Abstract
Objective: To determine whether rate-based funding using resource intensity weights (RIWs) adequately represents trauma case costs.
Design: A prospective time-in-motion resource utilization pilot study to assure the effectiveness of the computerized hospital Transition-One data acquisition system, followed by a retrospective observational case costing study. Patient costs with no identifying data were used, and all costs were tabulated as mean cost per group.
Setting: London Health Sciences Centre, London, Ont., a tertiary care “lead” trauma hospital.
Patients: A modified random selection of 4 control case mix groups (CMGs) of surgical patients for the fiscal year 1996–97. The trauma group was selected as a representative resource-intensive CMG. Each patient was assigned to a CMG by Health Records according to the most responsible diagnosis.
Outcome measures: Total case costs were tabulated for each patient then combined for a mean case cost per CMG. The RIW assignments for each patient were combined to create a mean RIW per CMG and mean length of stay per CMG.
Results: There was no statistically significant difference between the control surgical CMGs and the trauma CMG for mean RIW-adjusted length of stay per CMG, but there was a significant difference (p < 0.0001) between the control CMGs and the trauma CMG for RIW-adjusted mean case cost per CMG.
Conclusions: RIWs underrepresent trauma case costs by a factor of 3.5, which could result in underfunding and potential fiscal difficulties for leading trauma hospitals as has occurred in the United States.
Canadian hospitals have traditionally been funded on a “global” basis from their respective ministries of health with adjustments for location of care (teaching or nonteaching, urban or rural) and actual number of cases with a crude overlay for case complexity. When this system of global hospital budgets was established in the 1970s, concerns were raised regarding the fairness of funding for both base budgets and annual increments.1 In 1988, a fairer and more flexible measure of hospital output, analogous to the New York service intensity weights used by American hospitals, was developed and adopted by the Ontario Ministry of Health for that province.2 Resource intensity weights (RIWs) were thus created and were first used in the early 1990s to assess funding of Ontario’s hospitals.3 The premise on which RIWs were created was that hospitals providing comparable inpatient services had similar resource needs and were entitled to comparable funding, although questions have been raised regarding the validity of the assumptions used to create Canadian RIWs.4 Case mix groups (CMGs) were modelled after the American “diagnosis related groups” (DRGs),5 as it had become clear that US-based DRG groupings might not demonstrate statistical homogeneity when used with the Canadian acute-care hospital patient population.2 As this system has become more refined, it has been proposed that in the near future, hospitals be funded on a “cost per case” basis (mean cost per CMG) using a standard funding formula with well-defined adjustment factors (RIWs) for cases that are resource intensive (called rate-based funding).6
Experience gained in the US, when hospital remuneration was tied to the development of DRGs and a form of surrogate RIW measures, demonstrated that many hospitals with significant case volumes of major trauma or other resource-intensive surgical procedures, quickly experienced sizable operating deficits.7 In fact, several trauma centres were forced out of business because of the poor relationship of funding to case volumes, based on DRG assignments.
We hypothesized that although RIWs may control for differences in resource utilization among CMGs when crude length of hospital stay is used as a surrogate measure of costs, they could not accurately control for differences in resource utilization among CMGs when resource utilization is fully costed.
Methods
This study was undertaken at the London Health Sciences Centre (LHSC), an 800-bed teaching hospital affiliated with the University of Western Ontario, London, Ont., between June 1996 and August 1997. The LHSC serves as the “lead” hospital for major trauma in southwestern Ontario, managing over 400 major trauma cases (Injury Severity Score >15)8 annually. Since this study was considered to be a quality improvement one, no informed consent was required, and all case costs were averaged, so that no identifying patient data remained.
The standard methodology for costing studies is a time-in-motion study, in which patients are prospectively followed from the beginning until the end of a given treatment.9 The LHSC utilizes the Transition One (T-1) computerized data acquisition system, by which case costs, productivity and daily resource utilization (divided into each drug, test and indirect cost such as nursing time) can all be ascertained. The limitations of the T-1 system include the omission of drug costs in both the intensive care and emergency wards, as well as indirect costs related to the time spent in the emergency department and the departmental costs of the trauma program. No physician costs were included in this study as these were not accrued by the hospital. In the pilot phase of this study, patients were identified who fell into 2 CMGs (319 who had laparoscopic cholecystectomy and 876 with multiple significant trauma with lower extremity fractures). They were followed from the moment of entry into the hospital until their discharge between June 1996 and September 1996. Trauma patients were recruited into the study by activation of the trauma team as soon as the emergency department was made aware of the patient’s arrival. The patients who underwent cholecystectomy were recruited from the elective operating room booking schedules at LHSC.
The first phase of this costing study involved data collection of all resources used by each patient, including all staff hours, as well as drugs and materials used by the patient, radiologic and diagnostic tests, operating room and intensive care unit time. The patient’s chart was also used to record resources consumed by that patient. The total costs for each patient collected manually were compared to the costs tabulated by the T-1 system, with the purpose of ensuring that T-1 was an accurate tool to use for the eventual costing study. This proved to be the case. A few costs were not captured; they were added for each patient in the next phase of the study. These costs included the drugs consumed in the intensive care unit and the emergency department, the indirect costs of the initial resuscitation and the overhead costs of the trauma program of the LHSC.
The second phase involved selecting a representative major trauma CMG as well as a number of control surgical CMGs. The same trauma CMG (876) was used as in the pilot study. The standard method for selecting the control CMGs would be by random selection; however, because many CMGs have so few patients within a single fiscal year, the control CMGs were selected in a modified random fashion, selecting any CMG for which case costs were available where the number of patients exceeded 50 during fiscal year 1996–97. In this manner 4 control CMGs were selected: CMG 356 (non-traumatic femoral fractures), CMG 579 (nonmalignant major gynecologic procedures), CMG 580 (other major gynecologic procedures) and CMG 581 (procedures for endometriosis). Thus, 1 control CMG represented emergent orthopedic cases and 3 control CMGs were taken from elective abdominal gynecologic surgery cases, primarily owing to limitations in available costing data for CMGs from other surgical specialties. The direct and indirect fixed and variable costs were obtained from the T-1 data system.
The RIWs for each patient were also obtained from the T-1 system. Age, gender, mean case costs, mean length of hospital stay and mean RIW were reported for each CMG. Two multivariate generalized linear models were developed to assess the ability of RIWs to control for differences in resource utilization between CMGs. First, to determine if RIWs controlled for differences in resource utilization, as reflected by the surrogate measure length of hospital stay, we created a multivariate model containing CMG and RIW as main effects and length of stay (LOS) as the outcome. Second, to determine if RIWs controlled for differences in resource utilization, as measured using a fully costed approach, we created a multivariate model containing CMG and RIW as main effects and costs as the outcome. Both models contained CMG and RIW main effects along with a CMG–RIW interaction term. LOS and costs were log-transformed to address questions concerning the assumption of normality. Individual comparisons between CMGs were made using the LSMEANS option within PROC GLM (PC-SAS version 6.1210). All p values reported for direct comparisons between RIW-adjusted CMGs are derived from the LSMEANS option and are Bonferroni corrected to control for multiple comparisons. All analysis was performed using PROC GLM.10
Results
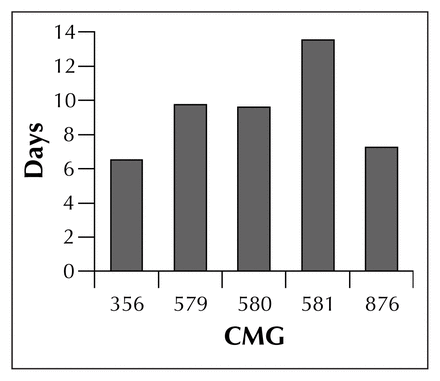
The patients’ demographic data includes the number of patients in each CMG for the fiscal year 1996–97, mean age and gender distribution (Table 1). Total costs, mean RIWs and mean length of hospital stay for each of the CMGs are shown in Table 2. The mean Injury Severity Score for the major trauma patients was 28 (range from 10–57). In the first multivariate model, analysis revealed that CMG, RIW and RIW–CMG were significant independent predictors of LOS (CMG p < 0.0001, RIW p < 0.0001 and CMG– RIW p < 0.0001). Using LSMEANS to investigate RIW-adjusted differences in LOS between CMGs revealed no significant differences between the trauma CMG 876 and any of the control surgical CMGs (Fig. 1).
Resource intensity weight (RIW)-adjusted mean length of stay in days, for each case mix group (CMG). There was no statistically significant difference between the trauma CMG 876 and the control surgical CMGs, using multivariate regression analysis (p = 1.0), indicating that RIW does adjust for length of stay (LOS). There was however, a statistical difference in the mean LOS between control CMG 356 and CMGs 579 and 580 (p = 0.007), showing that the RIW correlation to LOS is near perfect despite minor variations between a few of the control CMGs.
Patient Demographics for Each Case Mix Group (CMG) (a Total of 531 Patients)
Mean Cost, Resource Intensity Weight (RIW) and Length of Stay (LOS) for Each Case Mix Group (CMG)
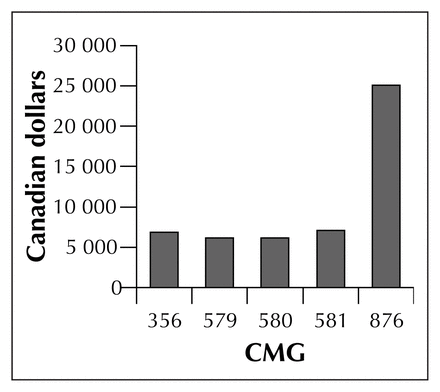
In the second model, multivariate analysis demonstrated that CMG, RIW and CMG–RIW were all significant predictors of costs (CMG p < 0.0001, RIW p < 0.0001 and CMG– RIW p < 0.0001). Using LSMEANS to investigate differences between CMGs we found that the RIW-adjusted costs associated with trauma CMG 876 were significantly higher than nontraumatic femoral fractures (CMG 356) ($25 088 v. $6844, p < 0.0001), significantly higher than nonmalignant major gynecologic procedures (CMG 579) ($25 088 v. $6195, p < 0.0001), significantly higher than other major gynecologic procedures (CMG 580) ($25 088 v. $6144, p < 0.0001) and significantly higher than procedures performed for endometriosis (CMG 581) ($25 088 v. $6170, p < 0.0001). However, there were no significant differences between any of the control groups with respect to RIW-adjusted costs. Complete results of individual comparisons, including costs calculated for each CMG using LSMEANS, are presented in Table 3.
Resource Intensity Weight (RIW)-Adjusted Length of Stay (LOS) and Costs for Each Case Mix Group (CMG)*
Discussion
The usefulness of RIWs is critically dependent on their ability to reflect resource consumption of an average CMG. It has been demonstrated that RIWs very effectively reflect length of hospital stay,11 which to date has been the best surrogate measure of resource consumption.
The standard measurement of resource consumption is case costing.9 This study looked at the RIW-adjusted mean LOS for the trauma and surgical control CMGs, to demonstrate that RIWs do accurately represent LOS and in that regard were well designed. Since the actual formula used by the Ministry of Health for RIW calculation is unavailable, we assumed use of a simple calculation for mean RIW-adjusted costs, based on how RIWs were created,3 and developed our statistical analysis accordingly. As expected, there was no statistical difference between the trauma and the surgical control CMGs (although there was statistical difference between CMG 356 and CMGs 579 and 580, demonstrating some variability in expected mean LOS) (Table 3, Fig. 1). The variability with mean LOS in CMG 356 may represent the current pressure on surgeons to discharge patients with isolated fractures to peripheral hospitals for convalescence sooner, owing to financial disincentives created by the funding system.
If the assumption that LOS is an accurate surrogate measure of cost and resource consumption is a correct one, there should be no difference between the RIW-adjusted mean costs per case. In fact, the RIW-adjusted mean costs per CMG revealed no statistical difference between the surgical control CMGs, but an enormous statistical difference between the trauma CMG and the control CMGs (Table 3, Fig. 2). This study has clearly demonstrated that when comparing the RIW-adjusted mean cost per case for a trauma CMG with a random group of other surgical control CMGs, the mean RIW assigned to the trauma cases underestimates the resource consumption, and thus costs of these cases, by a 3.5-fold difference. This suggests that RIWs are useful in representing case costs of fairly predictable surgical cases but do not accurately reflect cost in resource-intensive unscheduled trauma cases. Trauma case costs have been consistently underestimated in the past because of the high variability in case costs.7 However, it must be remembered that cost outliers are expensive and need to be included in these costing studies. Ignoring these cases could result in disastrous financial consequences for trauma hospitals in a rate-based funded system.
Resource intensity weight (RIW)-adjusted mean cost per case in Canadian dollars, for each case mix group (CMG). There was no statistically significant difference between any of the control surgical CMGs (p = 1.0). There was, however, a statistically significant difference in the RIW-adjusted mean cost per case between the trauma CMG and each of the control CMGs (p < 0.0001). This indicates that RIW assignments seem to adjust for mean case cost in the control surgical CMGs but not in the trauma CMG, which was 3.5-fold higher despite an RIW adjustment.
It is not clear which component of the major trauma cases leads to the high resource consumption. One may speculate that the high cost may be related to the exhaustive search for injuries in multiply injured patients (often including much more frequent use of computed tomography and admission to intensive care units).12 Further studies looking at cost per patient per day between CMGs using costing methods as outlined in the Ontario Case Cost Project may be more useful to elucidate this.13 High costs may also be related to the variability in injury severity, the age among trauma patients14 and the increased rate of early death among trauma patients, which decreases hospital reimbursement by financial disincentive.15 We do not consider that the inclusion of 1 orthopedic and 3 gynecologic CMGs as controls represents any limitation of this study, since there is sufficient similarity between operative procedures in elective abdominal gynecologic and general surgical cases. It represents simply a limitation in the costing data available to us at the time of the study.
The finding that RIWs cannot accurately reflect case costs of resource-intensive CMGs, such as multiple orthopedic trauma, is significant, since the Ontario Ministry of Health has given significant consideration to the sole use of RIWs for future hospital funding in a rate-based manner. The underfunding of such resource-depleting cases could ultimately lead to profound hospital deficits for institutions caring for large volumes of major trauma. The importance of a hospital staying within its global budget cannot be overstated, as the Ministry of Health uses this as an assessment tool for the determination of “efficiency” of a given hospital, and any discrepancy (if negative) is used to determine the extent of potential cutbacks that this hospital could receive for the next fiscal year.6
In 1990, in order to ensure that effective trauma services were available across the province, a number of large teaching hospitals were designated as “lead” trauma hospitals. These hospitals are concerned that the potentially negative financial impact of caring for trauma patients may discourage them from continuing to provide this service. This concern is a legitimate one, given the precedent set by trauma hospitals in the US7 and the fact that Canadian hospital funding is based on the American model and US costing data.16 In the US, over 90 trauma centres have closed in recent years. Subsequent examination of US trauma institutions revealed that 58% of trauma hospitals willing to discuss finances reported that their centres were facing severe financial problems17 and that most of these trauma hospitals were considering an additional charge for the care of trauma patients, since the cost to the hospital of caring for such a patient clearly exceeds the reimbursement. Many of these trauma patients have no private insurance, which results in these hospitals depending on government funding, not unlike Canada’s health funding system.
It is the current philosophy of the Canadian health system and the ministries of health to provide medical care access to all patients, including trauma cases, without billing the patient for resources consumed. This implies that trauma hospitals will invariably incur a financial burden if the ministry of health uses the proposed RIW system for hospital reimbursement. This could lead to increased cutbacks to these hospitals as a financial disincentive, an action that is directly linked to hospital bed closures and job cuts.6
Based on this information, we recommend that the proposed RIW system be utilized for predictable scheduled surgeries but that the RIWs for trauma CMGs be critically appraised. Perhaps another system for hospital reimbursement for these cases could be used, by which the hospital could provide the ministry of health with a more precise estimate of resource consumption by all trauma cases for each fiscal year. In the meantime, to address the dramatic underfunding for trauma cases currently managed by “lead” trauma hospitals, we recommend that the assigned RIW value to trauma CMGs be increased 3.5-fold (to roughly approach resource consumption) and that any current financial incentives for trauma hospitals managing patients in excess of estimated base case load in their global budget also be proportionally increased. There is no doubt that the current strain on health care funding is already at a critical level. This re-evaluation of trauma hospital reimbursements particularly in this area may seem to be a burden to the system. However, the precedence of trauma hospital closures in the US, and the annual operating deficits of “lead” trauma hospitals in Ontario that have resulted in funding cutbacks, bed closures and staff layoffs, makes this re-evaluation essential. Clearly, further accurate case costing studies are required to determine the effectiveness of RIWs in representing the resource consumption in other CMGs.
Footnotes
Presented in part at the annual meeting of the Royal College of Physicians and Surgeons of Canada, Toronto, Ont., Sept. 25, 1998.
- Accepted February 13, 2001.