Abstract
Background: Surgical residency has the reputation of being arduous and stressful. We sought to determine the stress levels of surgical residents, the major causes of stress and the coping mechanisms used.
Methods: We developed and distributed a survey among surgical residents across Canada.
Results: A total of 169 participants responded: 97 (57%) male and 72 (43%) female graduates of Canadian (83%) or foreign (17%) medical schools. In all, 87% reported most of the past year of residency as somewhat stressful to extremely stressful, with time pressure (90%) being the most important stressor, followed by number of working hours (83%), residency program (73%), working conditions (70%), caring for patients (63%) and financial situation (55%). Insufficient sleep and frequent call was the component of residency programs that was most commonly rated as highly stressful (31%). Common coping mechanisms included staying optimistic (86%), engaging in enjoyable activities (83%), consulting others (75%) and exercising (69%). Mental or emotional problems during residency were reported more often by women (p = 0.006), who were also more likely than men to seek help (p = 0.026), but men reported greater financial stress (p = 0.036). Foreign graduates reported greater stress related to working conditions (p < 0.001), residency program (p = 0.002), caring for family members (p = 0.006), discrimination (p < 0.001) and personal and family safety (p < 0.001) than Canadian graduates.
Conclusion: Time pressure and working hours were the most common stressors overall, and lack of sleep and call frequency were the most stressful components of the residency program. Female sex and graduating from a non-Canadian medical school increased the likelihood of reporting stress in certain areas of residency.
Previous research has concluded that medical residents experience increased levels of symptoms associated with stress during residency.1–4 They are required to be excellent clinicians, educators and researchers.1 Residents have reported feeling less humanistic and experiencing various psychological symptoms.1 Although not much research has been completed specifically on the stress of surgical residency, this area of research has become of great concern to those in charge of residency programs. A study from Belgium conducted biological tests to measure stress hormones, such as cortisol, and found that medical residents had high levels of cortisol, indicating high levels of stress.5 Lack of sleep is a common problem among medical residents and can lead to a variety of health issues.6 Although some level of stress might be a motivating and beneficial factor in the success of medical trainees, substantially high levels of stress have led to cases of suicide, increasing the demand for and interest in research on how the stress levels of medical residents can be decreased.7,8
Some studies have reported differences in how male and female residents coped with their stress, whereas others reported no such findings.9 Furthermore, some studies have reported on residents’ methods for reducing feelings of stress. Methods such as maintaining a positive attitude, staying in relationships and having religious beliefs have all been reported to have positive outcomes in decreasing stress levels during residency.10 To our knowledge, there are no reports on the stress level and methods of coping with stress specifically among surgical residents. We developed a survey to investigate the levels of stress experienced by surgical residents in different programs across Canada and to highlight the major causes of their stress and their coping mechanisms.
Methods
We used a descriptive survey design. Stress for the purpose of this study was defined as the body’s reaction to a change that requires a physical, mental or emotional adjustment or response. To assess stress, we designed and distributed a survey to surgical residents across Canada. We followed a detailed and specific method to create our questionnaire so that it would be relevant to surgical residents and objectively guide the participants to express their level of stress and its cause in a quantitative manner. We searched the literature for the previously published surveys in a similar study population.1,5–7,9,10 We used the questionnaire from Cohen and Pattern9 and added some more questions relevant to our study population. Our modified questionnaire posed general, stress-related and health-related questions on topics normally known to be correlated with stress in the workplace. The survey questions were reviewed by the authors on different occasions and changes were made. The final copy was tested for face and content validity before we conducted the survey. Local surgeons, surgical residents and research experts at the department of surgery at McMaster University, Hamilton, Ont., were asked to review the questionnaire for clarity and to determine whether the questionnaire satisfied the planned objectives. These reviewers were asked to consider whether the questionnaire included all relevant content and domains. Suggestions were reviewed and changes were made to the questionnaire. The final questionnaire is available online in Appendix 1 at cma.ca/cjs. An email was sent to the 600 Canadian surgical residents in the 2008 academic year asking them to complete the online survey using Survey Monkey. We received the list of all Canadian surgical residents from the Royal College of Physicians and Surgeons of Canada. The estimated time to complete the survey was about 15–20 minutes. Most of the questions were multiple choice, but some were short answer. The name and any other identifiers of the participants were unknown for confidentiality purposes. Two reminder emails were sent out to the surgical residents. On completion of the survey, we retrieved the data from the Survey Monkey website. The McMaster University Research Ethics Board approved the conduct of this survey.
Demographic characteristics including sex, marital status, place of medical school graduation and year of residency were collected. Categorical variables were reported as percentages and were compared using the χ2 test. No a priori group comparisons or any hypothesis testing was planned. Post hoc between-group comparisons of Likert scale questions were performed using the Mann–Whitney U and Kruskal–Wallis tests. We set a conservative threshold of p < 0.005 for statistical significance for multiple comparison adjustment. We used SPSS statistical software version 17.0 for statistical analysis.
Results
Survey respondents
This survey was distributed to 600 surgical residents in Canada and was completed by 169 residents (97 [57%] men and 72 [43%] women) for a 28% response rate. The mean age was 29.5 (standard deviation [SD] 3.8) years, and 139 (83%) respondents were graduates of Canadian medical schools whereas 29 (17%) were graduates of foreign medical schools. Table 1 summarizes demographic information relating to the specialties and years of residency of survey respondents.
Demographic characteristics of the survey respondents
Stress-related questions
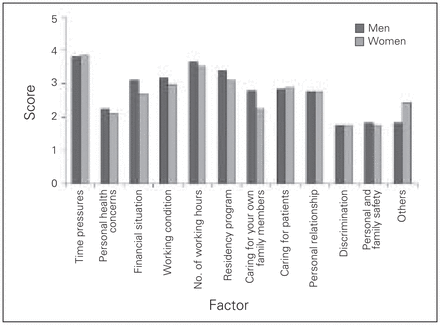
Of the responding residents, 78% reported that most days in their lives were somewhat stressful to extremely stressful, and 87% reported that most days of the past year of their residency were somewhat stressful to extremely stressful. Details on the factors contributing to stress (rated on a 5-point Likert scale, with 1 being not at all stressful and 5 being highly stressful) are shown in Figure 1, and the percentages of residents who rated the factors as highly stressful are shown in Table 2.
Average score of how much the various factors contributed to the stress of male and female surgical residents. The score was assigned on a scale of 1 to 5, with 1 being not at all stressful and 5 being highly stressful.
The percentage of residents who rated various factors as highly stressful
Time pressures were reported to be somewhat stressful to highly stressful by 90% of participants. Other sources of stress that were reported as somewhat stressful to highly stressful included number of working hours (83%), residency program (73%), working conditions (70%), caring for patients (63%) and financial situation (55%).
When asked about their ability to handle unexpected situations, 42% rated their ability as very good and 8% rated it as fair.
The stress attributable to specific components of the residency programs was rated by the residents (on a 5-point Likert scale, witih 1 being not at all stressful and 5 being highly stressful). Those rated as highly stressful are shown in Table 3. Insufficient sleep and call frequency were the components of residency programs that were most commonly rated as highly stressful (31%).
The percentage of residents who rated various aspects of the residency program as highly stressful
Residents were asked to rate their coping mechanisms on a scale varying from often to never. The frequency of the coping mechanisms is outlined in Table 4. Very few residents reported using unhealthy coping mechanisms, such as alcohol consumption, smoking or drug use. Most respondents reported positive thinking or engaging in enjoyable activities as their most commonly used coping mechanisms.
The percentage of residents who reported using various coping mechanisms often
Health-related questions
Respondents answered health-related questions as follows:
88% were nonsmokers;
38% drank 1–3 alcoholic beverages per week when on call;
46% reported an average of 2–3 hours of sleep when on call;
39% reported an average of 6 hours of sleep when not on call;
53% exercised 1–4 hours per week;
66% lost weight during their residency;
24% reported getting annual checkups from their physicians, of whom 71% were women and 29% were men;
54% reported annual checkups from their dentists;
22% reported having mental or emotional problems during their residency;
39% rated their general health as very good;
41% rated their mental health as very good;
37% reported intense anxiety or depression during their residency;
3% had a mental health problem diagnosed during their residency;
9% had a physical problem that was found by a physician to be caused by high levels of stress;
92% reported that they did not notice high levels of stress in their fellow residents; and
49% believed their stress levels would decrease after graduation.
Results of subgroup analyses
Of the people who reported having mental or emotional problems during residency (12 men, 22 women), women were more likely to seek help (18 women v. 5 men; p = 0.017). In addition, women were more likely to get annual checkups by their physician (27 of 68 women v. 11 of 87 men; p < 0.001). Women consulted others, slept more than usual and ate more or less than usual to cope with their stress than men.
Of the people who reported feelings of intense anxiety, depression or panic during their residency, 74% were in postgraduate year (PGY)-3 or above (p = 0.005). Of those who reported mental or emotional problems during their residency, 65% were women and 35.0% were men (p = 0.006), and women were more likely to seek help (p = 0.026). Men were significantly more stressed than women by financial situations (p = 0.036). Of the 66% of residents who reported weight changes during their residency, 67% were in PGY-3 or above (p = 0.010). The only significant difference between junior (PGY-1 and 2) and senior surgical residents (PGY-3 or above) in terms of their coping mechanisms to deal with stress was that senior residents were engaged in more enjoyable activates than junior residents (p = 0.009). Finally, graduates of foreign medical schools reported significantly more stress related to working conditions (p < 0.001), residency program (p = 0.002), caring for family members (p = 0.006), discrimination (p < 0.001) and personal and family safety (p = 0.001) than Canadian medical graduates. Graduates of foreign medical schools more often consulted others (p = 0.036) and smoked cigarettes (p < 0.001) than Canadian graduates as coping mechanism for stress, whereas Canadian graduates more often consumed alcohol (p = 0.004) and exercised (p = 0.001) to cope with their stress.
Discussion
Careers in medicine, particularly the intense years of residency, have been known to be stressful for quite some time.11,12 Although reasonable levels of stress may not have a negative impact on the successful training of medical or surgical specialists, excessive levels of stress might be harmful. In the present study, we assessed the stress of surgical residents across Canada by conducting a survey. This study is unique as, to our knowledge, there are no previous studies solely focused on the stress of surgical residents. As a nationwide sampling was undertaken, our study may have applicability across a wide range of surgical residencies. We also considered the effect of sex and other factors on stress reporting.
How do you define stress? Most would agree that stress is ever present in the lives of surgeons. The ability to react, respond and cope with a set of particular stressors determines success in one’s career. Some individuals may react or deal with stress in a positive manner, hence leading to good outcomes. Over time, the ability to deal with what one considers to be a stressful situation successfully then changes what one finds stressful. However, others who respond in a maladaptive pattern that causes a less than optimal outcome will find that particular circumstances remain stressful in the future. This makes it difficult to nail down an exact definition of stress for surgical residents. Certainly, this line of reasoning also allows us to consider that whereas junior residents may find a particular situation stressful, that same situation may no longer cause stress once they have gained experience and become senior residents. Our study examines how residents cope with stress and which mechanisms they choose to relieve the stress. Hence, one must be cognizant that not only is the definition of stress fluid, but also that responses to stress shift as different techniques and adaptations are subject to the process of trial and error. Dictionary definitions broadly consider stress to be a physical, mental or emotional strain or tension, or a situation, occurrence or factor causing strain. Our study allows for the identification of more residency-specific examples of both of these definitions.
For both sexes, we found that time pressure and the number of working hours were the most highly rated contributors to stress during residency. Also, when asked to rate specific components of the residency program in relation to their stress, the factors rated as highly stressful by most respondents were insufficient sleep and frequent call (Table 3). We found no differences between men and women in the number of hours slept. On average, women reported 2.32 hours of sleep on nights when they were on call and men reported 2.59 hours of sleep when on call. Hours slept when off call were similar between men and women, with men reporting 6.55 hours of sleep and women reporting 6.57 hours.
Previous research has concluded that sleep deprivation can affect optimum quality of care for patients.13 Sleep deprivation leads to increased levels of stress and illness. It has been reported that sleep deprivation of residents can be harmful to the patients they care for as well as the residents themselves, and it has also been suggested that overworking of residents may interfere with the moral growth and advancement that is required for the job.13 These considerations are well known, and work hour restrictions and home after call policies are now a focus in all residency programs.
Our survey revealed that financial issues were a cause of stress to 15% of residents. It has previously been reported that financial factors can disrupt the training of medical residents.1 It is important for directors of surgical programs to note this finding as a potential factor in program disruption that could possibly be averted with early intervention. An interesting finding was that men reported more stress related to their financial situations than women, and the difference between men and women requires more study.
Our survey also asked about the methods of coping mechanisms used by surgical residents for reducing stress. We found that the most common coping mechanism was staying optimistic, followed by engaging in enjoyable activities. The least frequent coping mechanism reported was turning to drugs and medication for reducing stress levels. In previous research, it has been reported that the most popular coping mechanisms are consulting others (such as family members) about problems, staying optimistic and adapting to the stressor.14 Certainly, staying optimistic can be accomplished in different ways; our study did not have the capacity to delve into the exact mental and emotional strategies used by residents to stay optimistic. Details of such internal conversations would be a fascinating topic for future study. Exercise was also one of the highly rated coping strategies for fighting stress. Exercise is known to decrease stress levels by causing the body to increase the release of hormones that combat the symptoms of stress and enhance positive mood.15 The least frequent coping strategy reported by Rudner14 was use of drugs and alcohol, which is consistent with our findings.
Some of the questions in our survey served to demonstrate the residents’ health levels. About one-quarter of residents reported annual checkups from their physicians, and of these respondents, 71% were women and 29% were men. This suggests that female residents may be more concerned with their health or more likely to attend annual physical examinations than male residents. Most of the residents who reported mental or emotional problems during residency were women. This may have been the reason that women were more likely to get annual checkups, but it is also possible that men were less likely to divulge mental or emotional illnesses, even on a confidential survey. Differences between male and female residents have been noted before.1,16 Other studies have shown that female residents were more likely than male residents to experience symptoms related to mental problems, such as depression.1 Furthermore, a recent study on general surgery residents in the United States found that the residents’ attitudes, experiences and expectations regarding training varied by sex and year of program.16
Of the residents who reported weight changes during their residency, 67% were in PGY-3 or above. In previous research, it has been noted that increased levels of stress can be correlated with weight changes.17 Since residents in PGY-3 or above were more likely to experience weight changes, it may be that they experience greater levels of stress in their residency program. An increase in time pressures and number of working hours can be the cause of higher levels of stress and less time for physical activity among more senior residents. In addition, those in the senior years of training are closer to final examinations and may experience stress related to studying and skill acquisition.
The balance between stress and coping mechanisms is important. Although stress may be reported and identified, the ability to cope with stress will determine mental and physical health outcomes. Even though many residents reported mental and physical symptoms during their residency program, 39% reported their general health as very good and 41% rated their mental health as very good. When asked if they had any mental or physical health problems diagnosed during their residency, only 3% reported receiving a diagnosis of a mental health disorder and only 9% reported receiving a diagnosis of a physical problem that was found by their physician to be due to high levels of stress. Tyssen and colleagues18 reported that job stress was correlated with mental health problems among residents and young doctors. The high stress levels of young doctors was found to be due to meeting others’ high expectations as well as anxiety about lack of skills and training while caring for patients.18 Our study found time pressures and the number of working hours to be the main contributors to the residents’ high stress levels. This shows that contributors to residents’ high stress levels are multifactorial and include mental and physical health problems. Training programs may benefit from addressing sources of stress among trainees and reinforcing healthy coping mechanisms.
Almost half of the participants believed that their stress levels would decrease once their program was completed. However, Tyssen and colleagues18 reported that young doctors also experience high stress levels after graduation owing to perceived lack of skills. This was also found to lead to mental health problems. Interestingly, 92% of residents reported that they did not notice high levels of stress in their fellow residents. This may be because residents attempt to hide their stress or that they are simply too busy to notice stress among their colleagues.
Graduates of foreign medical schools reported significantly more stress related to working conditions, residency program, caring for family members, discrimination and personal and family safety than Canadian medical school graduates. Perhaps this is because of their lack of familiarity with the Canadian residency training system. The coping strategies od foreign graduates were also somewhat different from those of Canadian graduates.
It has been noted that anesthesiologists do not experience high levels of stress during their residency program19 and has otherwise been suggested that there are no significant differences in the levels of stress experienced by residents in different specialties.20 However, when evaluating the specific stressors of residents across various specialties, including anesthesiology,19 obstetrics and gynecology,21 emergency medicine,22 and surgery (present study), factors causing resident stress are unique to each specialty. This observation illustrates the importance of studies such as these to identify stressors unique to a particular specialty and inform the development of stress management programs built around the needs of a specific group of residents.
For comparison, in future studies, we recommend a standardized and validated stress survey to be administered among 6 populations: surgical specialists, medical specialists, surgical residents, medical residents and skilled (i.e., people in professions that require a certain level of education and training) and nonskilled general population.
Limitations
Finally, it is worthwhile discussing the limitations of this study. After the invitation of all surgical residents across Canada and subsequent reminders to participate in our survey, our response rate was 28%. Although this response rate might be an acceptable standard for survey response, our sample may still have been too small given the breadth of trainees; therefore, the generalizability of our findings to a Canadian population of surgical residents may be limited. Despite our efforts to encourage participation from all disciplines, nearly 80% of respondents were enrolled in general surgery programs; therefore, the findings might be more generalizable to general surgery residents than to those in other disciplines. However, we feel that the response rate to our survey does not limit our ability to draw conclusions from our data. The survey included questions and topics commonly associated with stress during residency. These questions were derived from analysis of another established survey,9 but we found it useful to add new questions, which we thought would be important in assessing the specific causes of stress levels in surgical residents. We felt that these were not adequately covered by previously established and generalized surveys, and thus these surveys were not used. Another limitation of our survey was the lack of a comparison group. It would have been useful to compare the stress levels of surgical residents to those of other highly motivated trainees to put our findings in perspective. However, the findings from our survey would still help to identify specific issues that could be addressed in the future planning of surgical education programs and in designing a more comprehensive survey with a comparison group. Finally, we used a self-assessment stress questionnaire, which may have been prone to recall bias and overestimation of stress levels.
Conclusion
Overall, our results suggest that surgical residents may experience high stress levels as a result of the change brought about by the requirements of their residency programs. The factors that most influenced stress levels were time pressures and working hours. Based on the results of our survey, these 2 factors need to be of primary concern to those in charge of coordinating surgical residency programs. Much effort has already been applied to address the primary stressors of residents, including implementing many support systems, decreasing working hours over time and altering rules regarding on-call shifts. However, it still appears as if surgical residents perceive their overall stress levels as high. Program administrators may consider maximizing efforts to assist residents with positive coping mechanisms, such as social activities and physical fitness. Finally, training programs with residents from foreign medical schools may wish to consider the unique stressors reported in this group.
Footnotes
Presented at the annual meeting of the Canadian Association of General Surgeons, Sept. 10-13, 2009, in Victoria, BC.
Competing interests: None declared.
Contributors: N. Aminazadeh, F. Farrokhyar, A. Naeeni, M. Naeeni, S. Reid and K. Kahnamoui designed the study. N. Aminazadeh, A. Naeeni, M. Naeeni and A. Kashfi acquired the data. N. Aminazadeh, A. Naeeni, M. Naeeni, S. Reid and K. Kahnamoui wrote the article. All authors analyzed the data, reviewed the article and approved its publication.
- Accepted May 24, 2011.