Abstract
Objective: To find out if the cost of health services was artificially increased because of a delay in surgery due to a lack of resoures.
Design: A retrospective cohort study.
Setting: Three urban hospitals in Calgary, Alta.
Patients: The study cohort comprised 4441 patients (1 index procedure for each patient).
Interventions: Cholecystectomy, discectomy, hysterectomy, total knee and total hip replacements.
Outcome measures: The costs for physician claims, use of home care and pharmaceutical prescriptions 1 year before and after the selected procedures, using 1997/98 administrative records and waiting times maintained by Alberta Health and Wellness and Calgary Regional Health Authority.
Results: The median wait for joint surgery (88 d for knee replacements and 65 d for hip replacements) was longer than for the other selected procedures (29 d for cholecystectomies, 21 d for discectomies and 42 d for hysterectomies). Total per patient physician claim costs decreased after surgery (cholecystectomy — 30%, discectomy — 24%, hip replacement — 6%, hysterectomy — 23% and knee replacement — 4%). Seeing the procedure specialist more than once preoperatively was associated with a greater decrease in postoperative physician claim costs. Longer waits were not associated with more physician claim costs or Blue Cross prescriptions claim costs for seniors (≥65 yr) in the year before or after surgery nor were they associated with more physician claim costs during the actual wait compared with a matched postoperative time period.
Conclusions: No evidence was found to suggest that waiting for 1 of 5 common surgical procedures is correlated with greater health service expenditures pre- or postoperatively. In this study, wait time is not a proxy for health service use nor do health service costs decrease markedly after surgery.
Patients wait for health services when resources are insufficient. Waiting lists do not directly assess the functional impact or distress associated with waiting.1–3 However, just waiting for a therapeutic service such as surgery may have an independent economic effect. If a delay for surgery equates with failed problem resolution, then it is reasonable to hypothesize that additional health services will be required until the definitive surgical service is performed. If this is true, then waiting for therapeutic health services such as surgery may artificially increase overall health service expenditures. If not, the significance of waiting for surgery should be more closely scrutinized.
In this study we compared the use of health services (physician claims, use of home care, length of hospital stay and prescriptions) before and after 5 high-volume surgical procedures, the cost of these services before and after surgery compared with the length of the waiting period, and the cost for physician services during the actual wait minus a matched postoperative period was compared to the length of the waiting period.
Methods
This study compared a 1-year period immediately before and after surgery during the fiscal year 1997/98. The preoperative period began 365 days before each patient’s hospital admission date, and the postoperative period ended 365 days after the hospital discharge date. All physician claims during the procedure hospitalization were excluded.
Patients were included if 1 of 5 specific procedures (hip and knee joint replacements, cholecystectomy, hysterectomy, and discectomy) was performed in any 1 of the 3 Calgary Regional Health Authority (CRHA) hospitals (Foothills, Peter Lougheed Center and Rockyview) during the fiscal year 1997/98. Records were first identified by the clinical modification of the Classification of Diseases, 9th revision (ICD-9-CM) procedure code located within the CRHA inpatient and day surgery databases and retained if an appropriate Canadian Classification of Procedures (CCPx) physician claim (database maintained by Alberta Health and Wellness [AH]) could be located within ± 1 day of the ICD-9-CM procedure service date. The specific coding for procedures is available from the authors.
Patients were excluded for the following reasons:
A personal health number was absent from the original CRHA database or the personal health number could not be converted to an anonymous number linking the CRHA and AH databases.
The patient was not a resident of Alberta at the time of the procedure or death, or migrated into or out of the province in the 3-year period, ascertained by linking to the AH health care recipient registry.
Failure to match the CRHA record of procedure to a physician claim for procedure.
Hospital stay for the procedure was more than 28 days.
Procedures in more than 1 index group (hip and knee joints, cholecystectomy, hysterectomy, discectomy) were performed during the same admission (2 patients).
The same surgery was performed on more than one occasion within the 3-year study period (75 patients).
The outcomes studies were as follows:
Physician claim costs during the year before the procedure, the year after the procedure and the difference between the 2 years.
Length of hospital stay.
Home care estimated costs based on hours of care during the year after the procedure. This measure was derived by linking with the Alberta Home Care database.
Blue Cross prescription dollars claimed during the year before, the year after, and the difference between the 2 years for “seniors” (≥65 yr) with Alberta Blue Cross registration.
The descriptive variables included the following:
Waiting times (date when the CHRA receives a booking request for a specific procedure to the date of hospital admission).
Age and sex of the patient on the date of procedure.
Residence within or out of the CRHA on the date of procedure.
Physician service by general practitioner, service specialist or all other specialists. Service specialist is defined as cholecystectomy — general surgeon, hysterectomy — gynecologist, hip and knee replacement — orthopedic surgeon, discectomy — neurosurgeon. Our methodology for matching procedural specialist to procedure required that the physician specialty was defined and used as the initial matching criterion. During this period, 128 discectomies (32.0% of all discectomies) were attributable to an orthopedic surgeon rather than a neurosurgeon.
Type of physician claim (consultation, procedure or out of hospital diagnostic radiology).
Whether the patient saw the procedure specialist on more than 1 occasion before admission. Procedural physician analysis was restricted to patients for whom a preoperative claim was found for the same physician who submitted a claim for the index procedure.
Total number of ICD-9-CM procedures done and total number of comorbid ICD-9-CM diagnoses during hospitalization for index surgery.4
Surgery priority category (urgent, emergency, elective) as determined solely by procedure physician. The general clinical guidelines for patient categorization is emergent (within 24 h), urgent (within 1 mo) and elective (not emergent or urgent). Category verification or comparability is not validated.
Descriptive statistics and linear regression were used to assess the relation between physician claims and waiting time. Significance was defined as p < 0.05. The SAS version 6.12 was used for analysis.
Results
Of 4391 inpatient episodes and 951 day-surgery episodes that were selected using the ICD-9-CM definition for the 5 procedures, 901 patients were excluded, yielding a final cohort size (1 index surgery for each patient) of 4441. The number of cases, mean age and proportion of women by procedure were as follows: hip replacement — n = 440, 70 years, 68%; knee replacement — n = 303, 70 years, 63%; cholecystectomy — n = 1838, 47 years, 73%; hysterectomy — n = 1460, 46 years, 100%; and discectomy — n = 400, 43 years, 42%.
The CRHA administrative records did not list a wait day for all patients. Cases without wait times were excluded for all analyses requiring wait times as noted by the listed changes in the number for each procedure below. The median wait for joint surgery (298 knee replacements — 88 days, and 313 hip replacements — 65 days) was longer than the 3 other selected procedures (1455 cholecystectomies — 29 days, 352 discectomies — 21 days, and 1406 hysterectomies — 42 days). Although in general average waits decreased from elective to emergent, a wide range in waits was noted for each priority rating (Table 1).
Average (and Range) Waiting and Number of Patients by Booking Priority for the Five Index Procedures
Physician claims
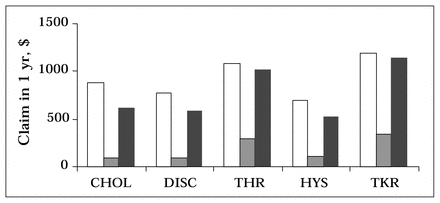
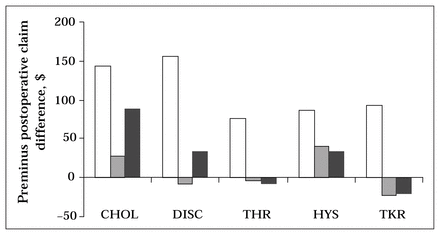
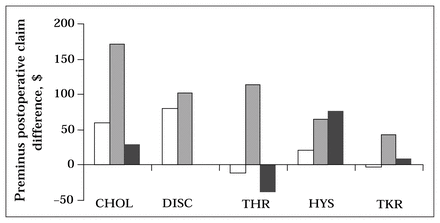
Fig. 1 illustrates the total physician claims per patient before the waiting period, during the waiting period, and after the surgical procedure. For all 5 procedures, total preoperative physician claims per patient decreased after surgery (cholecystectomy — 30%, discectomy — 24%, hip replacement — 6%, hysterectomy — 23%, and knee replacement — 4%). The percentage of preoperative physician claims during the wait varied among procedures. This simply reflected the relative proportion of the preoperative year spent waiting (cholecystectomy — 11%, discectomy — 11%, hip replacement — 27%, hysterectomy — 16%, and knee replacement — 28%). The per patient difference between before surgery and after surgery claims for out-of-hospital diagnostic imaging, procedures, consults, general practitioners and specialists are illustrated in Figs. 2 and 3. Note that differences less than zero represent increased dollar claims after surgery. Claims for consults showed the greatest decrease after surgery (cholecystectomy — 55%, discectomy — 86%, hip replacement — 119%, hysterectomy — 54%, and knee replacement — 189%). Claims for all non-service specialists showed the greatest decrease after surgery (cholecystectomy — 77%, discectomy — 56%, hip replacement — 118%, hysterectomy — 87%, and knee replacement — 106%). Claims for the service specialists did not show a consistent decrease after surgery (cholecystectomy — 11%, discectomy — 0%, hip replacement — gain of 59%, hysterectomy — 47%, and knee replacement — 18%).
Total physician claims per patient before and after (black bars) surgery, excluding all claims during hospitalization for the surgical procedure. The preoperative period comprises the period before wait (white bars) and during wait (shaded bars). CHOL = cholecystectomy, DISC = discectomy, THR = total hip replacement, HYS = hysterectomy, TKR = total knee replacement.
Type of pre- and postoperative physician claims: consult (consultation) (white bars); procedure (shaded bars); diagnostic (out of hospital diagnostic radiology) (black bars). CHOL = cholecystectomy, DISC = discectomy, THR = total hip replacement, HYS = hysterectomy, TKR = total knee replacement.
Pre- and postoperative physician claims by type of physician: general practitioner (white bars); service specialist (black bars); all other specialists (shaded bars). Service specialist was defined as a general surgeon for cholecystectomy, a gynecologist for hysterectomy, an orthopedic surgeon for hip and knee replacements, and a neurosurgeon for discectomy. CHOL = cholecystectomy, DISC = discectomy, THR = total hip replacement, HYS = hysterectomy, TKR = total knee replacement.
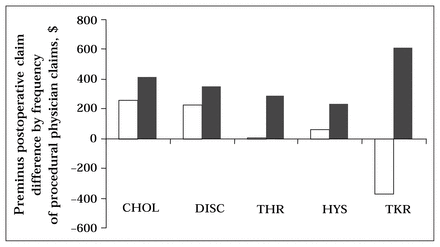
We attempted to identify at least 1 preoperative claim by the physician who did the procedure. The number of patients for whom a procedural physician preoperative claim was found and frequency of more than 1 preoperative claim by that physician was as follows: cholecystectomy (n = 1323, 20%), discectomy (n = 262, 19%), hip replacement (n = 278, 35%), hysterectomy (n = 1334, 56%), and knee replacement (n = 280, 42%). The difference (in Canadian dollars) between before and after surgery claims per patient were consistently greater if the procedure specialist was seen on more than 1 occasion preoperatively (Fig. 4): cholecystectomy — $159, discectomy — $125, hip replacement — $284, hysterectomy — $178, and knee replacement — $982. The dollar difference for the 5 procedures was still greater if the procedure specialist was seen on more than 1 occasion even after eliminating all claims by the procedural doctor: cholecystectomy — $90, discectomy — $8, hip replacement — $83, hysterectomy — $83, and knee replacement — $587.
Difference between before minus after surgery total physician claims per patient. Patients who saw the procedural physician only once during the preoperative period (white bars) are compared with those who saw the procedural physician multiple times during the preoperative period (black bars). Note that dollar amounts are not directly comparable with Fig. 1 as at least 1 preoperative claim by the procedural physician was not identified in 964 of the 4441 total cohort. CHOL = cholecystectomy, DISC = discectomy, THR = total hip replacement, HYS = hysterectomy, TKR = total knee replacement.
Home care
Postoperative home care was provided to some patients. Their number and attributed costs were as follows; cholecystectomy (n = 98, $840); discectomy (n = 26, $407); hip replacement (n = 214, $1368); hysterectomy (n = 104, $521); and knee replacement (n = 124, $822).
Blue Cross
The administrative databases for Alberta Blue Cross are predominately restricted to seniors. The study was limited to claims from Blue Cross, universally available to all seniors in Alberta (age ≥65 yr). The analysis was restricted to all seniors who made claims before or after an index procedure. Seventy-seven percent of 1054 seniors who underwent 1 of the 5 index procedures submitted Blue Cross prescription claims in the pre- or postoperative period (cholecystectomy — 79%, discectomy — 81%, total hip replacement — 74%, hysterectomy — 77%, and knee replacement — 77%). The preoperative cost and cost difference of before minus after surgery for prescription claims were cholecystectomy (n = 262, $744, +$26), discectomy (n = 22, $819, −$158), total hip replacement (n = 236, $1015, −$53), hysterectomy (n = 109, $575, +$193), and total knee replacement (n = 180, $950, +$53).
Hospital stay
The mean (and range) hospital stay in days was cholecystectomy (n = 954, 4.0 [1–28]), discectomy (n = 400, 4.2 [1–24]), total hip replacement (n = 214, 8.9 [3–28]), hysterectomy (n = 104, 3.6 [1–23]), and total knee replacement (n = 124, 7.4 [3–27]).
Waiting time
The determinants of waiting time were modelled by multiple regression. The independent variables in the model were age, sex, emergent surgery, urgent surgery, number of comorbid diagnoses and procedures during hospital stay, length of hospital stay, hospital (1 of 3 sites), residence in the CRHA, and “saw procedure doctor on more than 1 occasion” preoperatively. The model explained up to 37% of the variance in wait days. Emergency surgery, urgent surgery, “saw procedure doctor on more than 1 occasion,” and length of hospital stay were inversely associated with waiting time (i.e., all these categories were associated with less wait).
Table 2 illustrates the average daily cost of physician claims in the year before and year after surgery. The effect of wait on the dependent variables of total 1-year physician claim costs (preoperative, postoperative, and preoperative minus postoperative) was modelled by multiple regression for each procedure. Regressions were reported on all patients with a defined waiting time and preoperative claim by the procedural doctor (n = 3080). The independent variables were waiting time, “saw procedural doctor on more than 1 occasion,” age, sex, surgery priority, number of ICD-9-CM procedures and diagnosis.
Average Daily Cost (Canadian Dollars) of Physician Claims in the Year Before and Year After Surgery for the Five Procedures
Tables 3 and 4 illustrate the dollar increase in physician claims for each day of waiting and dollar increase in physician claims if the patient saw the procedural physician on more than 1 occasion. Waiting time was only weakly and inversely correlated with total physician cholecystectomy claims; longer waits resulted in lower expenditures. “Saw procedural doctor on more than 1 occasion” was strongly positively correlated (longer waits resulted in higher expenditures) with preoperative claims in all 5 index procedures, postoperative claims in cholecystectomy and total knee replacement as well as the preoperative minus postoperative differences for hysterectomy and total knee replacement. A similar pattern was noted if claim dollars were restricted to those by the procedural physician (Tables 5 and 6). Waiting time was only weakly and inversely correlated with total physician hysterectomy claims; longer waits resulted in lower expenditures. “Saw procedural doctor on more than 1 occasion” was strongly positively correlated (longer waits resulted in higher expenditures) with preoperative, postoperative, and preoperative minus postoperative difference for all 5 index procedures. All models’ variance explanation was uniformly low at no more than 10%.
Increase in Physician Claims (Canadian Dollars*) by Increase in One Day of Waiting Time for the Five Procedures
Increase in Physician Claims (Canadian Dollars*) if the Patient Saw the Procedural Physician More Than Once Preoperatively*
Increase in Procedural Physician Claims (Canadian Dollars*) by Increase of One Day in Waiting Time
Increase in Procedural Physician Claims (Canadian Dollars*) if the Patient Saw the Procedural Physician More Than Once Before Admission
Emergent and urgent surgery was not significantly associated with physician claims in the multiple linear regression analysis. We did not note any material changes in our results by separating the analysis by elective and urgent or emergent patients. We also attempted to define elective and urgent by elapsed time between booking date and surgical date (i.e., 1 or 7 d). The constructed or actual categorization of elective and emergent or urgent surgery did not materially influence the multiple regression model of physician costs, and these data are not shown.
To assess the importance of the time period chosen on the association of wait and total physician claims we did the following: (1) restricted cases to those with waits up to 250 days (to minimize the influence of those patients with longer waits who would likely have had more claims during the longer wait within a fixed 1-yr period); (2) restricted claims to those during the actual wait period (in this manner assessing the influence of claims that were made only after the booking date). The duration of waiting was not significantly associated with preoperative, postoperative, and preoperative minus postoperative difference in all 5 index procedures when the time period was restricted to 250 days. To assess the association of wait with physician claims restricted to the actual wait period, we subtracted the waiting time physician claims from physician claims in an identical postoperative time period matched for each patient. In this manner we were able to control for the increase in claims for any given increase in time in which claims were summed. The duration of wait was not significantly associated with preoperative minus postoperative difference in all 5 index procedures when the time period was restricted to the waiting period alone.
Waiting time did not correlate with Blue Cross prescriptions claims for seniors. It was inversely correlated with hospital length of stay (less wait, longer hospital stay). Waiting time was inversely correlated to home care costs (longer waits associated less with home care costs) in those patients who underwent total hip replacement.
Discussion
We found that physician claim costs for health services decrease by no more than 30% after 5 common surgical procedures. Postoperative physician claim costs remain higher in older patients receiving joint replacement. We found no evidence to suggest that waiting for surgery is correlated to greater expenditures pre or postoperatively (physician claims, home care, and Blue Cross prescriptions for seniors). Repeated preoperative visits to the procedural physician were correlated to a greater decrease in postoperative physician claim costs.
Preoperative physician claims are a mixture of payments for care unrelated to the problem requiring surgery, care related to making the diagnosis in which surgery was recommended, and claims for care that may have been potentially avoided if earlier surgery had been done. Postoperative physician claims are payments for postoperative care (not bundled into the operative claim that was excluded from these analyses) and care unrelated to the problem requiring surgery. There was no consistent change in claim costs during the preoperative wait compared with preoperative claim costs prior to waiting. As claim costs summed over an increased time are greater, we compared pre- minus postoperative claim costs for fixed periods. Our results were robust for all the time periods we counted physician claim costs (1 yr in those with waits up to 1 yr, 1 yr in those with waits up to 250 d, only the wait period for each patient). We found a weak inverse relationship, with longer waits correlating with less (not more) perioperative claim costs. Although we have no information on the health status of those who waited, any potential health status change while waiting did not translate into a measurable increase in health service consumption. Thus, those who wait the longest may have a course of illness quite different from those who wait the shortest.
The number of patients on surgical waiting lists and the length of time they wait can be used as performance indicators and have been drivers of health resource allocation.5–8 Increasing the number of services may not improve the waiting times or decrease wait-list size.5–7 Patients on waiting lists have their needs assessed by individual clinicians. No attempt is made to balance the effectiveness of the specific intervention for one particular patient compared to providing another type of service to someone else.9 Focus on the target of wait time may divert attention from the quality, effectiveness and appropriateness of the health service. 10 Differences in urgency, case severity, telephone access, or physician and patient personal values influence how long a patient waits.11–14 The important issues about the delay to surgery are those of equity (everyone waits equally), prioritization (those who need most receive first), and societal costs of waiting (cost of suffering, lost wages).15–17
Wait lists are not simple queues.17 They contain patients who have died, no longer require the service, obtained the service elsewhere, or self-deferred the service for convenience. 6 Wait times are affected both by the time limitations of those providing the service as well as the availability of resources. In the case of the typical single physician wait list, wide discrepancies exist in wait times among physicians providing the same service.15 In this study, waiting decreased with multiple preoperative claims by the procedural physician despite the obvious need for time to elapse between procedural physician claims. Physicians prioritize patients on multiple occasions and in so doing likely limit the wait and potential claims due to delayed surgery. The categories of emergent and urgent surgery were derived at the initial time of booking, so we cannot assess if those with longer waits require more emergent or urgent surgery. Shorter length of stay in those with longer waits agrees with our other results in that these long-wait patients do not consume more health resources and may be less disabled than those with shorter waits.
Deciding when the clock starts for wait lists is problematic. Patients present a problem to a health worker; they may be referred to other health workers, and at some time along this path a decision may be made to recommend surgery.15,16 From the patient’s perspective, waiting begins with the problem. However, the link between the problem and the recommendation for surgery may vary among patients. The time of surgical booking is used as the wait time start, allowing a common, comparable reference point.1,3,5,12,13 However, wait time and resources may have been consumed prior to the surgical booking. We attempted to address this by comparing individually fixed time intervals before and after each procedure. In this manner, costs before the decision to have surgery were also analyzed.
The wait list is used to argue for more resources.16 In this study, wait time is not a proxy for future health service use. Wait time does not estimate need.8,15–19 It is likely that patients’ self-reports of need on wait lists will be influenced if patients know these self-reports are used to prioritize queue rank.20,21 The validity22 and reliability of priority tools23 may be insufficient for use within any one health service and are probably not a realistic way to prioritize between health services (in this manner they indirectly determine relative health service rates). A successful example of a wait list management program for one procedure (Ontario Cardiac Care Network24) may not be generalizable because of some unique features (strong anatomical determinants for priority setting, priority not determined by operating surgeon, pooled surgical referrals). The absence of successful models has in part prompted 2 new initiatives — The Western Canada Wait List Project and the Ontario Wait List Project.
Then how should resource allocation for different health services be determined? We argue that repeated visits to the procedural physician is a better indicator of future decrease in physician claims. Unlike wait lists in which patients may be placed and passively remain indefinitely15 (up to nearly 2 yr in this study), repeated physician visits require active involvement by both physician and patient. Unfortunately, repeated visits are no less immune to gaming than wait lists. We hypothesize that there exist potentially more useful markers for determining the relative resource allocation between services and the subsequent relative health service rates24 (prevalence of the condition,25 health burden of disease,26 potential of successful intervention).
This cost analysis was done from the payer perspective. A cost analysis from the societal perspective should include direct and indirect cost for patients and their families. Our ability to cost the waiting burden is limited. Patient’s return to income production is not a major factor for many patients after procedures like coronary artery bypass surgery.27 Experiencing significant difficulty in carrying on their work or daily duties as a result of their medical condition was noted in only 14% of patients who underwent gynecologic surgery.28 Improved quality of life after surgery has been noted after hip and knee replacements2 and a decreased quality of life experienced while on the wait list for coronary artery bypass surgery.3 However, patient satisfaction is contextual and not well correlated to actual length of wait.29 Patients’ own perceptions of their burden and ability to tolerate delayed relief is a consideration when assessing data from health-related quality-of-life measurement.1 When the tolerance of delay is measured as willingness to pay, the majority of patients were unwilling to pay out of pocket to lessen the delay for cataract surgery.30 Given these complexities and the difficulty of societal cost assessment, we elected to assess the cost of delay more narrowly by measuring the incremental cost of health services related to the delay of surgery. The proxy measurement of prioritization “repeated visits to procedural visit” may have limited the cost of delay by selecting patients with greater severity or at least patients or physicians who perceived the disease to warrant more immediate attention. Using repeated visits for prioritization may be inequitable. However, explicit prioritization tools23 or guarantee of maximum wait31 may not be superior in actual practice. Given the difficulty of measuring costs from the societal perspective, our results showing no effect from the payer perspective, and the persistent existence of a wait problem in multiple countries for decades,28 we do not believe that focusing on wait time costing is critical in solving the wait problem.
There are a number of limitations to this study. Physician activity was expressed in claim dollars. This is an appropriate economic metric but may not capture physician–patient interaction given the fee schedule peculiarities translating physician work to claim dollars. All physician claims and Blue Cross prescriptions were pooled since no reliable method exists to separate those claims that only pertain to the specific surgery. As such, we are unable to distinguish those drug costs that correspond to unrelated comorbidity. There are 2 methods by which wait lists can be analyzed: cross-sectional (all patients at a point in time as was done in this study) and longitudinal (follows patients over time). Although cross-sectional analysis is the most common, this method overestimates actual wait time due to sampling errors.32 Secondary use of administrative data should be interpreted with caution. We were able to cross-validate both wait time and index surgical procedure using independent databases. Our measure of comorbidity was crude and unlikely to faithfully capture either case severity or comorbidity.4
Acknowledgements
We thank the Calgary Region Health Authority and Alberta Health and Wellness for providing access to their administrative records. This work was partially supported by the Alberta Centre for Health Service Utilization Research. The opinions and conclusions expressed in this paper are those of the authors and no endorsement by the Alberta Department of Health & Wellness or Calgary Regional Health Authority is implied.
Footnotes
Reprint requests to: Dr. Hude Quan, Department of Community Health Sciences, University of Calgary, 3330 Hospital Dr. NW, Calgary AB T2N 4N1; fax 403 270-7368, hquan{at}ucalgary.ca
- Accepted July 27, 2001.