Tumefactive demyelinating lesion (TDL) is defined as a solitary de-myelinating lesion greater than 2 cm. Mass effect and contrast enhancement on neuroimaging make it difficult to distinguish this type of lesion from high-grade gliomas.1,2 Multiple sclerosis (MS) accounts for most cases of TDL.3 Even in patients with established MS, an atypical manifestation of a large lesion can suggest concurrent neoplasm, because the clinical manifestations are often similar.1,4 When examined on magnetic resonance imaging (MRI) scans, TDLs have ill-defined borders, mass effect, perilesional edema, central necrosis, cystic degeneration, contrast enhancement and variable involvement of grey matter.4 Unless specifically requested, pathological examination does not routinely include luxol fast blue staining, which can be used to detect demyelination. The presence of hypercellularity, atypical reactive astrocytes and mitotic figures can lead to an incorrect diagnosis of glial neoplasm.4 We present 3 cases of tumefactive demyelinating lesions that were clinically and radiologically challenging to distinguish from high-grade neoplasm.
Case 1
Patient 1 was a 50-year-old woman who presented with a 3-day history of headaches and generalized tonic-clonic seizures. Physical examination did not reveal a focal point of her seizure. A computed tomography (CT) scan of the patient’s head revealed a large right frontal ring enhancing lesion with central necrosis, peritumoral edema and a mild midline shift. This presentation was most consistent with a malignant brain tumour. The patient underwent surgery for resection of the lesion. Postoperative pathology indicated an extensive inflammatory cell reaction, both acute and chronic, with focal necrosis predominantly through the white matter areas. Luxol fast blue staining showed an absence of myelin. A diagnosis of acute disseminated encephalomyelitis was made.
Case 2
Patient 2 was a 43-year-old woman who presented with a 4-day history of left facial droop and left arm weakness that was more pronounced distally. Physical examination confirmed these symptoms, including gait ataxia. Her medical history included a diagnosis of MS 3 years ago when she had transverse myelitis. Magnetic resonance images obtained 3 years earlier showed transverse myelitis from T4 to T7 with unremarkable intracranial pathology. A new CT scan of her head showed a large solitary right frontal hypodense white-matter lesion. It was unclear whether this represented a tumefactive multiple sclerotic lesion or a low-grade cystic neoplasm. The patient underwent a stereotactic biopsy to determine the nature of the lesion. The diagnosis of MS was confirmed by biopsy (Appendix 1, available at www.cma.ca/cjs).
Case 3
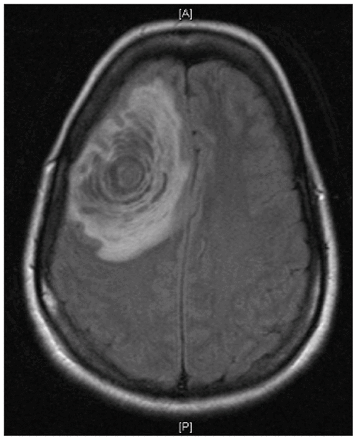
Patient 3 was a previously healthy 35-year-old woman who presented with new-onset generalized tonic-clonic seizures and headaches. Magnetic resonance imaging scans showed a large right frontal mass with surrounding edema and a mild midline shift (Fig. 1). The patient underwent a diagnostic stereotactic brain biopsy. Low-grade glioma and reactive gliosis were among the likely differential diagnoses. Permanent section showed a demyelinating lesion. In retrospect, the appearance of the mass was similar to that seen in Balo concentric sclerosis in which there are large regions of alternating zones of demyelinated and myelinated white matter.
A T1-weighted magnetic resonance imaging scan showed a right frontal lesion with midline shift.
Discussion
There are certain features seen by MRI and histopathology analysis that can help diagnose TDL. A central dilated vascular structure within the lesion on T2-echoplanar images from MRI perfusion studies is commonly seen in TDL.5 This structure is believed to represent a vein draining toward the distended subependymal veins.5 Several reports that used MRI have shown decreased perfusion within TDL lesions compared with that found in high-grade neoplasms.5 Corticosteroid therapy has been shown to reduce the size of TDL lesions on follow-up imaging.1,3
Magnetic resonance spectroscopy can also help identify these lesions. Glial cell tumours produce excess choline with suppressed levels of N-acetylaspartate (NAA) relative to creatine.4 There is also a prominent lactate doublet.4 In contrast to neoplasia, chronic demyelinating lesions show normalization of initial increase in lipid and lactate peaks within 3–4 weeks followed by persistent marked reduction of NAA levels.
The histopathologic characteristics of demyelinating lesions include the preservation of axons as shown by the presence of neurofilaments, the loss of myelin as shown by negative luxol fast blue staining, the presence of macrophages as shown by the presence of CD-68, and astrocytic proliferation as shown by the presence of glial fibrillary acidic protein.2 Standard tumour histopathological protocols do not include staining with Luxol fast blue, which is used to detect myelination. Therefore, it is important for the clinician to have a high index of suspicion for a demyelinating lesion and relay this to the neuropathologist.
In conclusion, the diagnosis of TDL often leads to surgical biopsy, which has a high risk of morbidity. It is important to recognize the subtle differences in TDL to avoid a brain biopsy and, more importantly, erroneous resection of viable brain tissue.
Footnotes
Competing interests: None declared.
Contributors: Drs. Paulseth and Jha designed the study and reviewed the article. Drs. Fallah, Banglawala and Ebrahim acquired the data and wrote the article. All authors approved the article’s publication.
- Accepted November 7, 2008.