Abstract
Background: Hip fractures are common injuries that result in blood loss and frequently require the transfusion of blood products. We sought to identify risk factors leading to increased blood transfusion in patients presenting with hip fractures, especially those factors that are modifiable.
Methods: We retrospectively reviewed the cases of all patients who had fixation of their hip fractures between October 2005 and February 2010. The need for transfusion was correlated with potential risk factors, including age, sex, preoperative hemoglobin, fracture type, fixation method and more.
Results: A total of 835 patients had fixation of their hip fractures during the study period; 631 met the inclusion criteria and 249 of them (39.5%) were transfused. We found an association between need for blood transfusion and female sex (p = 0.018), lower preoperative hemoglobin (p < 0.001), fracture type (p < 0.001) and fixation method (p < 0.001). Compared with femoral neck fractures, there was a 2.37 times greater risk of blood transfusion in patients with intertrochanteric fractures (p < 0.001) and a 4.03 times greater risk in those with subtrochanteric fractures (p < 0.001). Dynamic hip screw (DHS) fixation decreased the risk of transfusion by about half compared with intramedullary nail or hemiarthroplasty. We found no association with age, delay to operation (p = 0.17) or duration of surgery (p = 0.30).
Conclusion: The only modifiable risk factor identified was fixation method. When considering blood transfusion requirements in isolation, we suggest a potential benefit in using a DHS for intertrochanteric and femoral neck fractures amenable to DHS fixation.
Hip fractures are among the most common fractures treated by orthopedic surgeons. With increasing life expectancy, it is estimated that the number of people aged 65 and older will increase from the recent estimate of 323 million to 1555 million by the year 2050. As a result, it is estimated that the number of hip fractures occurring worldwide will increase from 1.66 million in 1990 to 6.26 million in 2050.1
Hip fractures result in blood loss and frequently require the transfusion of blood products. While blood transfusions are potentially life-saving interventions, they can also cause patient morbidity. Blood transfusions are correlated with an increased risk of bacterial infections2–7 and possibly increased mortality.8,9 There are also substantial costs involved in the collection, preparation, transport and administration of blood.
In the United States, more than 15 million units of blood are transfused annually.10 Many of these transfusions are given to surgical patients, including elderly patients with hip fractures. We sought to determine whether any modifiable risk factors for transfusion exist. The purpose of this study, therefore, was to assess risk factors for blood transfusion requirements in patients presenting with hip fractures. We performed a retrospective study at a single level I trauma centre from 2005 to 2010. Blood transfusion requirements were correlated with patient variables, such as age, sex, delay to surgery, duration of surgery, preoperative hemoglobin, fracture type and fixation method.
Methods
All patients undergoing surgical fixation of their hip fractures in a single academic trauma centre between October 2005 and February 2010 were included in this retrospective study. The fracture patterns included were femoral neck, intertrochanteric and subtrochanteric fractures. Fixation methods used included hemiarthroplasty, dynamic hip screw (DHS), cannulated screws and cephalomedullary nails. The study was approved by our institution’s review board. All patient information, including laboratory values and operative notes, were collected from our institution’s electronic patient database, Powerchart (Cerner Corporation). Blood transfusion information was collected from our institution’s blood transfusion laboratory.
The type of hip fracture was documented based on review of patients’ preoperative and postoperative radiographs. These included femoral neck fractures (AO-OTA 31-B1–3), intertrochanteric fractures (AO-OTA 31-A1–3) and subtrochanteric fractures (AO-OTA 32A,1–3 32-B[1–3] and 32-C[1–3]). Surgical fixation was documented based on review of patients’ preoperative and postoperative radiographs. The DHS used was from Synthes. All hemiarthroplasties were performed with the Conquest system (Smith & Nephew) through a standard Hardinge approach. The intramedullary nails were either Trigen or Intertan (both from Smith & Nephew). The cannulated screws were 7.3-mm screws (Synthes Inc). The following measures were recorded from the patients’ electronic charts: sex; age; American Society of Anesthesiologist (ASA) score; duration of surgery; and need for preoperative, intraoperative and postoperative blood transfusion. Time from admission to operation was also documented and was defined as the time from admission to our institution’s emergency department to the start of the operation. Criteria for administration of blood transfusion were a hemoglobin value less than 70 g/L or less than 80 g/L with signs/symptoms of anemia.
Patients were excluded from this study if they were younger than 60 years; had a known cancer in the region of the fracture; had a hemorrhagic complication in another anatomic site, such as a gastrointestinal bleed, pre- or postoperatively; were admitted to hospital for other clinically important comorbidities, such as sepsis or polytrauma; were undergoing revision surgery; had an intraoperative complication, such as a trochanteric fracture; were therapeutically anticoagulated or had documented hematologic disease before surgery; or had a delay in diagnosis of their fracture longer than 1 week.
Notably, all patients received thromboembolic prophylaxis with 5000 units of low molecular-weight heparin (dalteparin sodium, Pfizer Canada). This therapy was started on admission, withheld on the day of surgery and restarted on the first postoperative day.
Statistical analysis
We performed our statistical analyses using SPSS software. We conducted a univariate analysis of all independent variables (i.e., age, sex, duration of surgery, preoperative hemoglobin level, fracture type, fixation method) to establish an association with blood transfusion requirement. Variables that were found to have a significant association were then included in a multivariate analysis. We considered results to be significant at p < 0.05.
Results
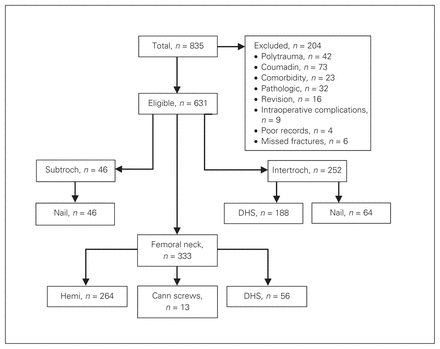
A total of 835 patients had fixation of their hip fractures during the study period; 631 patients met the inclusion criteria (Fig. 1). Forty-one patients were excluded because of multiple injuries, 73 patients were anticoagulated, 32 had pathologic or pending pathologic fractures, 23 had a significant hemorrhagic complication unrelated to their hip fracture, 16 underwent revision surgery, 9 experienced an intraoperative complication, 4 were excluded because of poor documentation and 6 were delayed to surgery because the fracture diagnosis was delayed longer than 1 week (Fig. 1).
Patients meeting inclusion criteria. Cann screws = cannulated screws; DHS = dynamic hip screw; hemi = hemiarthroplasty; intertroch = intertrochanteric fracture; nail = intramedullary nail; subtroch = subtrochanteric fracture.
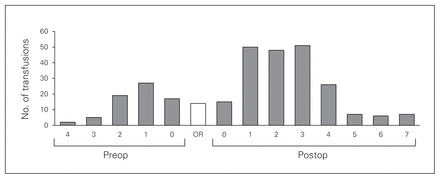
The mean age was 81.6 (range 60–100) years. The sample comprised 455 women (72.1%, mean age 82.4 yr) and 176 men (27.9%, mean age 79.3 yr; Table 1). The mean delay from admission to surgery was 48.9 hours. Of the 631 patients in the study, 249 patients were transfused (39.5%). This group included 26% of patients with femoral neck fractures, 52% with intertrochanteric fractures and 71% with subtrochanteric fractures. The majority of blood transfusions were administered on postoperative day 1, 2 or 3 (Fig. 2).
Number of patients receiving blood transfusions preoperatively, intraoperatively and postoperatively. Most transfusions were performed on postoperative day 1, 2 or 3. OR = intraoperative transfusion; preop 0 = preoperative transfusion day of surgery; postop 0 = postoperative transfusion day of surgery.
Characteristics of study participants
The results of the univariate analysis are presented in Table 2. The 13 patients with femoral neck fractures treated with cannulated screws were removed from the analysis because of the small number of patients. The univariate analysis demonstrated an association between need for blood transfusion and increased age (p = 0.004), female sex (p = 0.018), lower preoperative hemoglobin level (p < 0.001), fracture type (p < 0.001) and fixation method (p < 0.001). Patients requiring a blood transfusion had an average ASA score of 3.4, whereas patients not receiving a transfusion had an average score of 3.3 (p < 0.001). We found no association with delay to operation (p = 0.17) or duration of surgery (p = 0.30).
Univariate logistic regression analyses to predict transfusion, n = 618
Multivariate analysis demonstrated an association between blood transfusion requirement and 3 variables (Table 3). Men were at half the risk of women (1.54 odds ratio [OR], 95% confidence interval [CI] 1.002–2.36, p = 0.049). For every 10 g/L increase in preoperative hemoglobin, the risk of transfusion decreased by about 30% (OR 0.69, 95% CI 0.61–0.78, p < 0.001). Femoral neck fractures treated with DHS reduced the risk of transfusion by half compared with hemiarthroplasty (OR 0.49, 95% CI 0.61–0.78), and intertrochanteric fractures treated with DHS reduced the risk of transfusion by half compared with intramedullary nail (OR 0.52, 95% CI 0.29–0.95). This indicates that DHS fixation in either femoral neck fractures or intertrochanteric fractures decreases the risk of transfusion by about half compared with treatment with an intramedullary nail or hemiarthroplasty.
Multivariable analyses to predict transfusion. Logistic regression with only those variables that were significant at p = 0.05 in univariate analyses, n = 618
Discussion
We found a correlation between blood transfusion requirement and sex, preoperative hemoglobin, ASA score, fracture type and fixation method. No correlation was found with age, duration of surgery or delay from admission to operation.
Low preoperative hemoglobin is an independent risk factor for the need for blood transfusion. In the present study, preoperative hemoglobin was 112.0 ± 14.3 g/L in transfused patients and 122.1 ± 15.8 g/L in those not transfused (p < 0.001). Multivariate analysis showed that for every 10 g/L decrease in hemoglobin, patients had a 30% increased risk of blood transfusion (p < 0.001). This is consistent with a study by Adunsky and colleagues,11 who studied blood transfusion patterns in 302 patients with hip fractures. They found that a hemoglobin value less than 12 g/dL (120 g/L) increased transfusion risk 5-fold. They suggested that patients with a hemoglobin greater than 12 g/dL (120 g/L) did not require crossmatching preoperatively. Other studies have also identified low preoperative hemoglobin as a risk factor for transfusion.12–15
Our univariate analysis showed that older patients were more likely to receive a blood transfusion, but age was not important in our multivariate analysis, which suggests that other factors explain the same variability in need for transfusion as age but were even more predictive. The average age of patients in our study who received a blood transfusion was 83.1 ± 7.9 years compared with 80.9 ± 9.0 years in patients who did not (p < 0.003). Swain and colleagues16 studied the transfusion requirements for 249 patients with femoral neck fractures and found that patients aged 80 years and older were transfused significantly more than those aged younger than 80 years. Similarly, Dillon and colleagues12 found that patients older than 75 years were at higher risk of receiving blood transfusion.
Patients receiving a blood transfusion had an average ASA score of 3.4 compared with 3.3 in patients who did not receive a transfusion (p < 0.001). This result was significant; however, it is difficult to determine the clinical significance with such a minor difference between scores (0.1). Previous studies examining ASA scores and transfusion requirements did not find any association.11,12
Delay from admission to operation in elderly patients with hip fractures carries significant morbidity and mortality. Delay from admission to operation has been shown to increase mortality,17–19 postoperative infections19,20 and length of stay in hospital.20–22 However, the present study did not find a correlation with delay to operation and transfusion requirements. One would assume that while a patient is awaiting surgery, continued blood loss would be present at the fracture site, leading to greater blood loss and greater risk of transfusion. The equivocal risk of transfusion found in our study may be related to the formation of hematoma around the fracture site. The delay to surgery may have allowed the fracture hematoma to fully stabilize, minimizing the active bleeding before surgery. Intraoperatively, this may have resulted in less surgical blood loss and a lower rate of blood transfusion.
When comparing fracture types, patients with intertrochanteric or subtrochanteric fractures were at an increased risk of requiring a blood transfusion. When compared with femoral neck fractures, there was a 2.37 times greater risk of blood transfusion in patients with an intertrochanteric fracture (p < 0.001) and a 4.03 times greater risk in patients with a subtrochanteric fracture (p < 0.001). These results are consistent with those of Adunsky and colleagues,11 who found that patients with pertrochanteric fractures were transfused significantly more than patients with subcapital fractures. Swain and colleagues16 also found an increased transfusion requirement in patients with intertrochanteric fractures compared with those with intracapsular fractures, and Dillon and colleagues12 reported an increased risk for blood transfusion in patients with pertrochanteric fractures.
When comparing fixation methods for the different fracture types, we found a significant difference in blood transfusion requirements. In patients with femoral neck fractures, 24.8% treated with hemiarthroplasty were transfused compared with 14.3% of patients treated with DHS (p < 0.001). This may be partially related to severity of injury, as the more displaced fractures were likely treated with hemiarthroplasty. This finding is consistent with those of a meta-analysis performed by Wang and colleagues,23 who compared the outcomes of patients who underwent arthroplasty with those of patients who underwent internal fixation for displaced femoral neck fractures. They found greater operative blood loss and increased transfusion requirement in the hemiarthroplasty group. Similarly, Parker and colleagues24 found lower operative blood loss and lower transfusion requirements with internal fixation (using cannulated screws) than with hemiarthroplasty in patients with displaced femoral neck fractures. Similar to femoral neck fractures, intertrochanteric fractures treated with a DHS had a lower risk of transfusion than those treated with an intramedullary device. In our study, 37.9% of intertrochanteric fractures treated with a DHS were transfused compared with 51.6% treated with an intramedullary device (p < 0.001). The literature comparing blood loss in intertrochanteric hip fractures treated with intramedullary nail or DHS is inconclusive. Authors have reported reduced blood loss,25–27 increased blood loss28 and no difference29,30 in patients with intertrochanteric fractures treated with an intramedullary nail. The variability among studies may be related to differences in fracture severity, as patients with more displaced fractures are generally more likely to be treated with an intramedullary device.
Limitations
There are limitations to this study that should be considered. First, there may be inherent differences in medical comorbidities between the transfused and nontransfused patient samples that were not discerned by this retrospective, observational study. As mentioned, we attempted to stratify by ASA score, but it is difficult to determine if such a small difference in ASA score between groups has any clinical importance. Second, patients were generally given a transfusion based on the criteria of hemoglobin less than 70 g/L or less than 80 g/L with signs/symptoms of anemia. This threshold is consistent with the restrictive strategy group in a study by Carson and colleagues,31 who compared restricted and liberal transfusion thresholds. Similar to Carson and colleagues,31 we attempted to make the decision to transfuse as uniform as possible; however, there are difficulties with this. Determining signs/symptoms of anemia is subjective, and a lack of uniformity inherently exists among treating physicians. This may have resulted in some inconsistencies in decision to transfuse. Finally, we did not separately analyze patients with stable and unstable intertrochanteric fractures. One would assume that 3- and 4-part intertrochanteric fractures are most likely to cause greater blood loss and more likely to be treated with an intramedullary device. This would potentially affect the results of transfusion requirements between the intramedullary nail and DHS groups. However, previously published literature has failed to find convincing evidence of greater blood loss in patients with unstable fracture patterns.32,33
Conclusion
We found a correlation with blood transfusion requirement and sex, preoperative hemoglobin, fracture type and fixation method. The only modifiable risk factor found in the present study was fixation method. Further studies would be beneficial to determine other potential modifiable risk factors. Based on our findings, when considering blood transfusion requirements in isolation, we suggest a potential benefit in using a DHS for intertrochanteric and femoral neck fractures amenable to DHS fixation.
Footnotes
Competing interests: None declared.
Contributors: S. Desai, D. Bryant, A. Lawendy and D.W. Sanders designed the study. S. Desai, K.S. Wood and H. Abdo acquired the data, which S. Desai, J. Marsh, D. Bryant and A. Lawendy analyzed. S. Desai wrote the article, which all authors reviewed and approved for publication.
- Accepted April 7, 2014.