Abstract
Objectives: To estimate the costs of Canadian pediatric trauma and identify cost predictors.
Design: A chart review.
Setting: A regional trauma centre.
Study material: The charts of all 221 children who suffered traumatic injuries with an Injury Severity Score (ISS) of 4 or more seen over 6 years at a regional trauma centre.
Main outcome measures: Patient data, injury data, all hospital-based costs, excluding nursing, food and medication costs.
Results: Mean (and standard deviation) patient age was 12.8 (5) years. Sixty percent were boys. Motor vehicle accidents (MVAs) accounted for 71% of the injuries, followed by falls (11%). The mean (and SD) total cost of care was Can$7582 (Can$12 370), and the cost of media was Can$2666. Total cost correlated directly with age (r = 0.29, p < 0.001) and Injury Severity Score (ISS) (r = 0.34, p < 0.001) and inversely with the Pediatric Trauma Score (PTS) (r = −0.20, p = 0.003). The presence of extremity injuries correlated significantly with total cost (r = 0.22, p = 0.001) and PTS (r = −0.25, p < 0.001) but not with the ISS. Logistic regression analysis identified runk injury, ISS and PTS as the main determinants of survival.
Conclusions: The cost of pediatric trauma in Canada can be predicted from admission data and trauma scores. The cost of extremity injuries is significant and can be predicted by the PTS but not the ISS.
Traumatic injuries are the leading cause of death in children.1 In order to predict mortality and to better allocate hospital resources, numerical trauma scores were devised. Several such scores now exist, each differing in the factors included. Examples are the Injury Severity Score (ISS),2 Abbreviated Injury Score (AIS),3 Revised Trauma Score (RTS),4 Pediatric Trauma Score (PTS),4,5 APACHE II score,6 A Severity Characterization of Trauma (ASCOT)7 and the Trauma and Injury Severity Score (TRISS).8
In addition to potentially devastating medical and emotional effects, traumatic injuries are accompanied by a significant consumption of health care resources. Several studies have examined the costs of pediatric trauma, and found compensation to health care providers to be adequate in the United States.9,10 Equivalent studies in Canada are lacking. In this study, we sought to estimate the cost of Canadian pediatric trauma care and determine any predictors of higher cost and resource use.
Patients and methods
The charts of children (under 18 years of age) suffering traumatic injuries with an Injury Severity Score (ISS) of 4 or more, admitted to a Canadian regional trauma centre between Apr. 1, 1991, and Mar. 28, 1997, were reviewed. The ISS of 4 or more was used to limit the series to significant injuries.11,12 Patients with incomplete charts were excluded from the study.
A list of eligible patients was generated using our institution’s trauma database. Charts were reviewed for demographic information. including gender, date of birth, date of injury, mechanism and body region of injury. The ISS had been prospectively recorded in the trauma database. Components of the Pediatric Trauma Score (PTS)5 (blood pressure, weight, presence of open wounds or fractures, airway and neurologic status) were collected from charts retrospectively.
Operative records were reviewed for timing and duration of operations as well as procedures performed. Total cost of surgical care was determined as follows: (hourly operating room rate × operating room time) + (hourly anesthesia rate × anesthesia time) + recovery room cost + surgeon’s initial assessment + cost of all procedures.
Postanesthesia time in the recovery room was estimated at 1 hour for all patients, which has been shown to closely approximate actual times (K. Hawley, K. Fern, T. Smith, B. Zee, D. Pichora: unpublished data).
Charts were also reviewed for resource use. This included the use of blood products, days spent on mechanical ventilation, and length of stay in the intensive care unit, neonatal intensive care unit and regular ward. All the costs included represented charges rather than real costs since the former are the only ones commonly available. Hospitalization costs did not include nursing, allied professionals’ costs, physiotherapy, occupational therapy, etc., food and medication costs. Nursing, allied professionals’ costs and food costs were unavailable. Costs for medications were not included because it has been shown that they have a negligible impact on overall costs (K. Hawley, K. Fern, T. Smith, B. Zee, D. Pichora: unpublished data).
Statistical analysis included descriptive statistics of all demographic variables. Pearson’s correlation and Spearman’s rank correlation were used to examine the relationship between cost of care and various patient variables. Analysis of variance (ANOVA) was used in identifying significant trends in the characteristics of injuries by mechanism and body site. Stepwise logistic regression analysis was carried out, using survival as the dependent outcome variable. The logistic regression equation has the following form:
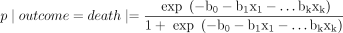
where p = probability; exp = natural logarithm; b0, b1 … bk equal coefficients to be estimated; x1, x2 … xk equal independent variables. Starting with a constant model having b0 as the only parameter, variables were entered into the equation only if their addition increased the likelihood of the model by a significant p value using 2-tailed test of significance.13
Data were stored on Excel spreadsheets. All analyses were performed using SPSS for Windows software version 7.5 (SPSS, Chicago). α was set at 0.05.
Results
The study group comprised 223 children. Two children with incomplete records were excluded. Of the 221 children injured, 132 (59.7%) were boys. Motor vehicle accidents (69.8%) were responsible for most accidents, followed by falls (11.1%), sports injuries (4.9%), bicycle accidents (2.2%) and child abuse (1.3%). Other mechanisms (including gunshot wounds, injuries involving trampolines, horses, cows, dog bites, diving and toboggan injuries) accounted for the remaining 10.7% of injuries.
The mean (and standard deviation) patient age was 12.8 (5) years, median 14 years. The age was also considered according to mechanism of injury (Table 1). The trauma scores and body sites injured are also shown in Table 1. ANOVA showed that the differences in all of these variables by mechanism of injury were statistically significant. Table 2 shows the relationship between mechanism of injury and the hospital stay and costs. The longer hospital stay and associated higher cost of MVAs is apparent.
Patient Variables by Mechanism of Injury in Children Who Suffered Trauma
Length of Hospital Stay and Hospital Costs According to Mechanism of Injury
The percentage of children injuring each body region was calculated. In our sample 71.5% of children had a head injury, 39.5% injured their trunk, 20% sustained upper extremity injuries and 24% lower extremity injuries. There were 19 trauma-related deaths in our study, giving a mortality of 8.6%.
The breakdown of total hospital costs is shown in Table 3. The total direct costs for our sample was Can$1 675 734. The mean cost per patient was Can$7583 ($12 370). The median cost, however, was only Can$2666. The costs for MVAs were significantly higher than for other injury types (Table 2).
Breakdown of Total Hospital Costs for Children Admitted to Hospital With Traumatic Injuries
The mean cost for the 19 children who died was Can$8659, an amount not statistically different from that for the 202 children who survived.
Total cost correlated significantly with age (r = 0.29, p < 0.001), ISS (r = 0.34, p < 0.001) and PTS (r = −0.20, p < 0.003). The mean cost for children with an ISS of 12 was Can$11 006 whereas the cost for those with an ISS less than 12 was Can$1778 (p < 0.001). Extremity injury correlated with total cost (r = 0.22, p < 0.001) and PTS (r = −0.25, p < 0.001) but not ISS. Injuries to other body components did not influence the cost.
Finally, by logistic regression analysis, performed using survival as the dependent outcome variable, 96.8% of possible outcomes were correctly predicted by an equation including the following 3 factors: PTS (p = 0.0005), ISS (p = 0.0065), and trunk injury (p = 0.0046). The equation has the following form:
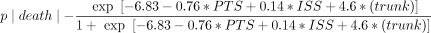
where “trunk” equals 1 if truncal injury was present and 0 if it was not.
Discussion
Trauma is a significant cause of morbidity and mortality in children, and as such it has received much attention in the literature. The demographic profiles of pediatric trauma in the literature show considerable variation. In our study, 60% of children were male, consistent with other reports suggesting a preponderance of boys, ranging from 58.8% to 78.4%.10,14–17 Most injuries in our series were due to MVAs (69.8%), a pattern that is mostly supported by the literature,18–21 although some studies identify falls as the most frequent cause of injury.1,17,21 The noteworthy absence of penetrating trauma in our series reflects the Canadian non-metropolitan setting of the study. The average age of patients in our study (12.8 years) was slightly higher than that found in other studies.10,15,19 Differences in trauma centre referral patterns and characteristics of the populations at risk may account for these differences. The breakdown of injuries by body site shows an overwhelming representation of head injuries, a pattern consistent with the reports in the literature.21 The death rate of 8.6% in our series is slightly higher than that usually reported.17,19
Resource consumption by pediatric trauma is a critical factor in resource allocation and the provision of health care. Trauma costs can be divided into direct and indirect costs. Direct costs include goods and services used to treat the actual injury, such as the cost of hospital stays, doctors’ fees and medications. Indirect costs relate to goods and services lost due to injury or disability. 22 The latter are more difficult to quantify because by definition they deal with potential rather than incurred losses. Several studies have attempted to quantify indirect costs, estimating them in the United States at $5.4 billion yearly, with total (direct and indirect) trauma costs exceeding $7 billion.22,23
The current study was concerned only with direct costs. Reports of direct costs in the literature range from $5000 to $25 000 per hospital stay.9,10,14,18,19,24 Our mean value of total costs per patient (Can$7582) is at the lower end of this range, consistent with the pattern of lower health care costs in Canada.9,10,12,18,21,23 It should be noted, however, that direct comparisons of cost are difficult because of the variability in inclusion criteria. The compensation mechanism in Canada is provincial, and in Ontario involves lump-sum transfers from the Ministry of Health to treating institutions based on an ISS bracket. The current formula in Ontario funds pediatric trauma only for an ISS of 12.25 The actual funding per case varies each year, although it usually approximates Can$15 000. This amount is slightly higher than our estimated cost of Can$11 000 for each patient with an ISS of 12, although our costs are noninclusive and therefore underestimate true costs to the institution. Based on this same formula, our study group would have generated Can$2 085 000 in ministry funding (139 children had an ISS of 12). This amount compares favourably with the total cost estimated at Can$1 675 734, albeit being rather insensitive to individual cases.
As expected, both trauma scores showed significant correlations with total cost in our study. A similar pattern of increasing costs with higher ISS scores has been reported.9 In our study, the PTS appeared to be a slightly poorer predictor of cost than the ISS, despite previous reports showing their equivalence.16 The PTS did, however, correlate strongly with the presence of extremity injuries. This may be owing to the inclusion in the PTS of a category for fractures and lacerations. The ISS considers only the most severely injured body region, potentially missing extremity injuries. Our observation that increasing age correlated with increasing cost is also supported by the literature. 14 This may reflect the higher frequency of resource-intensive MVAs in the older age group.
An analysis of our data revealed the prominence of MVAs in terms of both severity of injury and cost of care. Children involved in MVAs tended to have more body regions injured, lower PTS and higher ISS scores. They had longer stays in hospital and had significantly higher costs than other patients. Intuitively, these patients tended to be older.
Head injuries were very common in our study, yet their presence did not appear to have an impact on the cost of care. This may be the result of the common finding of associated injuries in head trauma patients and the nondiscriminating effect of head injury compared with the other injuries. The presence of truncal or extremity injuries on the other hand did have an impact on the total cost. This is evidenced both by the statistically significant correlations and by the inclusion of trunk injuries in the logistic regression equation. Truncal injuries, such as chest trauma or solid visceral rupture, are often critical injuries carrying significant morbidity. Extremity injuries often require surgical interventions and prolonged hospital stay. Results from our centre have shown that patients with injuries to multiple extremities require surgical intervention in 86% of cases and their cost of care is nearly 3 times greater than for other trauma patients (K. Hawley, K. Fern, T. Smith, B. Zee, D. Pichora: unpublished data).
There are several limitations to the current study. The study sample is relatively small and is limited to one particular trauma centre. Other trauma centres, especially if located in different geographical settings (e.g., metropolitan areas), may have a different population of injuries and therefore different costs. The costs derived are clearly underestimates, as important components of the hospital stay could not be included in the calculations, for practical reasons. Finally, the cost estimates cover only the initial hospital admission, which naturally reflects only a fraction of the total, long-term cost of each injury to society.
Conclusions
Canadian pediatric trauma carries a significant cost, which correlates with trauma scores, age and body region injured. Resource allocation may be enhanced if all of these factors are taken into account. Further studies are required to explore the long-term costs after pediatric trauma in the Canadian setting.
- Accepted January 20, 2000.









