disposition, use of antibiotics and planned follow-up.
Outcome measures and follow-up
The primary outcome was a composite rate of hospital readmission or emergency department visit within 30 days after discharge. We examined reasons for hospital readmission/emergency department visit and management received as secondary outcomes. Follow-up at 30 days after discharge was conducted via telephone interview. A maximum of 3 telephone follow-up interviews were attempted per patient. If a patient was unreachable after these attempts, he/she was considered lost to follow-up. Follow-up data were collected by means of a telephone script, supplemented with electronic medical record review, if required. In addition, we collected information on the timing of readmission/emergency department visit, length of stay after readmission and follow-up visits completed with health care professionals after discharge.
Statistical analysis
We conducted univariate analyses using means with standard deviations (SDs) for continuous variables and frequencies with proportions for categorical variables of the baseline characteristics, procedure- and hospital-related factors, and follow-up and outcome data. We also conducted bivariate analyses using the Pearson χ2 test to calculate stratified rates of readmission/emergency department visits by type of index procedure, distance of patient residence from the treating hospital, and urgent or elective procedure. Significance was set to p < 0.05. All statistical analyses were carried out with Stata/MP version 13 (StataCorp).
Results
A total of 133 patients were enrolled in the study, of whom 128 (96%) received 30-day follow-up. Two of the 5 patients who did not receive 30-day follow-up died, and 3 were still in a hospital or rehabilitation setting at the time of follow-up.
Baseline characteristics
The baseline characteristics of the study population are shown in Table 1. There were 94 men (70.7%) and 39 women (29.3%) with a mean age of 65.3 (SD 13.1) years. Most patients (100 [75.2%]) resided 50 km or less from the treating hospital. The most prevalent medical comorbidities were hypertension (101 patients [75.9%]) and dyslipidemia (79 [59.4%]). The most common index admission diagnoses were peripheral artery disease (67 patients [50.4%]), abdominal aortic aneurysm (31 [23.3%]) and carotid stenosis (12 [9.0%]) (Table 2). Lower extremity revascularization (50 patients [37.6%]), upper extremity/neck procedure (25 [18.8%]) and lower extremity amputation (24 [18.0%]) were the most common index procedures performed. Urgent or emergent procedures accounted for 50 (37.6%) of the index procedures. The mean hospital length of stay was 11.1 (SD 12.2) days. Most patients (104 [78.2%]) were discharged home. Antibiotics were prescribed to 28 patients (21.0%) at discharge.
Baseline patient characteristics
Characteristics of index admission and discharge
Primary outcome
At the time of 30-day follow-up, 3 patients were still in a hospital or rehabilitation setting, and 2 patients had died. Of the 128 patients who received 30-day follow-up, 127 (99.2%) had had a follow-up visit with a health care professional after discharge (vascular surgeon in 125 cases [97.7%], family doctor in 15 [11.7%], wound care nurse in 4 (3.1%) and other in 30 [23.4%]).
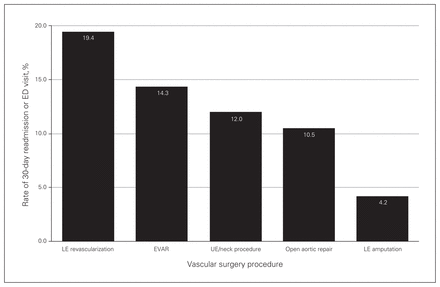
Of the 128 patients, 19 (14.8%) had been readmitted to hospital (n = 10) or had visited the emergency department (n = 9) within 30 days of discharge. One of the 19 was readmitted to another hospital but did not require transfer back to our institution. The rate of readmission/emergency department visit differed by index procedure, distance of patient residence from treating hospital and urgency of index procedure. The rate was highest among patients who had undergone lower extremity revascularization (19.4%) and lowest among those who had undergone lower extremity amputation (4.2%) (Fig. 1). Patients who lived 50 km or less from the treating hospital had a rate of readmission/emergency department visit of 12.0%, and those who lived more than 50 km away had a rate of 21.2%. The rate was 10.8% among elective cases and 20.0% among urgent cases. None of these comparisons were statistically significant (p > 0.05 for all).
Rate of 30-day hospital readmission or emergency department visit by index procedure. Note: ED = emergency department; LE = lower extremity; EVAR = endovascular aortic repair; UE = upper extremity.
Secondary outcomes
The 10 patients were readmitted a mean of 16.8 (SD 8.4) days after discharge (Table 3). The most common readmission diagnoses were surgical site infection (3 patients) and gastrointestinal complications (2). These diagnoses were most often treated with antimicrobial therapy (in 4 cases) and by surgical intervention (in 3). The mean hospital length of stay was 14.4 (SD 11.1) days.
Characteristics of readmission and emergency department visits
The 9 patients visited the emergency department a mean of 10.6 (SD 6.4) days following discharge (Table 3). The most common diagnoses for these visits were wound complications (6 patients) and lower extremity edema (2). Six patients were managed with oral antibiotic therapy, and 3 were reassured that no medical treatment (such as antibiotics) was needed for their wound.
Patients who received an antibiotic prescription at discharge had a higher rate of readmission/emergency department visits (7/28 [25%]) than did those who were not prescribed antibiotics at discharge (12/105 [11.4%]); however, the difference was not statistically significant (p = 0.07). Also, the rate of readmission/emergency department visits was higher among patients with diabetes (15.6%) than among those without diabetes (13.6%), but not significantly so (p = 0.8).
Discussion
In this single-centre prospective cohort study, the rate of readmission/emergency department visits among inpatients following major vascular surgery was 15%. The rate was highest among patients with peripheral artery disease who underwent lower extremity revascularization. The most common cause for readmission was surgical site infection, and wound complications accounted for two-thirds of emergency department visits after discharge. Not surprisingly, antibiotics were the most common treatment among patients who were readmitted to hospital or discharged from the emergency department. We also found that patients tended to present to hospital within 11–14 days of discharge, which indicates that earlier follow-up may be beneficial. Therefore, these findings lead us to hypothesize that specialized, targeted strategies such as early wound assessment within 7–10 days of discharge may help prevent emergency department visits or readmission following major vascular surgery.
Several authors have reported rates of readmission after individual vascular procedures, such as abdominal aortic aneurysm repair (8%–54%),14–16 amputation (9%–18%),17–19 and lower extremity bypass (12%–49%).8,9,11,20,21 However, there are conflicting reports regarding readmission rates and reasons. Merkow and colleagues22 found that, among about 500 000 operations identified in the American College of Surgeons National Surgical Quality Improvement Program database, surgical site infection was the most common cause (20%) of 30-day readmission. The rate was even higher (36%) among patients who underwent lower extremity bypass operations. However, lower extremity vascular bypass surgery was the only vascular procedure examined in that study; data with regard to other vascular procedures were not available. Engelbert and colleagues23 investigated the association between readmission and patient or clinical characteristics in a large tertiary hospital. They reported a same-institution readmission rate of 9.7%, with below-knee amputation (25%), foot amputation (22%) and lower extremity revascularization procedures (22%) accounting for most cases of readmission. This is a noteworthy disparity with our findings, as we observed considerably higher readmission rates among patients who underwent lower extremity revascularization than among those who underwent amputation. Owing to the retrospective nature of their study, Engelbert and colleagues23 were unable to capture readmission to other institutions. Jackson and colleagues24 retrospectively studied 30-day readmission rates among 799 live patients discharged from a university-affiliated hospital after vascular surgery. They reported a 30-day readmission rate of 11.9%; the most common cause for readmission was wound complication. Similar to our study, patients who underwent open lower extremity revascularization had the highest rates of 30-day readmission (15%).
Readmission rates may also vary by hospital volume. Tsai and colleagues25 used national Medicare data to calculate 30-day readmission rates for 6 index procedures, 3 of which were major cardiovascular procedures (coronary artery bypass grafting, endovascular aortic aneurysm repair and open aortic aneurysm repair). They found that hospitals in the lowest quartile for surgical volume had a significantly higher readmission rate than hospitals in the highest quartile for surgical volume (17% v. 13% in an adjusted multivariate model). Furthermore, hospitals in the lowest quartile for death had significantly fewer readmissions than those in the highest quartile for death (13% v. 14% in an adjusted multivariate model). Overall, the readmission rate at our centre (15%) is comparable to rates observed in other high-volume centres in the US.25
Numerous strategies have been proposed to reduce the occurrence of 30-day readmission and emergency department visits, but the efficacy of these interventions is debatable. In populations of general medical patients, pharmacist telephone follow-up 2 days after discharge,26 coordination of discharge planning by a nurse discharge advocate and pharmacist telephone follow-up 2 days after discharge,27 and 24-week exercise programs led by nurses and physiotherapists combined with telephone follow-up28 have all been shown to significantly curtail rates of 30-day hospital readmission/emergency department visits in controlled trials. Other strategies, such as enhancement of hospital care and patient discharge by a clinical nurse specialist,29 discharge facilitators on resident teams,30 and telephone follow-up calls at 1 week and 1 month,31 did not reduce 30-day readmission rates among such patients. In a systematic review investigating interventions designed to lower 30-day readmission rates, no single intervention was identified that could consistently reduce these rates.32 Moreover, most of these interventions were developed and stipulated for the US health care system. Given the considerable differences between the Canadian and US health care systems, the effectiveness of these strategies in the Canadian health care system remains to be established. Our findings indicate that vascular surgeons should consider following patients with peripheral artery disease in particular within 7–10 days after discharge to assess and manage wound-related issues. This strategy may lead to a reduction in unnecessary hospital visits. It is, however, unclear from our study whether telephone- or computer-based, nurse-led or traditional clinical follow-up strategies are best. At our centre, the vascular administrative assistants are available during daytime hours to answer telephone calls from patients who are experiencing postdischarge issues. When required, these administrative assistants facilitate urgent clinic visits with vascular surgeons. However, it is unclear whether this leads to lower rates of hospital readmission or emergency department visits.
Given the apparent difficulty in reducing the occurrence of hospital readmission, it is becoming increasingly important for policy-makers to discuss whether high readmission rates actually imply poor quality of care and whether hospitals should be penalized for them. Moreover, the claim that 30-day hospital readmission serves as a marker for quality of care is contestable, as important factors such as mortality rates are often overlooked.6,7
Our findings have important implications. First, they reiterate the high prevalence of hospital readmission/emergency department visits after vascular surgery procedures. Patients with peripheral artery disease appear to be at higher risk for readmission, likely owing to a combination of patient (e.g., sedentary lifestyle, smoking, diabetes) and procedural (e.g., groin incision, use of prosthetic material, long procedure time) factors. This highlights the importance of effective guideline-recommended risk-reduction programs for patients with peripheral artery disease, which may reduce the risk of adverse limb outcomes.33 Second, the results support the formulation of public health campaigns against peripheral artery disease, especially in light of the large knowledge gap present within the Canadian public.34 Last, this study highlights the need for the development of effective outpatient quality-improvement initiatives for patients undergoing vascular surgery stipulated for the Canadian health care system, particularly targeting early wound assessment and management after surgery.
Strengths and limitations
A major strength of our work is that it was a prospective study. To the best of our knowledge, most previous studies of readmission after a major vascular procedure have been retrospective and/or registry based. The main advantage of the prospective design of our study was that it allowed us to follow all patients at 30 days and establish accurate rates of 30-day readmission and emergency department visits with minimal risk of ascertainment bias. In contrast, retrospective studies may be biased by incomplete follow-up and may underrecognize hospital readmission or emergency department visits. Furthermore, the prospective design allowed us to capture readmission to other institutions, which is not always possible in single-centre retrospective studies.
Our study has a few limitations. First, because it was conducted in a single tertiary hospital, the results may have poor generalizability. However, we included a broad range of vascular surgical procedures, which is likely representative of contemporary vascular surgery practice in other Canadian tertiary vascular care centres. Second, the study may have been underpowered owing to the small sample. Third, we did not collect data on the proportion of patients with wound infection who were treated successfully as outpatients outside of the emergency department or hospital setting. Fourth, our data may have been subject to recall bias, as follow-up was at 30 days after discharge via a telephone call. However, we supplemented information obtained from patients with medical record data for completeness.
Conclusion
Our results suggest that readmission to hospital and/or emergency department visits after vascular surgery in a high-volume single tertiary vascular centre are fairly common, occurring most often within 2 weeks after procedures of the lower extremity among patients with peripheral artery disease. For this patient population, we hypothesize that having a specialized wound care team that is primarily responsible for early (within 7–10 d after discharge) wound assessment may reduce rates of hospital readmission and emergency department visits after vascular surgery.
Acknowledgement
The authors thank Areesha Satti for assistance with data collection.
Footnotes
This study was presented in part at the 39th Annual Meeting on Vascular Surgery, hosted by the Canadian Society for Vascular Surgery, Sept. 15–16, 2017, Banff, Alta.
Competing interests: None declared.
Contributors: M. Hussain, Z. Khoshhal and M. Al-Omran designed the study. M. Hussain, Z. Khoshhal, B. Altuwaijri and B. Hughes acquired the data, which M. Syed, M. Hussain, Z. Khoshhal, K. Salata, N. Alsaif, C. de Mestral, S. Verma and M. Al-Omran analyzed. M. Syed wrote the article, which all authors reviewed and approved for publication.
- Accepted November 22, 2017.