Abstract
Objective: Fewer orthopedic surgery trainees are choosing careers in trauma. The impact of stressors on health-related quality of life has not been evaluated among orthopedic surgical residents. The current study aimed to determine predictors of unsatisfactory resident quality of life during trauma rotations.
Method: This was a prospective observational study in which we chose orthopedic trauma rotations within 2 training programs at 3 level 1 trauma centres. A sample of 15 orthopedic surgery residents participated in the study. The main outcome measure was the 36-Item Short-Form Health Survey taken at baseline, 2 and 6 months into the rotation. Residents ranked level of stress for 15 work-related and 13 individual problems on 5-point Likert scales.
Results: The residents ranged from training years 1 through 5, and their mean age was 31 (standard deviation [SD] 2.8) years. Fear of error decreased at 6 months, compared with baseline (p = 0.007). Lack of time for family decreased as a problem at 2 and 6 months, compared with baseline (p = 0.025). Baseline Physical Component Summary scores were above population norms (p = 0.007). At 2 months, scores for the concept role limitations (physical) decreased significantly (p = 0.019), compared with the baseline. Mean Physical Component Summary scores declined from 57.59 (SD 3.51) at baseline to 53.68 (SD 6.50) at 2 months (p = 0.015) and 53.94 (SD 3.52) at 6 months (p = 0.008). At 2 months, mean general health scores significantly decreased, compared with baseline (p = 0.022). Social functioning scores at 6 months were decreased from population norms (p = 0.02). More resident social time was spent with medical people exclusively at 6 months, compared with baseline (p < 0.02).
Conclusion: Trauma rotations affect residents’ emotional well-being. Training programs should equip residents with coping strategies to improve quality of life during trauma rotations.
Quality of life and general well-being during orthopedic surgical residency is a topic of current interest, given evolving guidelines for maximum allowable work hours weekly.1–4 The Accreditation Council for Graduate Medical Education (ACGME) requires all programs to limit resident work hours to 80 hours weekly, with some programs allotted an extra 10% for specific educational purposes.2 Although physician fatigue has taken centre stage as the primary motivation behind this movement, the effect of these rules on the continuity of care for hospitalized patients needs to be critically analyzed from the perspectives of patients, physicians and the health care system.5
Damestoy and colleagues6 identified 3 main types of stressors in resident quality of life studies: work-related stressors such as long working hours, heavy workloads, time pressure and low self-confidence; personal stressors such as a lack of time for oneself and one’s family; and economic stressors due to the financial burden of training. In a study by Lewittes and colleagues,7 27% of nearly 2000 residents surveyed felt that they were “often” or “nearly always” bothered by the feeling that their workload was too heavy and could not be finished in a usual working day. Other studies have pointed out the link between excessive work demands, fatigue and quality of care.8–10 Residents’ obligations to provide care while suffering from fatigue may lead them to tolerate lower standards of patient care than they would if they were well rested.7 As well, fears of inadequate performance as a physician during residency may cause residents to ignore their personal well-being as they focus on their professional development.11 Time pressures and sleep deprivation constitute the major stressors adversely affecting the ability of residents to learn and, at times, the quality of care they provide.11–15
It is our belief that orthopedic surgery residents’ quality of life is subject to adverse changes during a busy trauma rotation. Using this as our hypothesis, we chose the trauma rotation for the setting of our study. Trauma rotations of 3 or 6 months’ duration are mandatory requirements of all orthopedic training programs in North America. The impact of stressors on health-related quality of life and well-being has not been thoroughly evaluated among orthopedic surgical residents on busy trauma rotations. The current study aimed to determine those modifiable factors and stressors that predict residents’ quality of life. Further, information from this study might encourage trauma curriculum reform to renew enthusiasm for careers in trauma among orthopedic surgical trainees.
Methods
We conducted a prospective, multicentre, observational study of quality of life during standardized orthopedic trauma rotations across 3 level 1 trauma centres.
Eligibility criteria
Eligible trainees included orthopedic surgery residents rotating on an orthopedic trauma service during our study period. A total of 15 orthopedic surgery residents at 3 level 1 trauma hospitals (part of 2 orthopedic training programs) were enrolled in this study. Ten enrollees were senior residents (fourth and fifth year), and 5 enrollees were junior residents (first to third year).
Trauma rotations
Trauma rotations were at 3 level 1 trauma centres. The residents were on call an average of 1 in 4 days. The typical workday when not on call was from 0600 to 1800. The typical work week was 80 hours on average. Patient load varied depending on the service.
Baseline evaluation
Residents were approached before the start of their trauma rotation and asked to provide baseline information. This information included demographic characteristics of age, sex, year of residency, marital status and number of children. We measured overall stress, stress of being a resident and stress of combining a personal and professional life (from Rudner and colleagues11) before and during the rotation, using a 5-point Likert scale: 0 = little or no stress, 1 = minimal stress, 2 = moderate stress, 3 = high stress, 4 = excessive stress.
Assessment of quality of life
We assessed quality of life and general well-being with the 36-Item Short-Form Health Survey (SF-36),16 a stress questionnaire11 and a list of individual and work-related problems experienced by residents.17,18
On approval by the institutions’ ethics review boards, survey questionnaires were given at baseline evaluation and at months 2 and 6 of the trauma rotation. The first survey served as a baseline, which we compared with subsequent surveys. Surveys required 20 minutes to complete. One research assistant analyzed all the surveys. Each resident was given a numeric code, and all identifiers were removed after analysis. Faculty and staff had no access to the surveys, and all results were kept anonymous and confidential.
The SF-36 includes 1 multi-item scale measuring each of the following 8 health concepts:
Physical functioning assesses limitations of normal physical activities and is designed to estimate the severity of limitation (10 questions).
Role limitations (physical) assesses functional limitations at work that are caused by physical health problems (4 questions).
Bodily pain assesses both the severity of pain and the extent to which it interferes with normal activities (2 questions).
Social functioning assesses the quantity and quality of interactions with others, extending measurement beyond the exclusively physical and mental health concepts (2 questions).
Mental health/emotional well-being assesses the 4 major mental health dimensions of anxiety, depression, loss of behavioural or emotional control and psychological well-being (5 questions).
Role limitations (emotional) assesses functional limitations at work that are caused by emotional problems, but this concept excludes limitations caused by physical problems (3 questions).
Vitality/energy assesses a subjective feeling of well-being, including energy and fatigue (4 questions).
General health assesses physical health status and has been documented to be a good predictor of health care expenditures (5 questions).
We also derived Physical Component (physical functioning, role physical, bodily pain and general health perceptions) and Mental Component (vitality, social functioning, mental health and role emotional) Summary scores.19
In addition, we asked residents to rank 15 work-related stressors11 on a 5-point Likert scale ranging from 0 (not a problem) to 4 (extreme problem). The 15 work-related stressors were as follows: learning everything, feeling rushed, being on call, self-doubt, fear of error, no time for needy patients, frustration, death of patient, conflict between patients, program problems, status as a resident, problems with other specialties, sleep problems, faculty problems and resident problems.
An inventory developed by Nelson and Harvey18 at the University of Minnesota, and a modified version developed by Smith, Andrasik and Quinn (revised scale),17 both having over 100 questions, yielded the top 10 individual problems identified by residents. Our surveys included these 10 problems as well as an additional 3 that we believed to be highly applicable to our study. Again, residents ranked the 13 individual problems on a 5-point Likert scale ranging from 0 (not a problem) to 4 (extreme problem). The 13 individual problems were as follows: not enough time for self, not enough leisure time, not enough time for physical activities (sports, exercise), not enough time to spend with spouse/friends/relatives, problems created by inflexible work hours, not enough time for study, not confident enough about self in medicine, reservations about being a doctor, not enough money, sexual drive decreased since beginning residency, not sure about choice of residency, feeling unfairly treated by program staff, and residents or medical people the only people seen socially.
Statistical analysis
For each time period surveyed, the number of residents responding varied slightly. As a result, we used paired t tests to detect changes in the same group of residents throughout the rotations. Junior residents had shorter rotations and thus were not included in the 6-month follow-up. We compared each of the SF-36 domains with the mean normative SF-36 Canadian population domain scores20 for people aged 25–34 years. Statistical significance was established with Student’s t test to compare the means. We corrected our p values for multiple comparisons and conducted such tests to explore the specific points at which differences might have been important (or statistically significant). Because we carried out numerous t tests, we set statistical significance at a p value of less than 0.03 to avoid significance due to chance alone.
Results
In total, 15 residents (13 men and 2 women) from training years 1 through 5 participated in the study. Their mean age was 31 (standard deviation [SD] 2.8) years. Of the residents, 53.3% were married or in a common-law relationship, 46.7% were single, and 33.3% had children.
The overall stress level was ranked by residents at baseline and at 2 and 6 months. According to paired t tests, there were no statistical differences in stress levels at baseline, 2 and 6 months. At 6 months, fear of error had decreased significantly from baseline (p = 0.007) (Table 1).
Changes from baseline in residentsí ranking of work-related stressors
Throughout the rotation, there were no statistically significant changes in residents’ perception of time for themselves. Lack of time for spouse, family and friends decreased as a problem among residents at 2 and 6 months, compared with baseline (p = 0.025) (Table 2). In other words, residents reported having more time to spend with their spouse, family and friends. At 6 months, more resident social time was spent with medical people exclusively, compared with baseline (p = 0.018).
Changes from baseline in residents’ ranking of individual problems
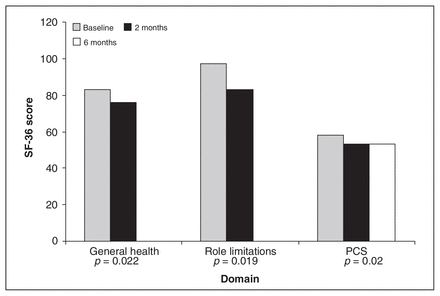
For the SF-36, mean baseline role limitation (physical) scores of residents were 97.32 (SD 5.32). At 2 months, these scores significantly decreased to 83.04 (SD 24.2) (p = 0.019) when compared with the baseline score (Table 3, Fig. 1). There were no statistically significant differences among residents’ scores at baseline, 2 and 6 months when compared with the mean Canadian population norms for role limitation.
SF-36 domains with significant changes. PCS = Physical Component Summary score; SF-36 = 36-Item Short-Form Health Survey.
SF-36 scores at baseline compared with 2- and 6-month scores
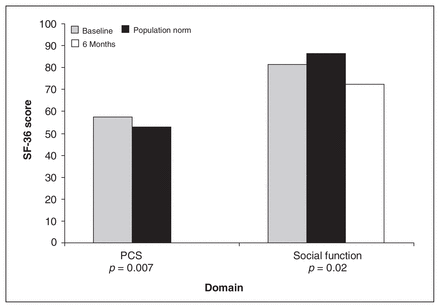
Residents’ mean scores at baseline for bodily pain, vitality, mental health, physical and social functioning and role limitations (emotional) did not change significantly over the rotation. At 6 months, however, the residents’ mean social functioning scores had decreased significantly from the Canadian norms (mean 86.3, SD 20.3; p = 0.02) (Fig. 2).
Significant change in SF-36 scores compared with population norms. PCS = Physical Component Summary; SF-36 = 36-Item Short-Form Health Survey.
At baseline, mean scores for general health were 83.14 (SD 13.10). At 2 months, this score had decreased significantly to 76.64 (SD 14.07) (p = 0.022 v. baseline) (Table 3, Fig. 1). The mean 6-month general health score (75.78, SD 16.14) was also lower than baseline scores, but this was not statistically significant (p = 0.037). No statistically significant differences were found for residents’ mean scores at baseline, 2 and 6 months when compared with the mean Canadian population norms for general health.
Physical Component Summary (PCS) scores take into account scores for physical functioning, role (physical), bodily pain and general health. PCS scores declined from 58.13 (SD 2.93) at baseline to 53.68 (SD 6.50) at 2 months (p = 0.015), and 53.94 (SD 3.52) at 6 months (p = 0.008) (Table 3, Fig. 1). The baseline mean PCS score for the residents was significantly higher (p = 0.007) than the mean Canadian population PCS score (53.0, SD 7.2) (Fig. 2). No statistically significant differences were found among residents’ mean scores at 2 and 6 months when compared with the mean Canadian population norms for the PCS.
The Mental Component Summary (MCS) score includes scores for vitality, social functioning, mental health and role (emotional). The mean MCS score for residents did not change over time, and there were no statistically significant differences between residents’ mean scores at baseline, 2 and 6 months and the mean Canadian population norms for the MCS.
Discussion
There is no question that surgical residency programs impose an added stress on quality of life and well-being, mainly owing to the high volume of work-related experience that is required to train a successful surgeon. In various residency programs, including the surgical specialties, Perry and Osborne21 studied the following characteristics addressed before and after residency: eating habits, hours of sleep, recreational time, exercise and missed significant events. They found that residents perceived significant changes in many areas of health and wellness during residency training. In a survey of residents throughout their first year, Bruce and colleagues22 found that interns experienced increased levels of stress and ill health in the middle of the year as compared with the start and end of the year.
In evaluating the trainees’ quality of life during a busy trauma rotation, we used several modalities. The SF-36 general quality of life validated survey has not, to our knowledge, been used with surgical residents before this study. The SF-36 has been validated across several disease states as well as “healthy norms.” We simply applied this questionnaire to a population otherwise perceived as healthy and normal. This tool allowed us to compare the general health and emotional well-being of residents with age-matched population norms. Our findings suggest that differences do occur in this population and deserve future exploration in larger data sets.
The SF-36 showed that resident scores declined in 2 out of 8 health domains and in the PCS. General health scores declined significantly at 2 months, compared with baseline scores. PCS scores declined from mean 57.59 (SD 3.51) at baseline to mean 53.68 (SD 6.50) at 2 months (p = 0.015), and mean 53.94 (SD 3.52) at 6 months (p = 0.008). At 6 months, residents’ social functioning scores had decreased significantly from the Canadian norms (mean 86.3, SD 20.3; p = 0.02). It has been shown that a 5-point difference between groups or a 5-point change over time is considered clinically relevant.23 Given that the baseline physical function and PCS scores were above the Canadian population’s mean, the decrease in the PCS score at 2 and 6 months is indicative of a decline in the residents’ general health through the rotation.
Role limitations (physical) assess the individual’s functional limitations at work that are caused by physical health problems, and at 2 months, resident scores in this domain decreased from baseline (p = 0.019). It is thus imperative for residents to be in good physical condition before starting their trauma rotation, as some decline is to be expected.
Fear of error decreased among residents at 6 months when compared with baseline (p = 0.007). It is evident from our study that, as the residents progressed in their rotation, their knowledge base and technical experience increased. Reduced fear of error was the most important stress-reducing factor modified during the rotation. Lack of time for spouse, family and friends decreased as a problem at 2 and 6 months when compared with baseline (p = 0.025). Therefore, issues that initially were significantly problematic were diminished or nonexistent as the rotation went on. This confirms that coping strategies, when placed early in the training program, can be beneficial and thus decrease the level of anxiety and stress among residents early in their rotation. Rudner’s recommendations, 11 based on survey results, include developing support groups, providing advisors and assigning a senior resident to each beginning first-year resident. In our training program, each staff surgeon mentors a single resident, and regular one-on-one meetings take place. We believe this is also highly valuable for career counselling and helps to support residents during difficult times.
A recent study by Sargent and colleagues24 found considerable burnout in orthopedic surgery residents, with high emotional exhaustion and depersonalization. Protective factors included being a parent, having a physician father, spending time with spouse and discussing concerns with colleagues, friends and family. Schwartz and colleagues25 found that “high-quality” teaching rounds and a night-float system were among the suggestions made by the residents to lessen stress. Further, to cope with stress, the residents reported that they talked to others, tried to see humour in the situation or slept. This was illustrated in our study, where more resident social time was spent exclusively with medical people at 6 months compared with baseline.
We realize that this study is limited by its small sample size. We also realize that this study is specific to orthopedic surgery residents, our target group. We acknowledge the limitations of this study specifically related to sample size. Whether our findings are real will only be revealed by evaluations conducted by other investigators in a similar subset of people. Ultimately, increasing the sample should improve the precision of our estimates and also provide improved generalizability. We do believe, however, that similar studies within surgical and nonsurgical subspecialties should take place in the near future. The importance of such studies for improving the surgical education and quality of life of residents cannot be underestimated.
Trauma rotations affect residents’ emotional well-being. Training programs should equip residents with coping strategies to improve quality of life during trauma rotations. Mentorship programs wherein residents meet their mentors regularly have been implemented in some programs, including ours. Further, stress management training should be implemented and has been shown to be beneficial if frequent training is provided; otherwise, its benefits are not long-lasting.26 Stress management programs may also be beneficial to residents before they start trauma rotations. Improving the quality of life for orthopedic residents in a trauma rotation should begin early in their training with support programs implemented by residency programs.
Footnotes
This paper was presented at the 11th Meeting of the Combined Orthopaedic Associations in Sydney, Australia, October 24–9, 2004, and at the Annual Meeting of the American Academy of Orthopaedic Surgeons (AAOS) in Chicago, Ill., March 22–6, 2006.
Competing interests: None declared.
Contributors: Drs. Zahrai, Bhandari, Rennie, Stephen and Schemitsch designed the study. Drs. Zahrai, Varma, Kreder and McKee acquired the data, which Drs. Zahrai, Waddell and Schemitsch analyzed. Drs. Zahrai and Bhandari wrote the article. All authors reviewed the article and provided final approval for publication.
- Accepted June 16, 2007.