Abstract
The diagnosis of mesenteric ischemia is based on acute clinical awareness of the condition and confirmed by angiography or laparotomy. The standard treatment is abdominal exploration with resection of the gangrenous segment of the bowel or embolectomy of the superior mesentery artery, or both. Alternative treatment such as intra-arterial thrombolysis may be considered in selected patients. A 66-year-old man with a history of atrial fibrillation presented with abdominal pain. Angiography documented an embolus in both the ileocolic artery and a branch of the right renal artery. The patient was treated with selective intra-arterial infusion of streptokinase. The abdominal pain resolved. Repeat angiography showed lysis of both emboli.
For a small but significant number of patients with intestinal ischemia no salvage procedure is possible by the time the diagnosis is made. On the other hand, no clear management guidelines are available for patients who have intestinal ischemia but viable intestine. Close monitoring, exploratory laparotomy and interventional radiologic techniques have been advocated for the management of such patients.
Recently, thrombolytic therapy has been used in a selected group of patients with intestinal ischemia, but data are lacking on the therapeutic efficacy of the technique and its potential complications. We report the outcome of a patient with intestinal ischemia who was treated with a thrombolytic agent.
Case report
A 66-year-old man, with a long history of paroxysmal atrial fibrillation, presented to the local hospital with a 6-hour history of severe right lower quadrant pain associated with nausea but no vomiting. Five days earlier he had undergone successful cardioversion and was taking warfarin at the time of discharge. His surgical history included a cholecystectomy and an appendectomy and his medical history included hypertension and ischemic heart disease for which diltiazem hydrochloride and sotalol hydrochloride had been prescribed.
On admission to this hospital the patient was in mild distress. The pulse rate was irregular, at 120 beats/min and the blood pressure was 150/100 mm Hg. Cardiac examination showed absence of S1 but normal S2 heart sounds. On abdominal examination there was localized tenderness in the right lower quadrant but no guarding. The abdomen was not distended, there was no guarding or rigidity and bowel sounds were present. Rectal examination yielded no pathological findings.
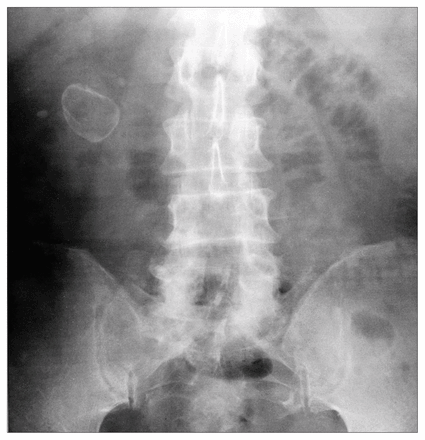
Laboratory investigations included a leukocyte count of 13.6 × 109/L, a hemoglobin level of 13.5 g/L, an international normalized ratio (prothrombin time) of 1.2 and a partial thromboplastin time of 28 seconds. Details of arterial blood gases were as follows: pH 7.38, Pco2 30 mm Hg and Po2 73 mm Hg. An abdominal x-ray film showed a large renal calculus (Fig. 1), and there was no free air under the diaphragm or evidence of a localized ileus. Urinalysis revealed microscopic hematuria.
Supine abdominal x-ray film shows large right renal calculus.
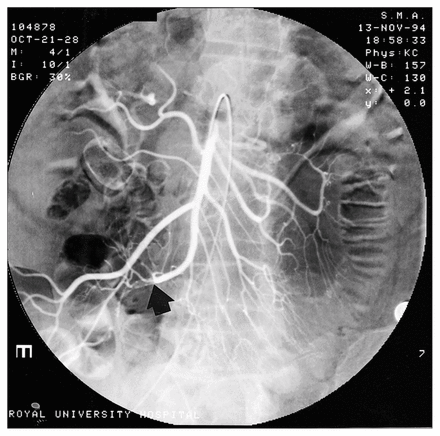
Given this patient’s history, our differential diagnosis included intestinal ischemia. The patient therefore underwent selective angiography 2 hours after admission. This revealed a 3-cm intraluminal defect in the ileocolic artery, consistent with an embolus. There was, however, flow around the filling defect (Fig. 2).
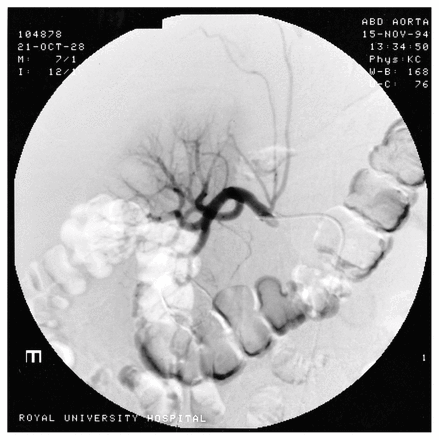
Selective superior mesenteric angiogram shows embolus (arrow) in distal portion of ileocolic vessel.
In an attempt to dissolve the embolus, a bolus injection of 5000 units of streptokinase was given by infusion through the catheter into the ileocolic artery. This was followed by infusion of 36 mg of papaverine over 20 minutes, and an additional 72 mg were injected 2 hours later over a period of 1 hour. The patient received a maintenance dose of streptokinase for 12 hours (5000 units/h), and this was followed by intravenous administration of heparin.
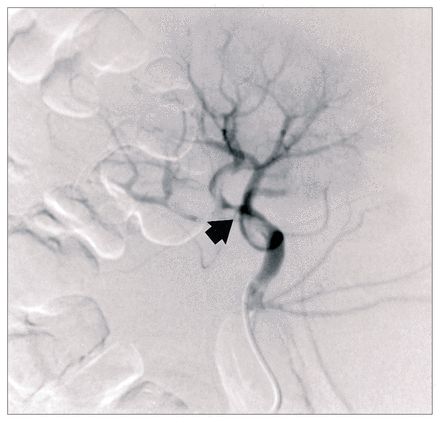
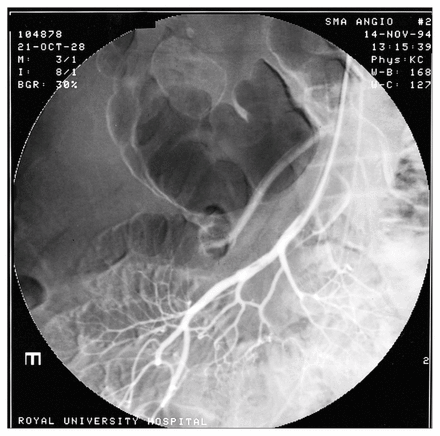
After the procedure the patient remained stable and his abdominal pain was less severe. The following day, however, he complained of right flank pain associated with hematuria. Although a calculus was evident in the right kidney on a plain abdominal film, we considered that another embolic episode was likely to be the cause of the pain, so angiography was repeated. This showed a filling defect in the inferior branch of the right renal artery (Fig. 3) and confirmed the patency of the previously treated ileocolic artery (Fig. 4).
Selective angiogram of right renal artery showing embolus (arrow) in branch of right renal artery.
Selective superior mesenteric angiogram after 18 hours of treatment with streptokinase, showing improved flow through vessel and nearly complete lysis of embolus.
Right renal artery infusion of streptokinase (5000 units/h) was given for 12 hours, after which angiography was repeated. This revealed complete dissolution of the embolus. At the same time the patient’s flank pain resolved completely. The patient was then started on a regimen of intravenously administered heparin. He had no further episodes of abdominal pain. Repeat angiography showed patency of inferior branch of the right renal artery (Fig. 5). He was discharged home 10 days after admission, feeling well and on a normal diet. Although he remained free of abdominal pain he died of a massive myocardial infarction 2 months after discharge.
Selective angiogram of right renal artery after 12 hours of streptokinase treatment. Lysis of embolus and improved flow are noted in previously embolized branch to inferior pole of kidney.
Discussion
Essential to the early diagnosis and successful outcome of mesenteric ischemia is acute clinical awareness of the condition in patients admitted with acute onset of abdominal pain in association with a compatible history. The diagnosis is confirmed either at laparotomy or by angiography. The various causes underlying mesenteric ischemia and the associated pathophysiologic effects have been reviewed.1
There is little disagreement as to the management of patients who present with unequivocal signs of intestinal gangrene. On the other hand, there is no consensus on the investigation and treatment of patients who present with intestinal ischemia associated with a viable intestine. For such patients angiography may have a therapeutic as well as a diagnostic role, as illustrated by our patient.
Thrombolytic therapy in the management of intestinal ischemia was first reported by Jamieson, Thomas and Cade,2 with the successful infusion of streptokinase directly into the superior mesenteric artery. Flickinger and associates3 successfully dissolved a superior mesenteric artery embolus with the intra-arterial infusion of 5000 units/h of streptokinase for 3 hours. Hillers and associates4 used a higher dose of streptokinase (10 000 units/h) infused for 60 hours. Pillari and colleagues5 dissolved emboli in the celiac and superior mesenteric arteries by simultaneous catheterization of those vessels. Although only anecdotally documented, many authors recommend the use of vasoactive drugs, such as papaverine, after the lysis of the thrombus by streptokinase.
Our patient differed from the patients in the reports cited above in that the embolus occluded a branch rather than the main trunk of the superior mesenteric artery. Several questions arise from the management of this case. First, although we believe that the symptomatic improvement of our patient was the direct result of thrombolysis, we cannot be certain that the same effect might not have occurred spontaneously and soon enough before the development of irreversible ischemic changes. Indeed, the fact that there was blood flow around the embolus makes such an outcome a distinct possibility. Second, although the incidence of multiple extramesenteric emboli in patients with embolic occlusion of the superior mesenteric artery can be as high as 50%,6 we cannot exclude the possibility that the embolic occlusion of the inferior branch of the right renal artery in our patient was not a complication of the thrombolytic therapy aimed at the ileocolic artery. This possibility reflects on the lack of standardized regimens for the thrombolytic therapy of intestinal ischemia. Moreover, the evidence in support of the use of vasodilatory drugs remains weak. Third, it is noteworthy that although our patient responded promptly to the treatment, no data exist as to the optimal time that one should wait for a therapeutic effect before resorting to surgical treatment.
In this report we have presented evidence that patients with angiographically demonstrated intestinal ischemia not associated with diffuse peritonitis may be considered for thrombolytic therapy in the absence of the general contraindications for such therapy. Careful patient monitoring, however, is essential to this form of treatment, and if the patient’s symptoms worsen during thrombolytic treatment or if the patient fails to respond to the treatment promptly, laparotomy should not be delayed.
Acknowledgments
We thank Dr. Nicholas Hadjis for his critical editing of this paper.
- Accepted June 21, 1995.